Are you hesitant about getting dental implants because of diabetes? We uncover the myths and facts regarding diabetic implant procedures. Learn how thorough blood sugar management and systematic clinical protocols can raise the success rate of diabetic dental implants to 95%.
"Is it okay to get implants even though I have diabetes?"

This is one of the most frequent questions I hear in the consultation room. Many patients with diabetes hesitate, filled with worry and anxiety before deciding on the procedure. Having encountered countless diabetic implant patients, I fully understand your concerns. However, please do not worry. With accurate management and systematic preparation, success is well within reach for diabetic patients.
1.Is Getting an Implant Truly Dangerous If You Have Diabetes?
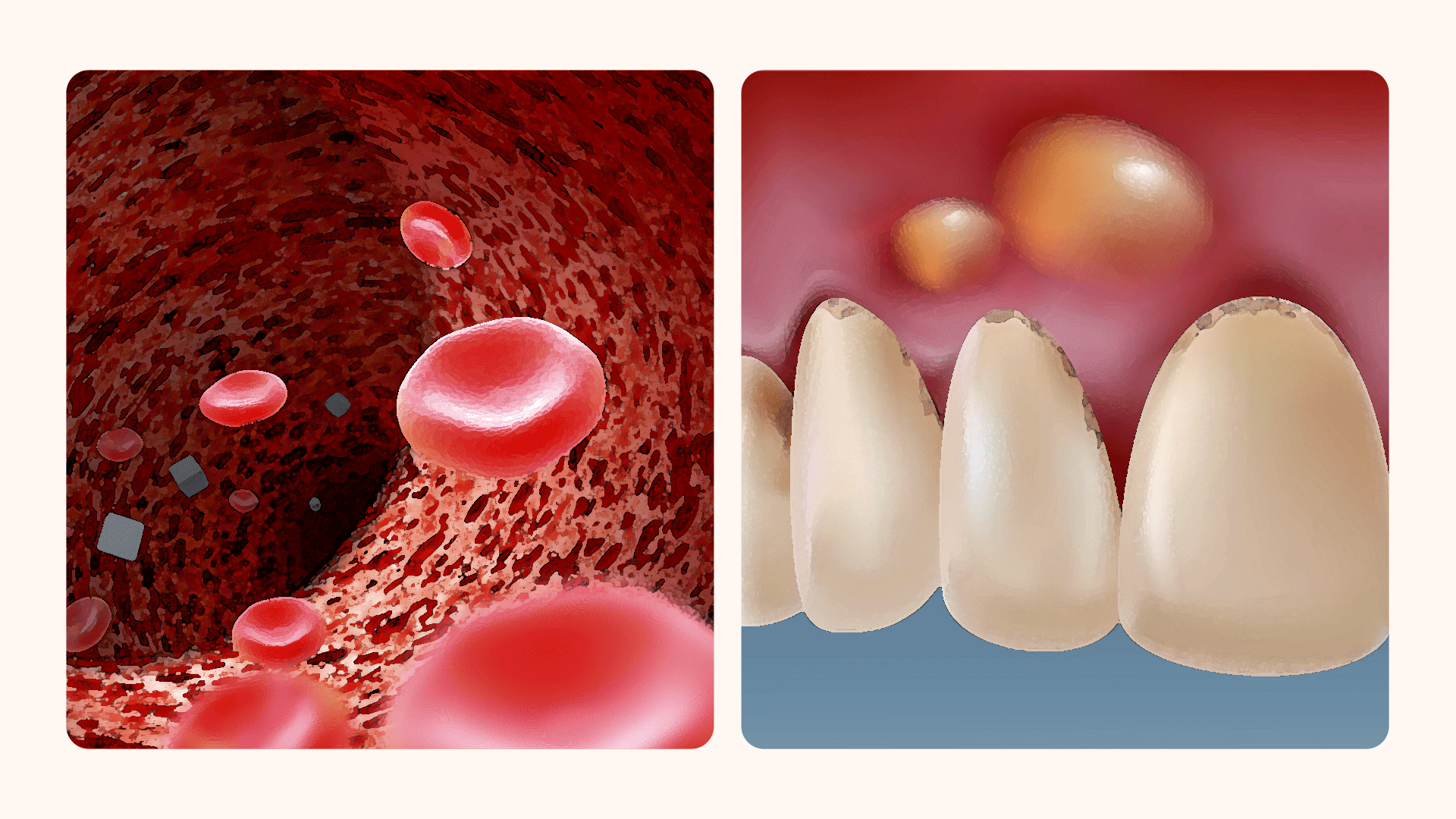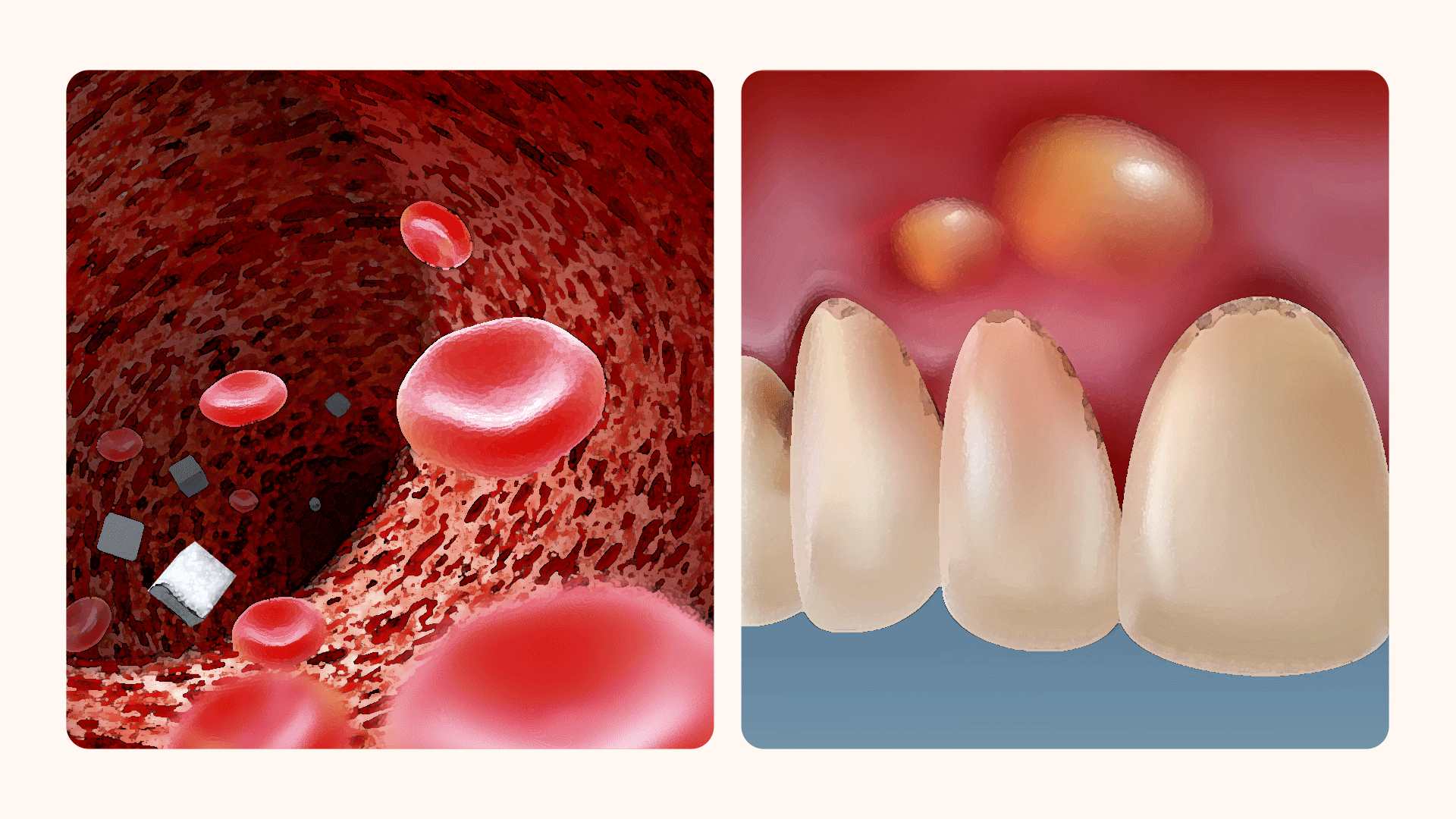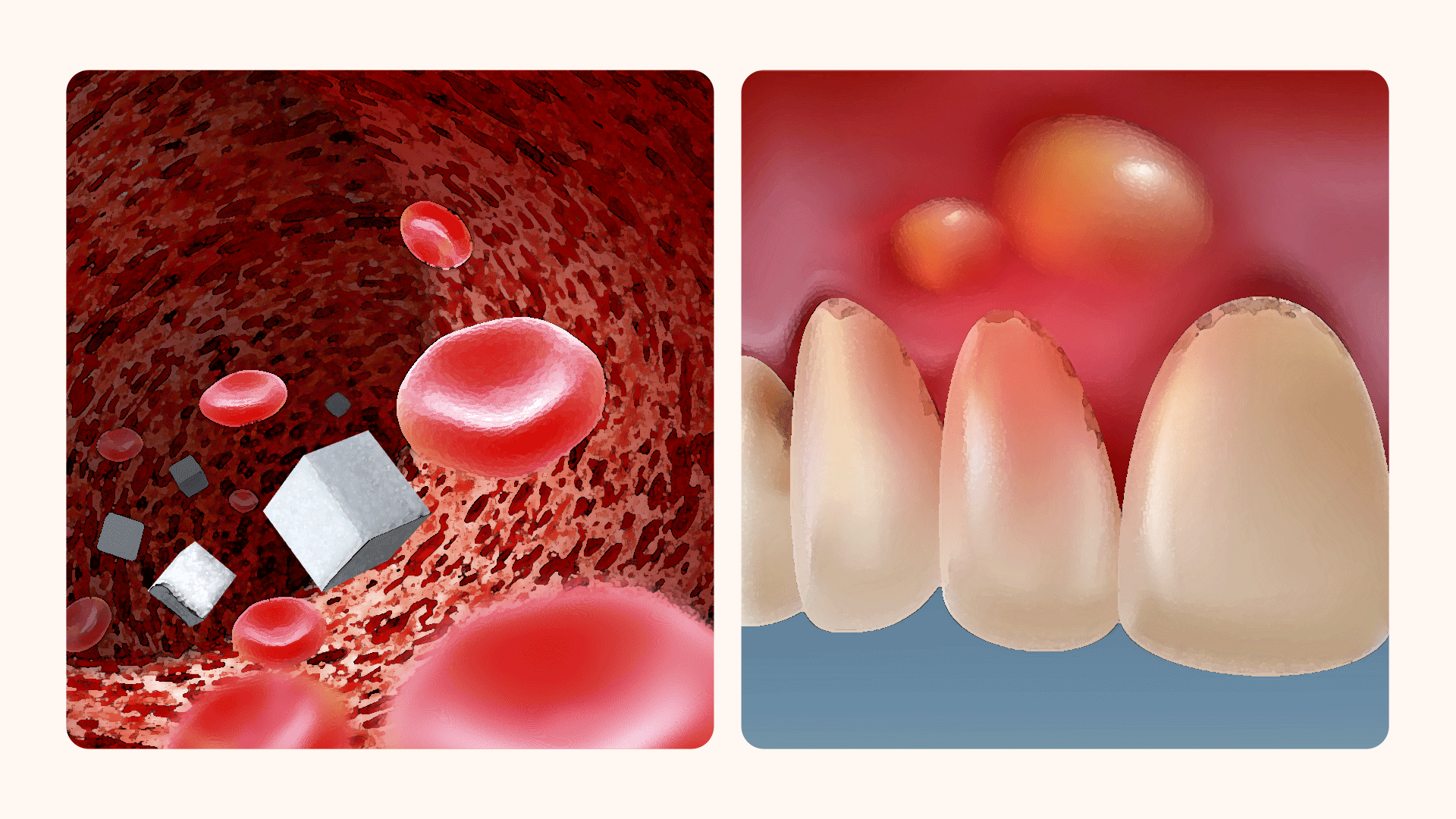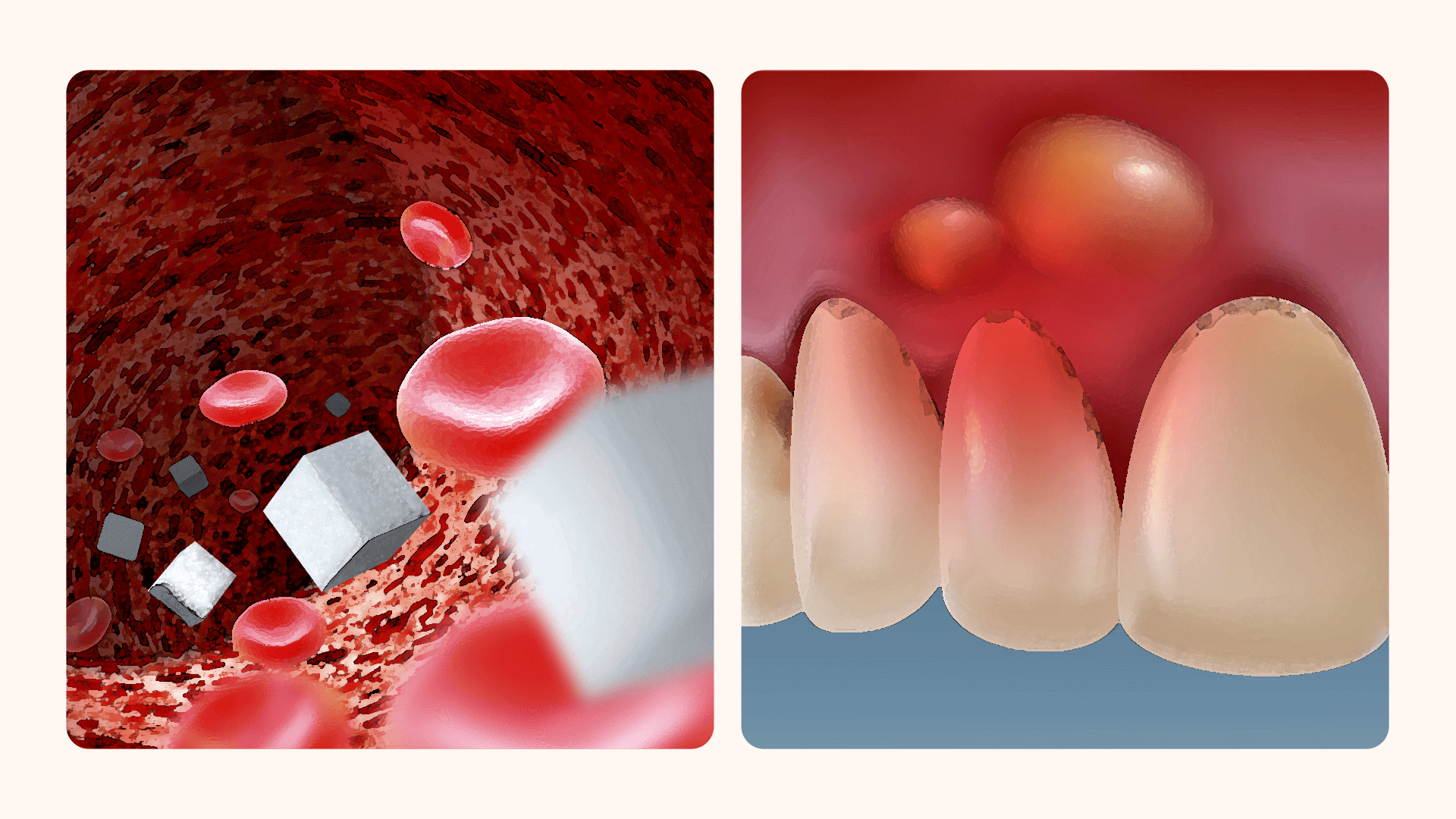
Many patients worry after hearing that "implants are absolutely impossible for diabetics" or "high blood sugar leads to certain failure."
It is true that diabetic patients require more caution than the general population. High blood sugar levels can weaken the immune system, increasing the risk of infection by approximately 2 to 3 times. Additionally, the wound healing process is slower, often taking 1.5 to 2 times longer than average. The period for osseointegration—the process where the implant and bone fuse firmly—can also be extended.
However, these risk factors do not make dental implants impossible. Rather, they are elements that can be successfully managed and overcome through proper clinical preparation.
2. What is the Basis for the 95% Success Rate?
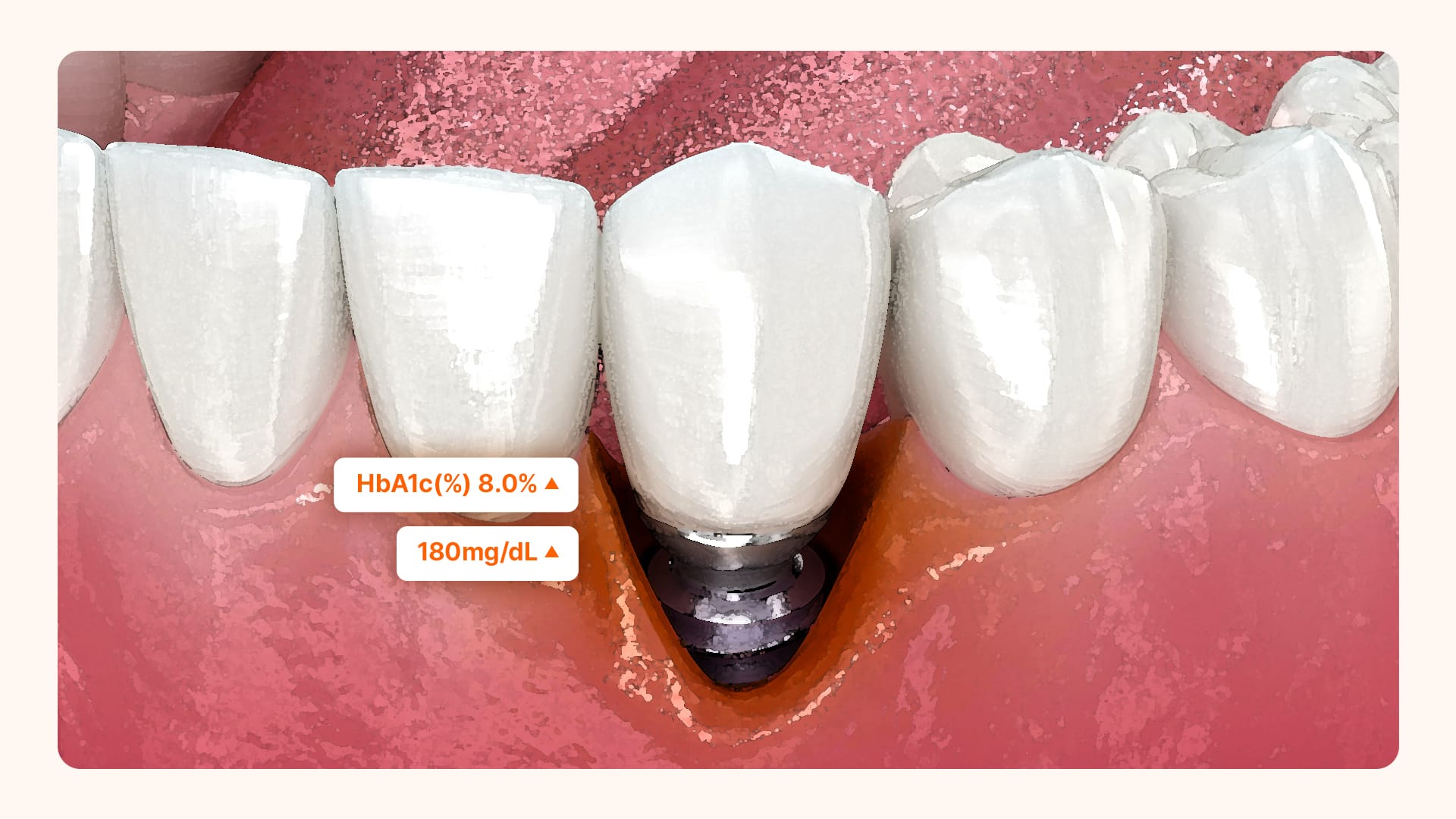
The claim that diabetes makes implants dangerous is only half true. To be precise, the success rate depends entirely on your "blood sugar management status."
According to domestic and international clinical research, patients with HbA1c (Hemoglobin A1c) levels lower than 8% showed implant success rates nearly identical to those without diabetes. Simply put, when post-meal blood sugar is kept below 180 mg/dL or fasting blood sugar below 130 mg/dL, the implant success rate is approximately 96–97%.
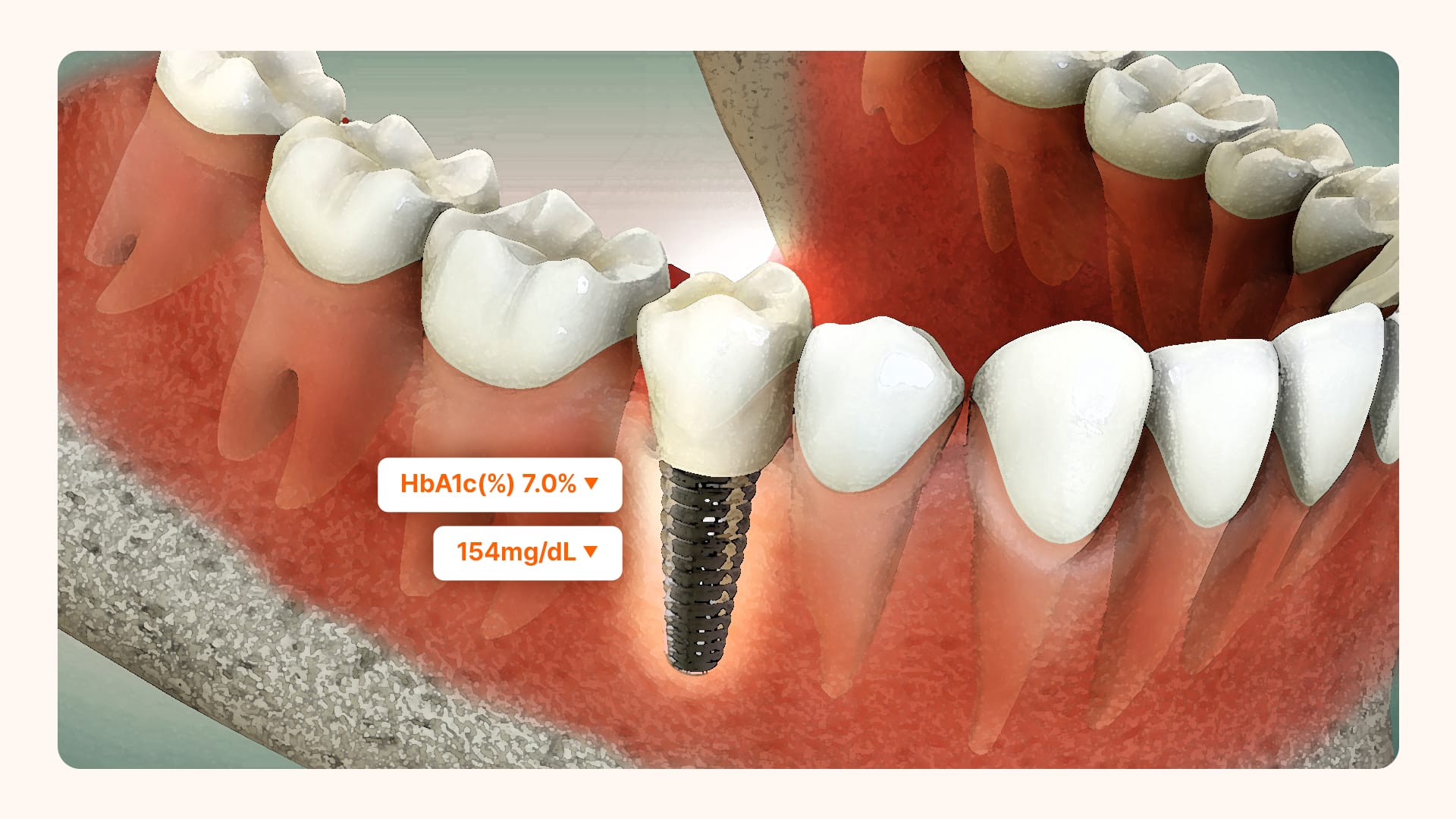
Some studies even show that 87–96% of implants remain stable after five years. This demonstrates that with proper management, success is highly achievable.
3. 4 Essentials to Check Before a Diabetic Implant Procedure

To increase success rates, diabetic patients should choose a clinic with extensive experience and a systematic approach. Be sure to verify the following:
- Do they provide specific success stories?Look for a clinic that explains the treatment process in detail based on the patient's actual glucose levels, rather than just saying "it’s possible."
- Is internal medicine cooperation available?A clinic that prioritizes pre-operative blood sugar checks and maintains a collaborative system with internal medicine specialists is safer.
- Is there a systematic Pre-/During/Post-operative management plan?Choose a clinic that takes responsibility for the entire journey—from initial consultation to long-term aftercare—not just the surgery itself.
- Is an emergency response system in place?Since diabetics can be more vulnerable to infection, verify if the clinic has a clear antibiotic management plan and protocols for emergency situations.
4.Frequently Asked Questions (FAQ)
Q. What are the ideal blood sugar levels before and after the procedure?
Ideally, fasting blood sugar should be below 130 mg/dL and post-meal sugar below 180 mg/dL. On the day of surgery, it is important to maintain fasting levels between 100–150 mg/dL and post-meal levels below 200 mg/dL. Always check your levels immediately before the procedure.
Q. Are there special care methods to prevent complications?
You must strictly follow the prescribed antibiotic regimen and maintain exceptional oral hygiene. Quitting smoking is essential, and staying hydrated is important. We recommend checking your blood sugar at least three times a day for two weeks following the surgery.
Q. How does the process or duration differ from general patients?
For diabetic patients, the osseointegration period (bone-to-implant bonding) typically takes 1.5 to 2 times longer. We usually plan for an additional 3 to 4 months of recovery and double the frequency of follow-up check-ups. This thorough approach is what ensures a high success rate.
Q. . How should I manage the implant once the treatment is finished?
Regular blood sugar monitoring combined with dental check-ups every 3 months is essential. Early detection of gum inflammation is critical, so we recommend more frequent scaling than for non-diabetic patients.

There is no need to give up on implants just because you have diabetes. Through consistent blood sugar management and a systematic clinical system, you can achieve healthy, lasting results. When the patient’s effort meets the expertise of the medical team, the success rate can reach 95% or higher.
Sources
- Al-Ahmari, A. M., & Al-Amri, A. S. (2018). The effect of diabetes mellitus on dental implant survival: a systematic review and meta-analysis. Journal of Periodontal & Implant Science.
- Morad, G. H., et al. (2020). Implant success rates in diabetic patients: A systematic review and meta-analysis. Clinical and Experimental Dental Research.
- Korean Dental Association. (2022). Guidelines for Dental Implant Treatment in Diabetic Patients.
※ The copyright for all content on this blog belongs to Medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads