Learn why preventing periodontitis—the most significant side effect of diabetic implants—and maintaining an HbA1c level below 7% is crucial. Increase your success rate with peri-implantitis treatment and the three core management principles.
“The implant surgery went well, but my gums keep swelling and bleeding. Could it be because of my diabetes?”

For diabetic patients, weakened immunity and excessive inflammatory responses can cause peri-implantitis to progress much faster than in the general population.
This article covers the dangerous cycle between diabetes and periodontitis, why managing gum health is vital, and the three core management methods to keep your implants safe for a lifetime.
1. The Dangerous Mechanism of How Diabetes Attacks the Gums

Periodontitis is not just a simple gum disease; it is a hidden complication of diabetes designated by the American Diabetes Association (ADA). Notably, diabetic patients are three times more likely to develop periodontitis than those without the condition.
| Process | Internal Body Changes | Impact on Implants |
| Rising Blood Sugar → Toxic Substances (AGEs) | High blood sugar produces toxic proteins called 'AGEs,' promoting inflammation and aging. | Gum cells are damaged, making inflammatory responses occur easily. |
| Inflammatory Surge (Increase in TNF-α, IL-6) | Excessive secretion of inflammatory substances hinders bone formation and activates cells that dissolve bone. | The jawbone weakens, and bone resorption around the implant begins. |
| Bone Dissolution (Alveolar Bone Loss) | Osteoblasts (bone-forming cells) lose function while osteoclasts (bone-resorbing cells) become overactive. | The bone holding the implant gradually disappears. |
| Plaque and Bacterial Toxin Production | Food debris and bacteria combine to form toxins. | Weakened immunity leads to an inability to respond properly to bacteria. |
| Occurrence of Peri-implantitis | Combined bacterial toxins and inflammatory responses create severe inflammation. | Gums swell and bleed, and the implant begins to shake. |
2. The Vicious Cycle: Periodontitis Worsening Diabetes
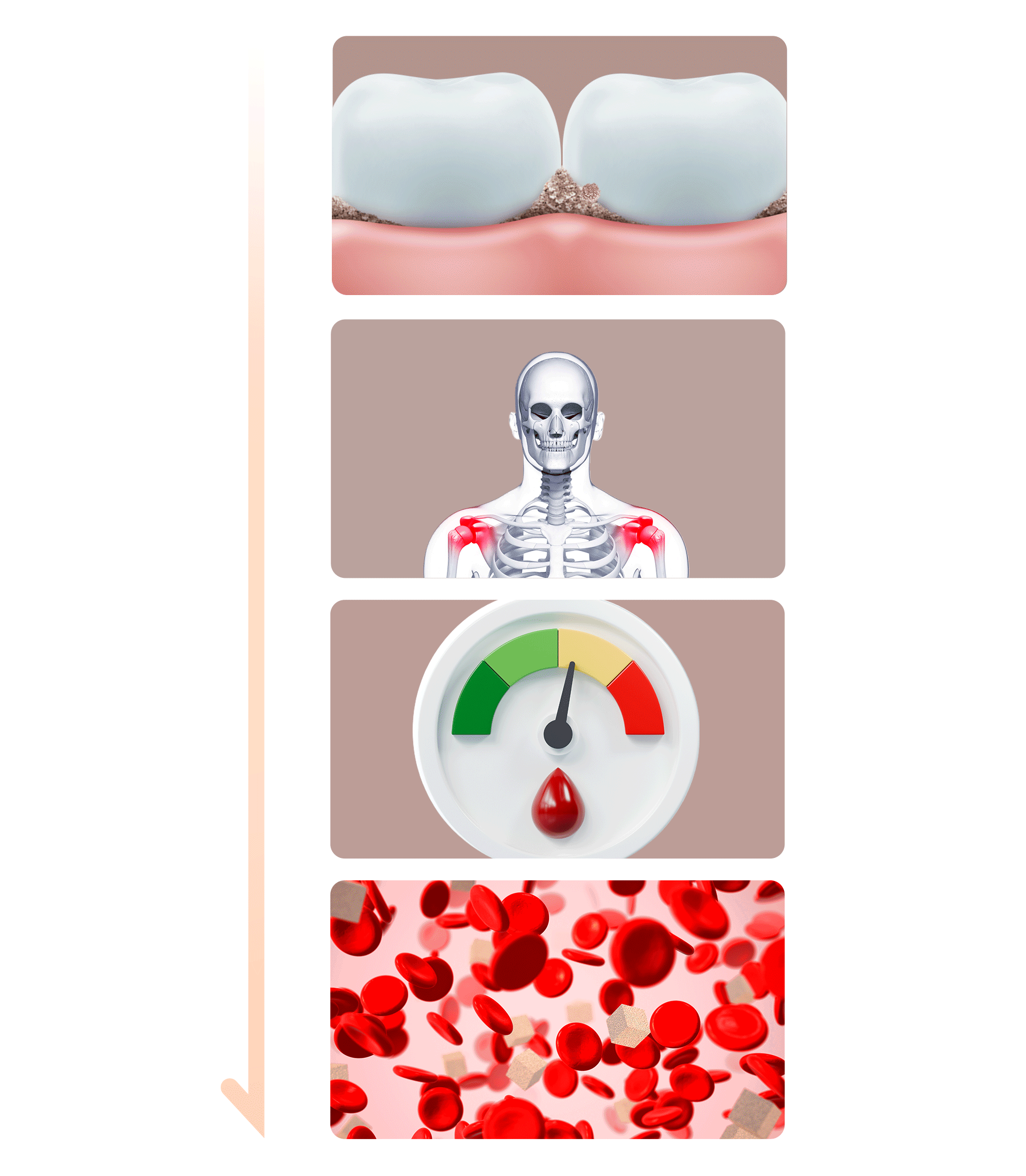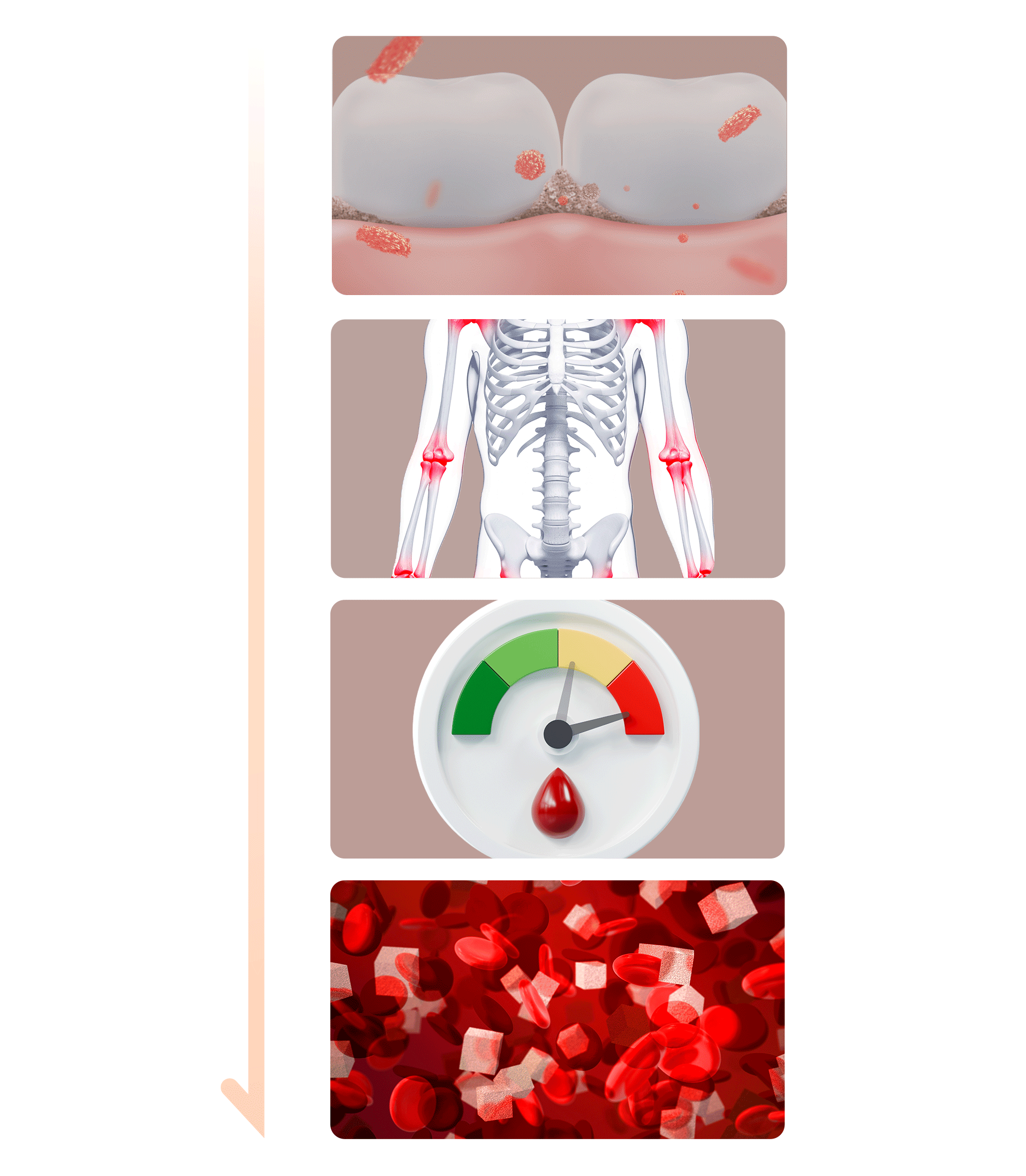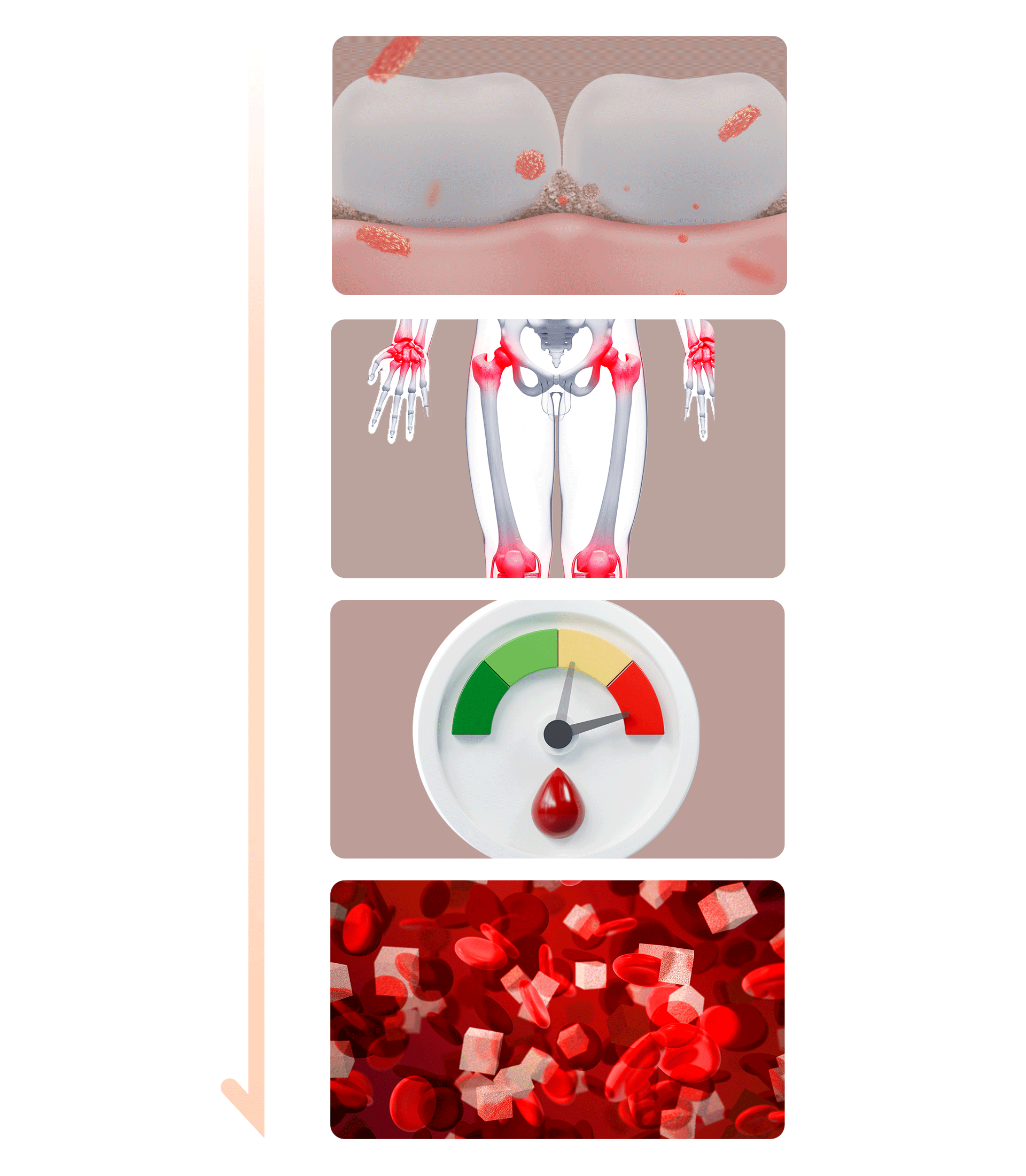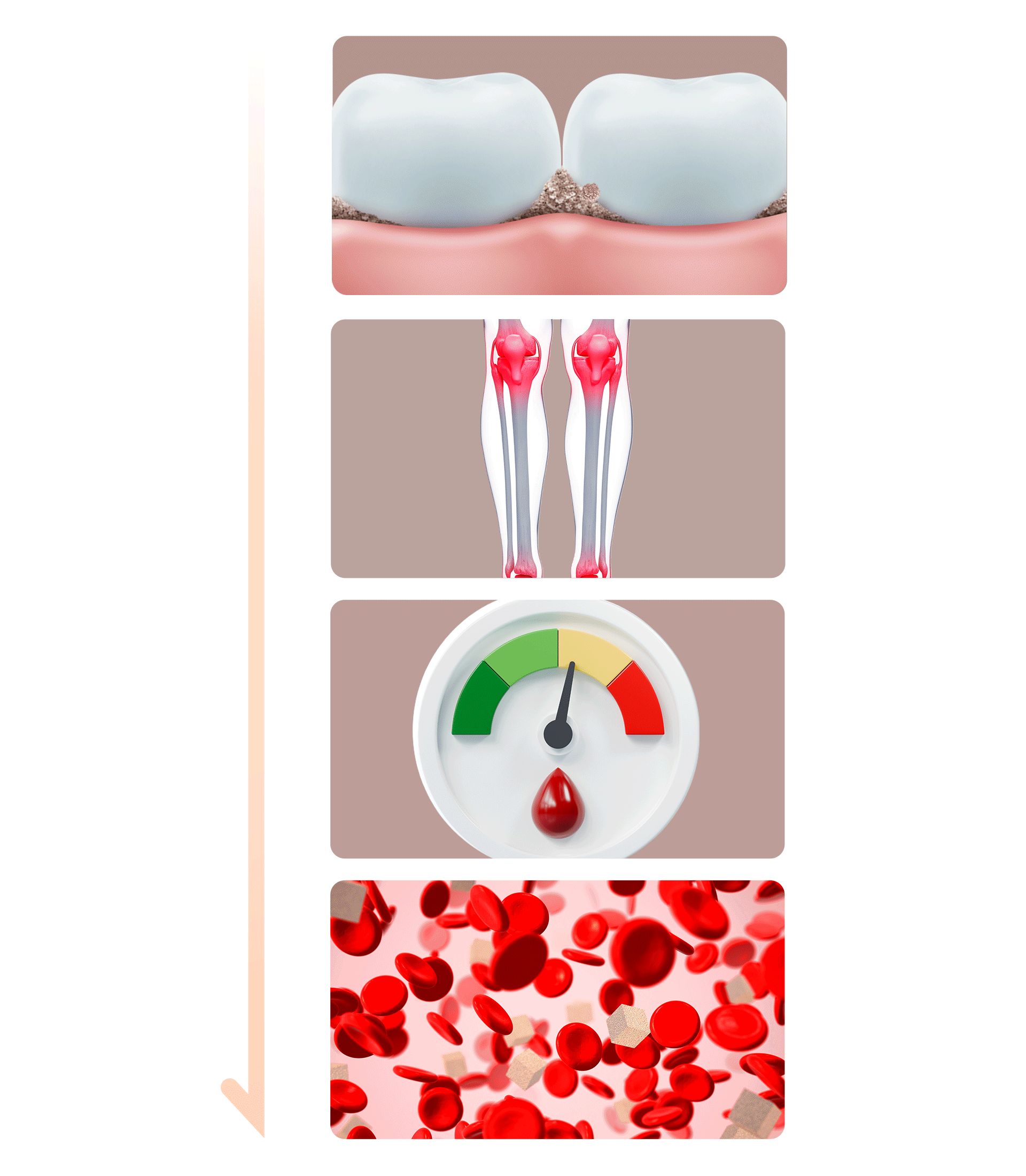
- Inducing Bacteria and InflammationBacteria and byproducts found in plaque and tartar—the causes of periodontal disease—trigger inflammation. These bacteria and inflammatory substances can enter the bloodstream and spread throughout the body, potentially advancing and worsening diabetes.
- Increased Insulin ResistanceInflammation from periodontal disease increases insulin resistance, making blood sugar control even more difficult. It works similarly to how carbon buildup in a car engine reduces fuel efficiency.
- Worsening Due to Dietary ChangesSevere periodontal disease makes chewing difficult, leading to a higher intake of easily digestible fats and simple sugars. Simple carbohydrates like instant noodles or bread cause rapid spikes in blood sugar, negatively impacting diabetes.
3. Three Danger Signals When Diabetic Implants are Neglected
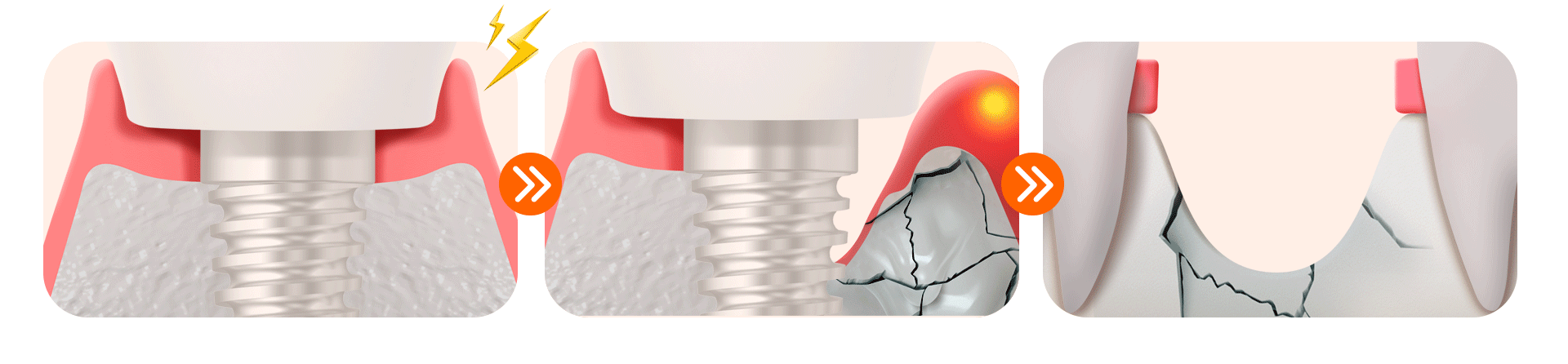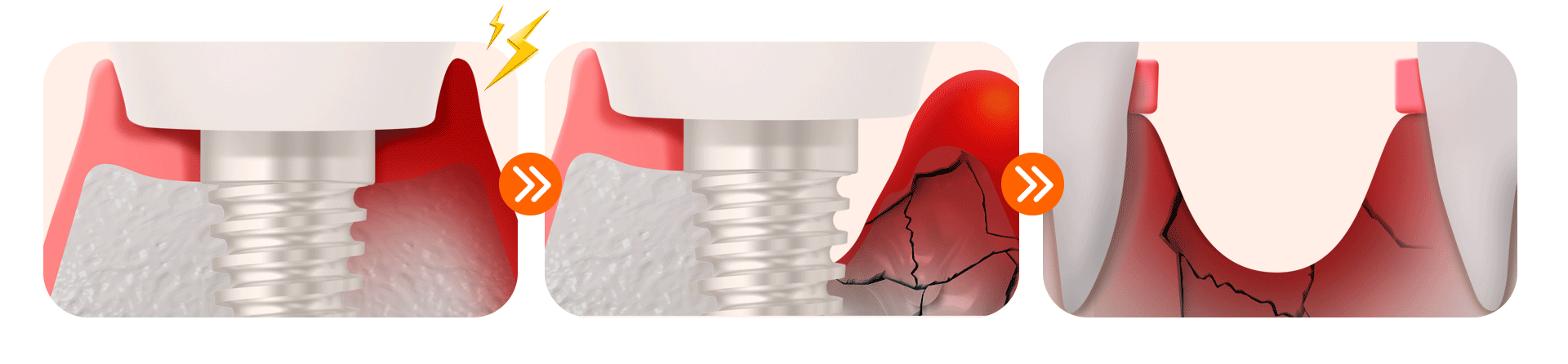
If periodontal management is neglected in diabetic patients, peri-implantitis (inflammation around the implant) progresses very rapidly, leading to the following three stages of side effects.
[3 Stages of Danger Signals for Neglected Diabetic Implants]
| Stage | Main Symptoms / Changes | Clinical Risk | Action Plan |
| Stage 1 | Start of Peri-implantitis Gum swelling, bleeding during brushing. | Early stage of inflammation; can progress rapidly. | Immediate dental visit; professional scaling required. |
| Stage 2 | Jawbone Damage Bone starts to dissolve. | Weakened support due to bone loss; risk of revision surgery. | Laser inflammation treatment and bone preservation therapy needed. |
| Stage 3 | Revision Surgery or Extraction Severe jawbone damage; implant cannot be maintained. | Implant removal and bone grafting required. | Potential consideration for dentures. |
4.The 3 Core Management Principles for Diabetic Implants

- Lifelong 'Regular Professional Care'
- Visit the clinic every 2 months for intensive management of inflammation and tartar.
- Minimize discomfort and bleeding with non-incisional laser treatments.
- Consistent management leads to a 10-year implant survival rate of over 95%.
- Thorough 'Self-Oral Hygiene'
- Completely remove plaque using toothbrushes, floss, interdental brushes, and water flossers.
- The 3-3-3 Rule: Brush 3 times a day, within 3 minutes after meals, for 3 minutes.
- Frequent water intake to suppress bacteria if the mouth feels dry.
- 'Blood Sugar Control' in Partnership with Your Doctor
- Maintain HbA1c below 7% to suppress inflammation.
- Strengthen immunity with a fiber-rich diet, smoking cessation, and hydration.
- Collaboration between internal medicine and dental clinics yields an implant success rate of approximately 97%.
5.Frequently Asked Questions (FAQ)
Q. My gums are swollen around the implant; is it definitely peri-implantitis?
If there is swelling and bleeding, there is a high probability of peri-implantitis. Diabetic patients are at a higher risk of inflammation progressing quickly to the bone, so you should visit a dentist immediately for an accurate diagnosis and professional cleaning. This is the most important action to prevent early diabetic implant side effects.
Q. Is there a way to self-check if my gum management is going well after an implant?
Check if there is bleeding when cleaning the area between the implant and the gum with an interdental brush. If bad breath worsens or swelling and bleeding occur, it is a signal that inflammation is progressing. Detecting these subtle changes before feeling pain is the golden time for peri-implantitis treatment.
Q. Since diabetes slows down wound healing, how is the treatment for inflammation around implants different?
Diabetic patients are more vulnerable to bacterial infections. Therefore, methods that involve less bleeding and discomfort, such as laser treatment (non-incisional) that removes inflammation without cutting the gums, are more effective than general inflammatory treatments. It is important to remove inflammation while minimizing jawbone loss.
Q. My HbA1c level is high; must I get implant surgery?
If your HbA1c level is very high (9% or above), we recommend focusing on stabilizing your blood sugar first for a successful diabetic implant outcome. For safe treatment and to lower the risk of complications, it is in your long-term best interest to lower the level to below 7% in cooperation with an internal medicine specialist before starting implant treatment.

The success of a diabetic implant depends more on the management of periodontitis than the surgery itself. The key is to receive professional, close-knit care at a dental clinic every 2 to 3 months. Since the jawbone of a diabetic patient is vulnerable to inflammation and slow to recover, preventive management that blocks any chance of inflammation around the implant is vital.
Sources
- Korean Diabetes Association. (2023). Clinical Practice Guidelines for Diabetes 9th Edition: Management of Periodontal Disease.
- Korean Academy of Periodontology. (2020). Recommendations for Management of Periodontal Disease and Implants in Diabetic Patients.
- Löe, H., et al. (1993). Diabetes and periodontal disease: two-way relationship. Journal of Periodontology, 64(11 Suppl), 1056-1061.
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



