The success rate of dental implants for diabetic patients depends heavily on blood sugar control. Check the HbA1c standards and essential safety protocols before starting your treatment.
"Is it okay to get implants even though I have diabetes?"

Patients who have lived with diabetes for over a decade often give up on treatment due to a vague fear that "implants are impossible for diabetics."
However, the feasibility of a diabetic dental implant is not determined by a single glucose reading. It is a result of long-term blood sugar management, overall systemic health, and the clinical experience of the medical team. This guide aims to provide transparent and accurate answers to common concerns regarding diabetes and dental implants.
1. The Relationship Between Diabetes and Implants
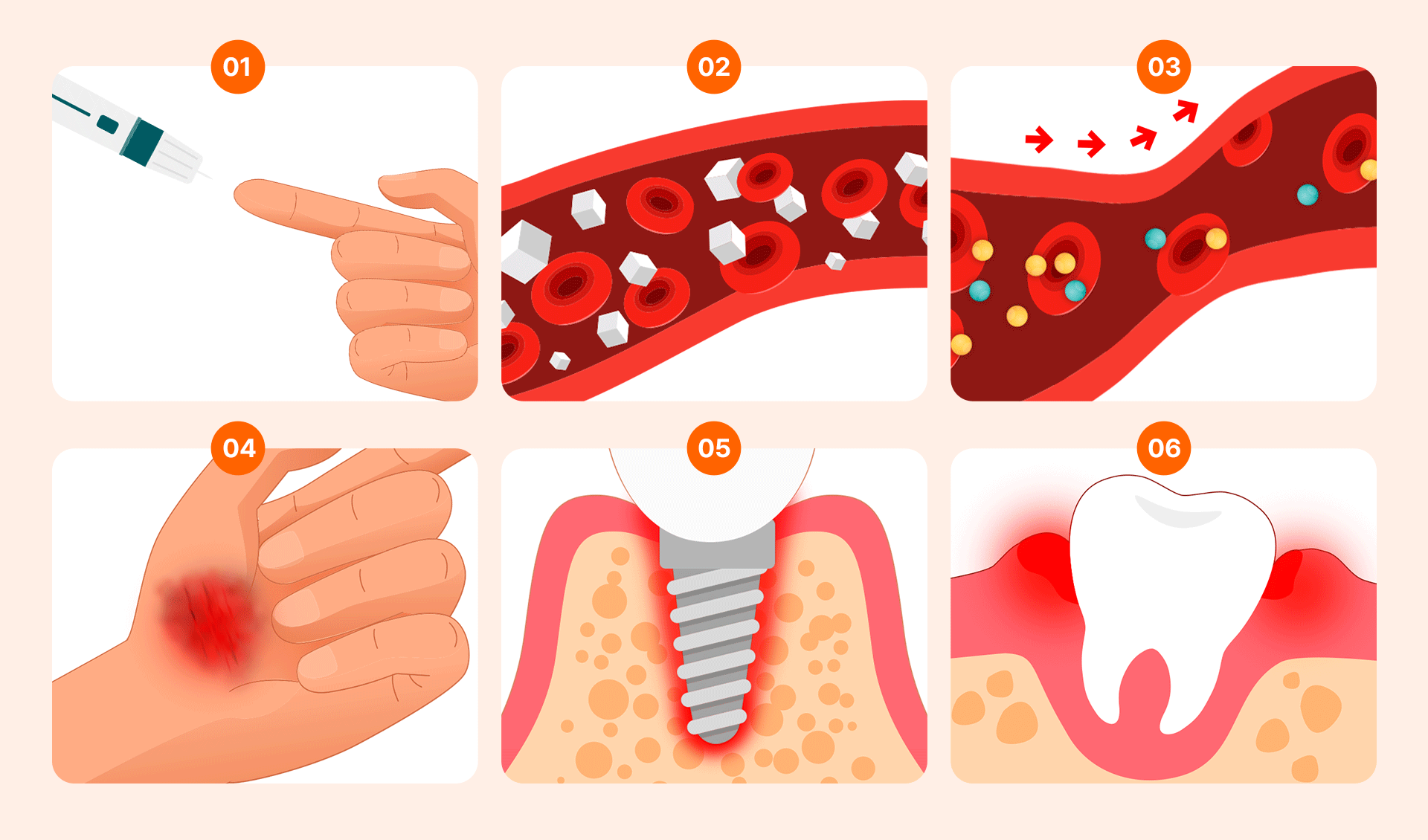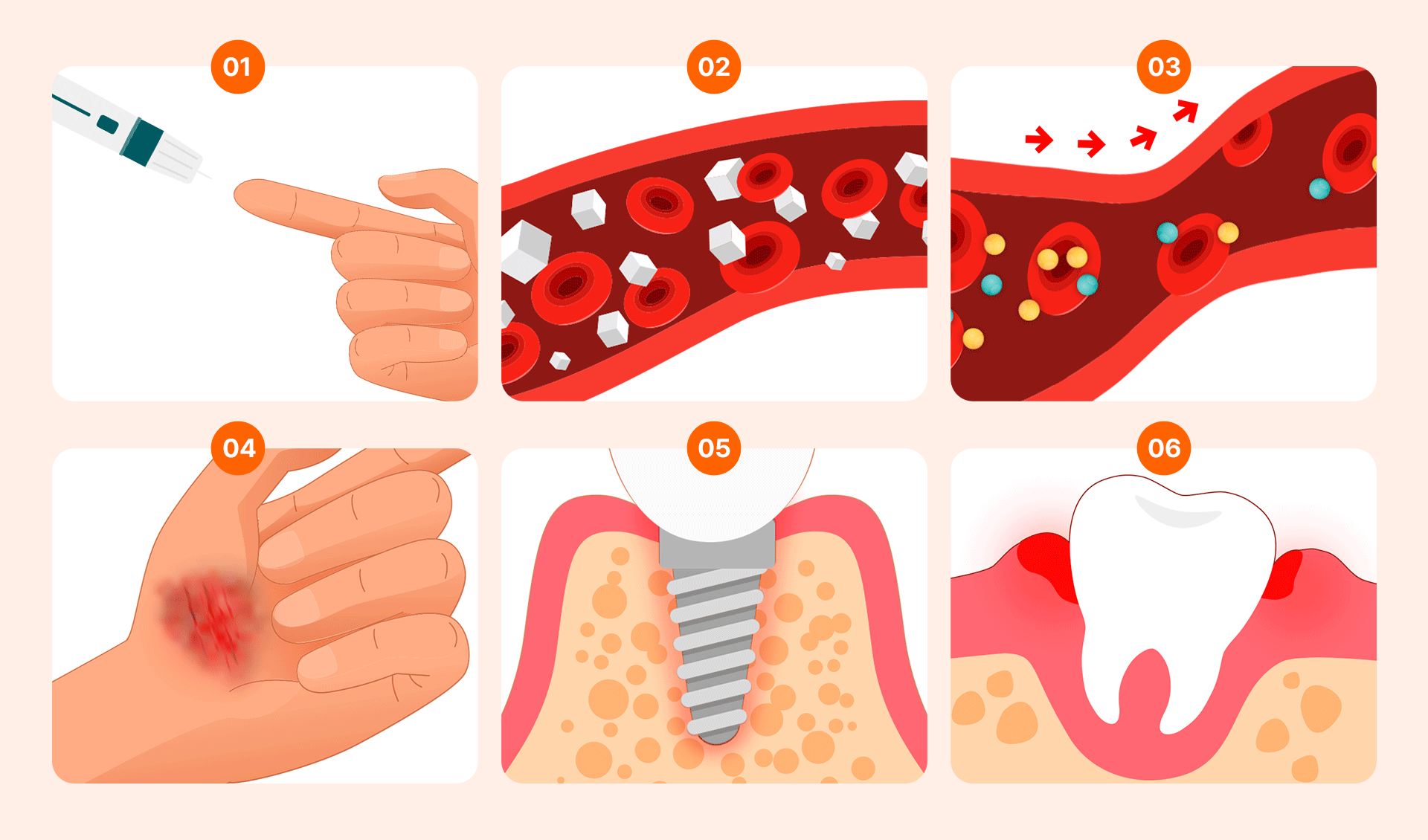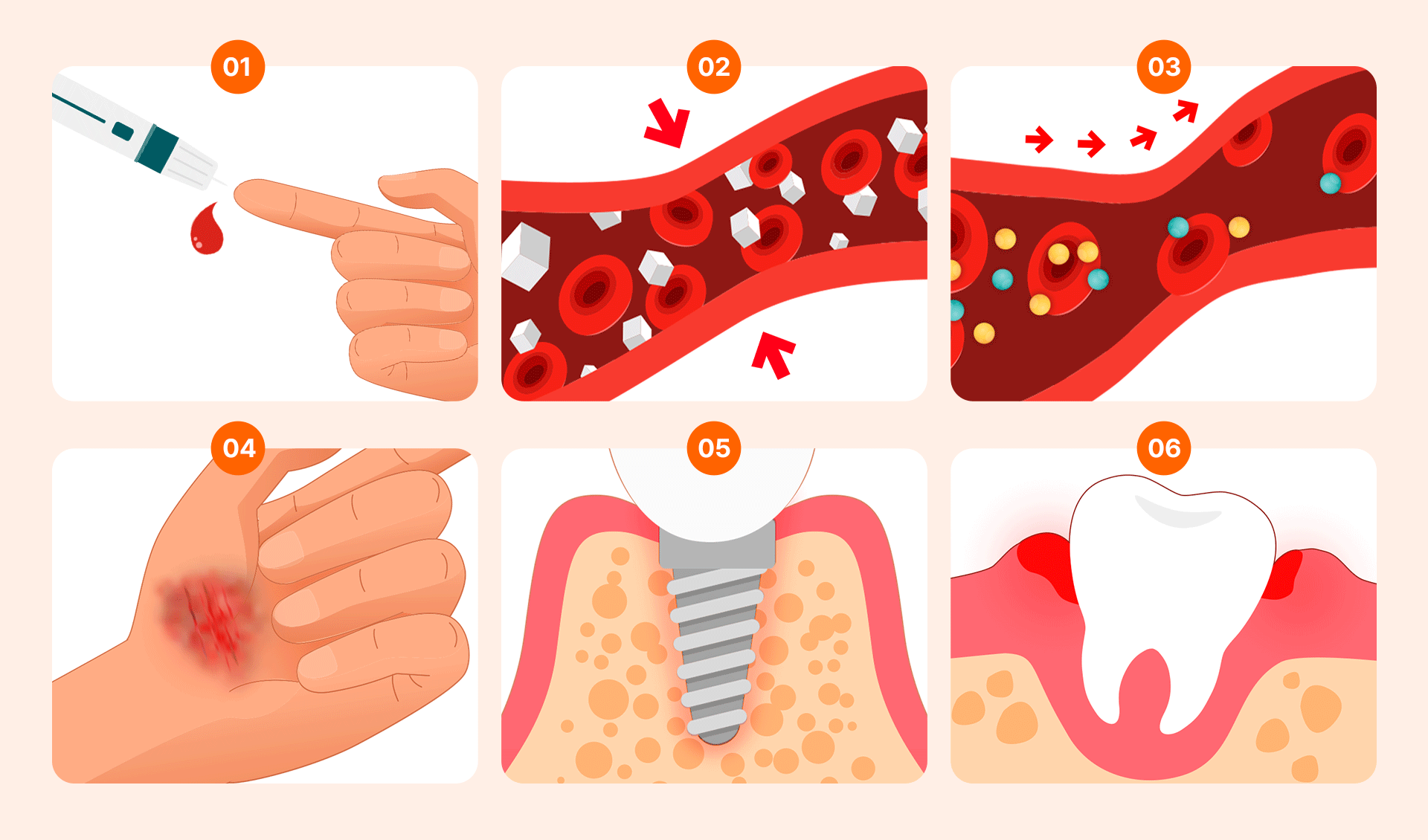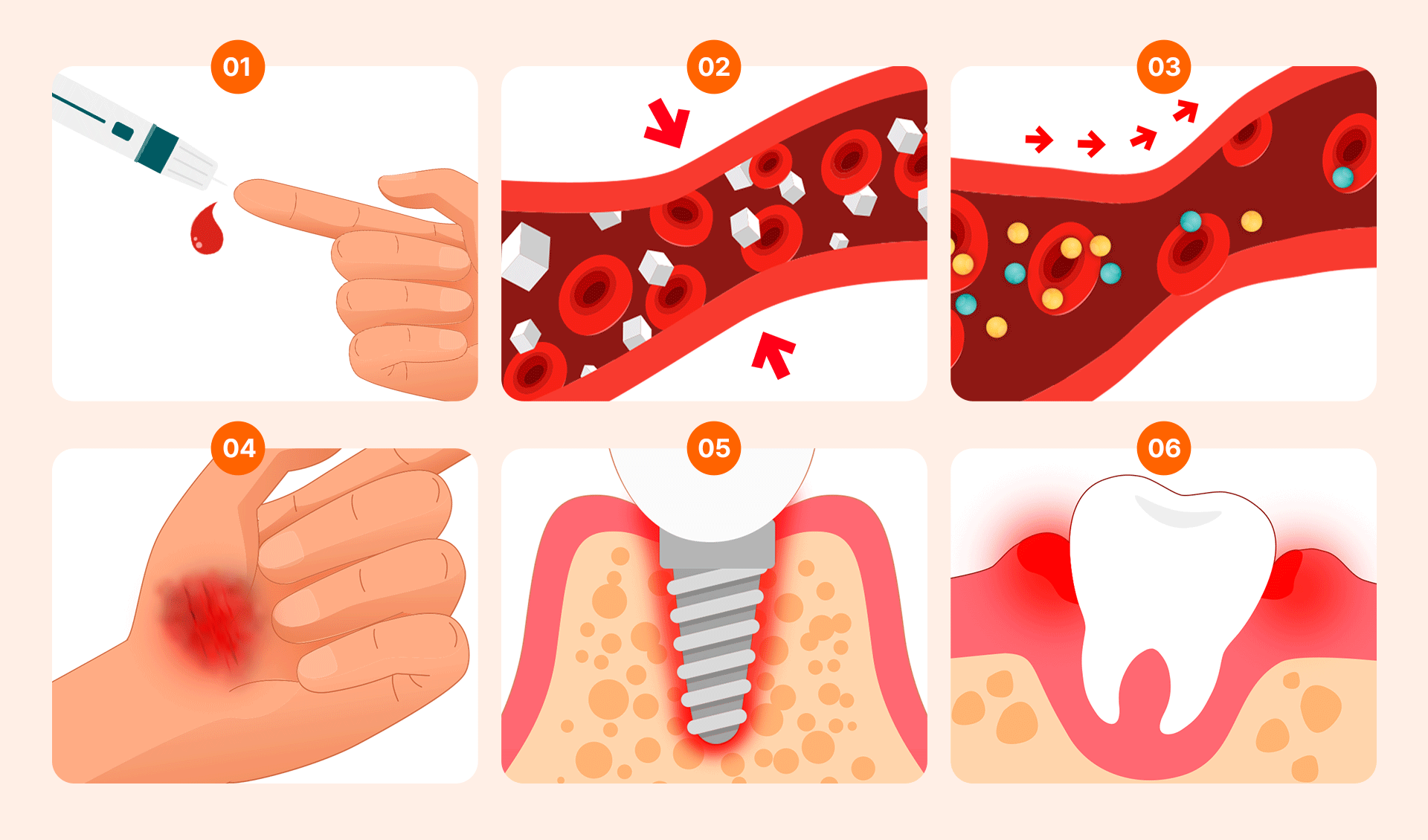
Having diabetes does not mean you must give up on implants. The primary issue arises from uncontrolled hyperglycemia (high blood sugar).
- Delayed Healing and Infection Risk: High blood sugar impairs white blood cell migration, which slows down the recovery of the surgical site and increases the risk of infection.
- Impaired Osseointegration: Implants must fuse firmly with the bone. Advanced Glycation End-products (AGEs) can hinder bone regeneration, and poor blood circulation in diabetic patients can increase the probability of failure.
- Vulnerability to Gum Disease: High glucose levels in the mouth facilitate bacterial growth. Combined with a weakened immune system and suboptimal bone metabolism, this significantly increases the risk of peri-implantitis.
2. Blood Sugar Standards: What is the Safe Range?
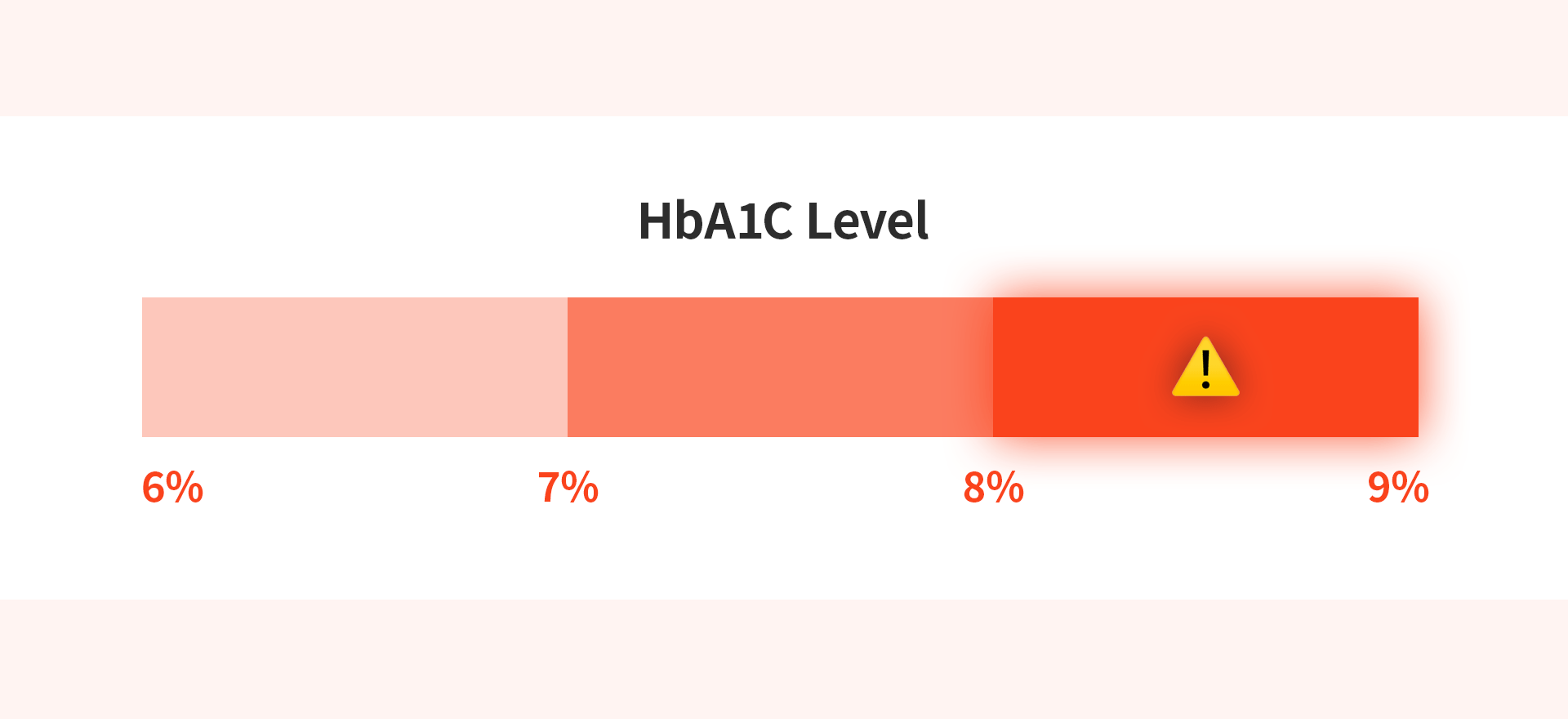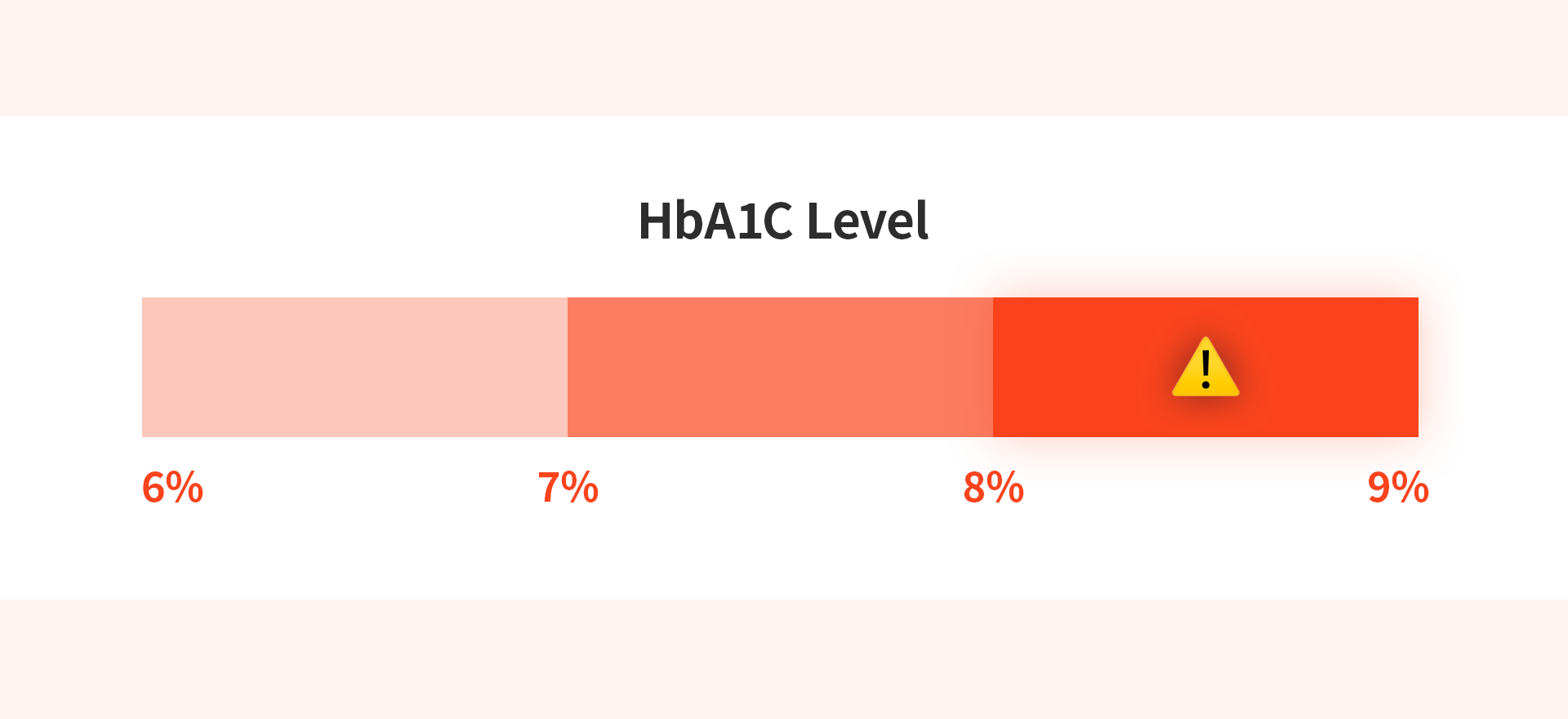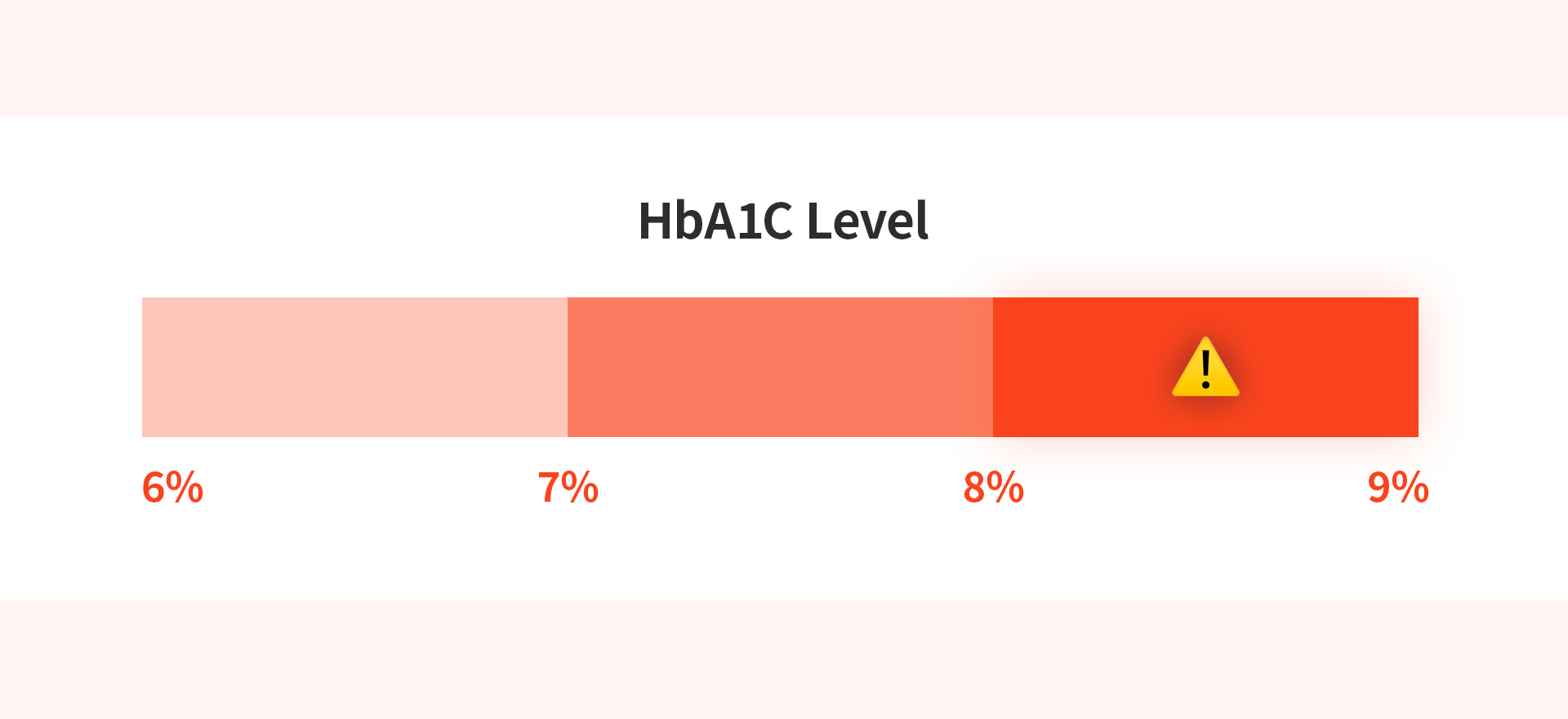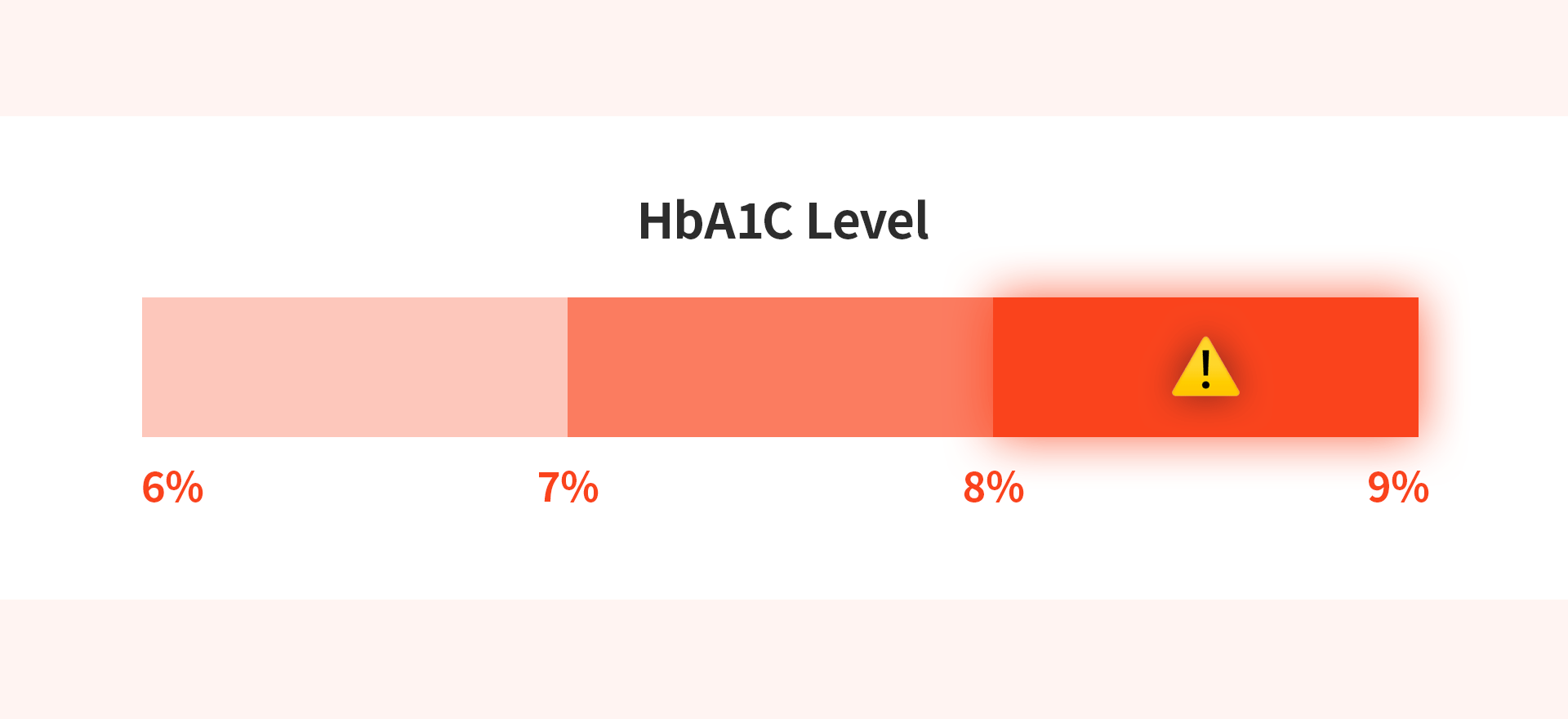
The most critical criterion for deciding on a diabetic dental implant is the patient's level of glycemic control.
HbA1c (Hemoglobin A1c) Levels
HbA1c is a vital indicator that shows average blood sugar levels over the past 2–3 months, offering a more reliable assessment than a single fasting glucose test.
| HbA1c Level | Evaluation | Feasibility for Implants |
|---|---|---|
| ≤ 7.0% | Safe Zone | Similar success rate to non-diabetic patients |
| 7.0% – 7.9% | Caution Zone | Management and clinical caution required |
| ≥ 8.0% | Risk Zone | Blood sugar stabilization prioritized first |
3. Treatment Planning and Management for Diabetics
1) Prioritizing Blood Sugar Control
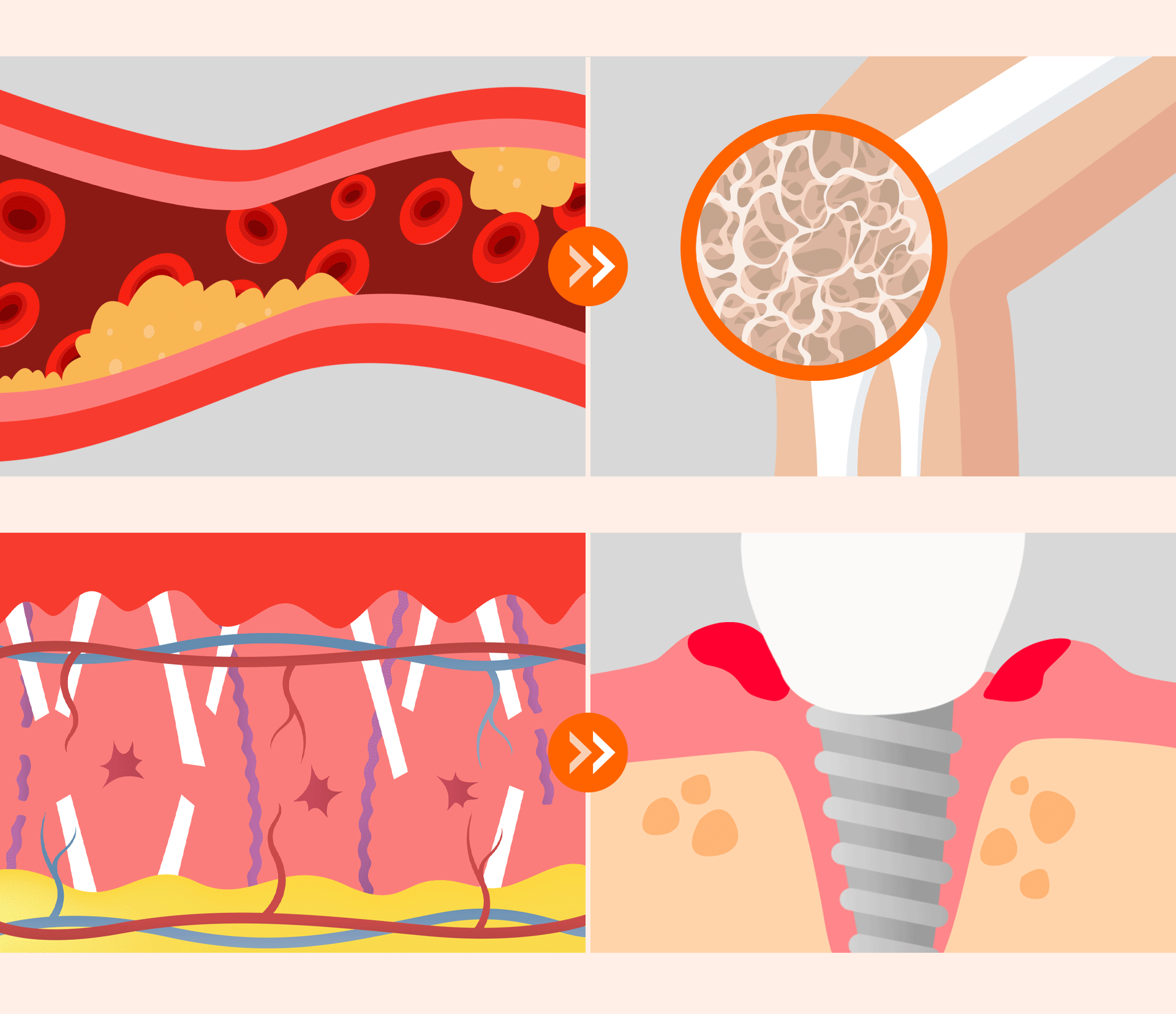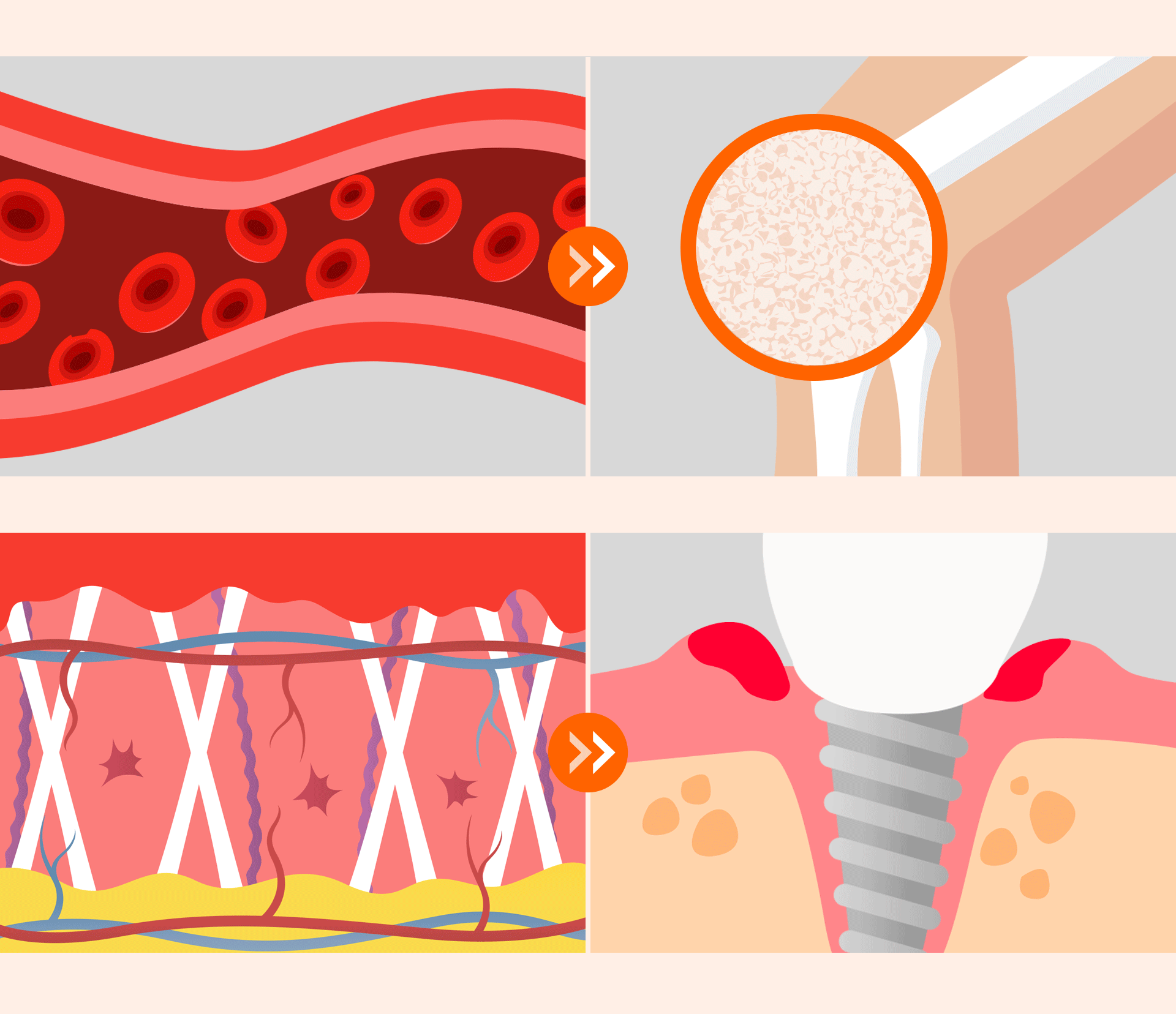
High glucose levels weaken bone-forming cells and lead to the accumulation of AGEs, which trigger inflammatory responses. Stabilizing blood sugar is the most important factor in increasing the implant's success rate and preventing osseointegration failure.
2) Impact of Fluctuating Blood Sugar on Recovery
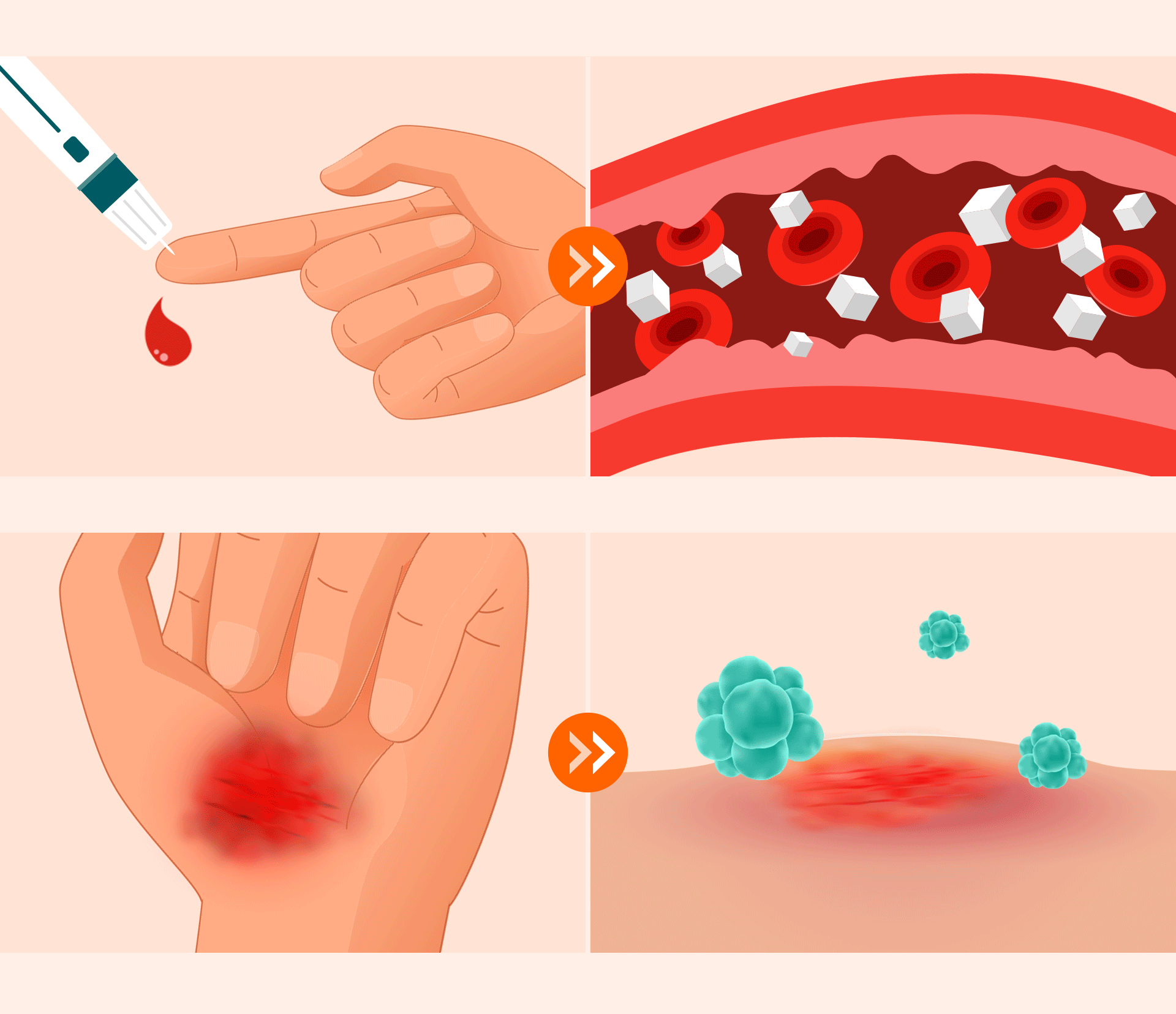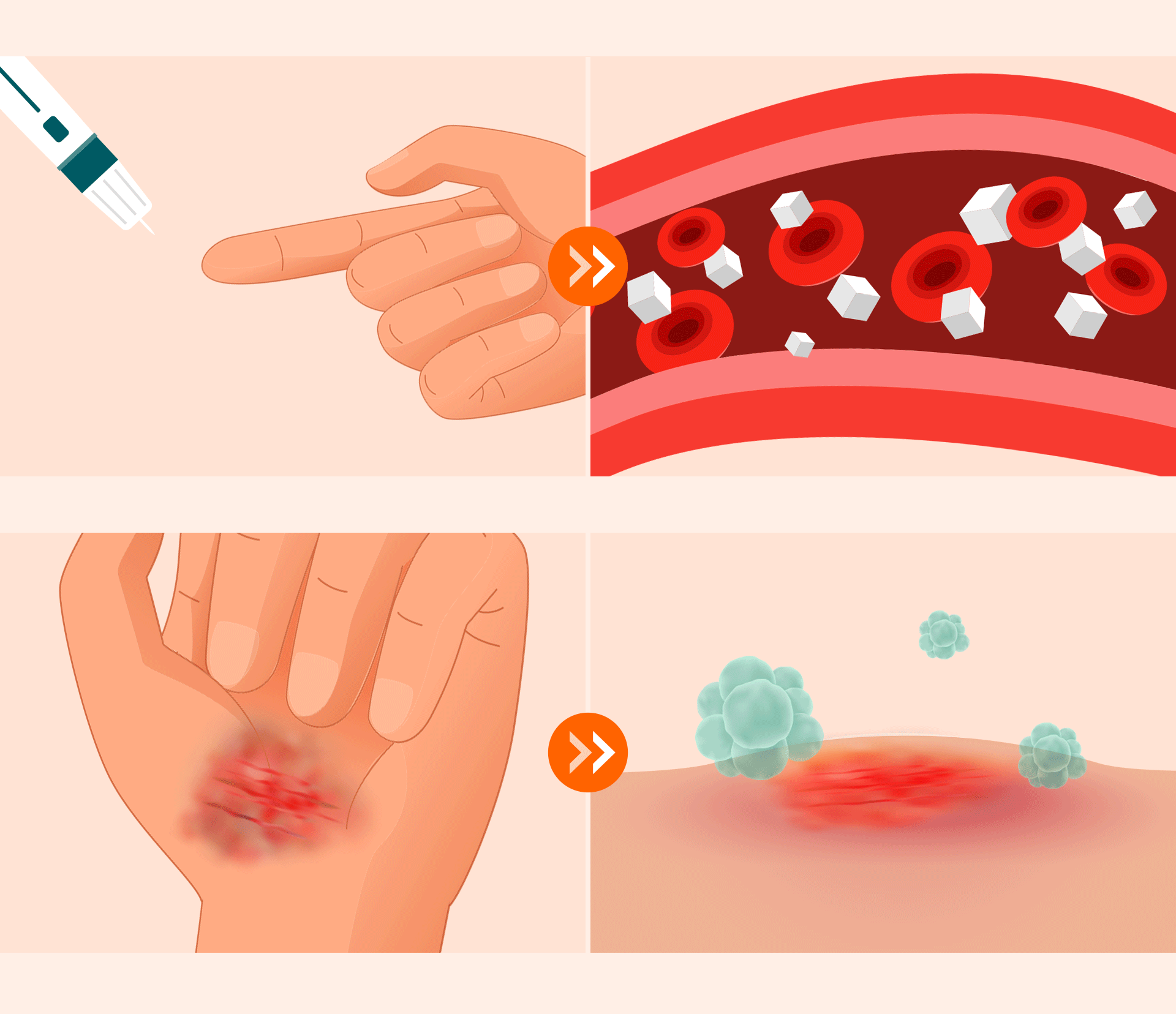
Unstable glucose levels weaken blood vessels, hindering the supply of oxygen and nutrients. This leads to slow wound healing and vulnerability to infection, which are the leading causes of implant failure.
3) Internal Medicine Consultation and Integrated Care
Before treatment, a consultation with an internal medicine specialist is necessary to review medical history and medications. Specifically, blood thinners or antiplatelet agents may increase the risk of bleeding during surgery; dosages should be adjusted only after consulting your physician.
4. Frequently Asked Questions (FAQ)
Q. Is bone grafting possible for diabetic patients?
Yes, it is. However, since the bone regeneration rate may be slower than average, more meticulous care is required. Success is achieved by strictly managing blood sugar levels and adjusting the treatment plan based on regular check-ups.
Q. Can I have surgery while taking diabetes medication?
In most cases, yes. However, if you are taking medications related to blood clots (Aspirin, Warfarin, etc.), you must consult your physician to adjust the dosage or temporary suspension of the drug to minimize bleeding risks.
Q. Is the recovery period longer for diabetic patients?
If blood sugar is well-controlled, there is no significant difference. However, if levels are unstable, healing may be delayed. Following post-op instructions and maintaining stable glucose levels are essential for a successful recovery.
Q. Are full-mouth implants possible?
Yes, they are. For diabetic patients, full-mouth (full-arch) implants are performed through a systematic, multi-stage process. Given the higher risk of infection, we implement strict sterilization and hygiene protocols. Patients must also be exceptionally diligent with their oral hygiene at home.
Q. When is the best time to start treatment?
The best time is when your blood sugar levels are stable. If you have decided on treatment, it is wise to first consult your internal medicine specialist to stabilize your levels and then coordinate the surgical schedule with your dentist.

Dental implants are fully possible for diabetic patients as long as blood sugar is well-managed. Success is not just about the numbers; it’s about lifestyle management, internal medicine collaboration, and communication with an experienced medical team.
Sources
- American Diabetes Association. (2023). Standards of Medical Care in Diabetes. Diabetes Care.
- Pjetursson, B. E., et al. (2014). Dental implants in patients with diabetes mellitus. Clin Oral Implants Res.
- Korean Diabetes Association. (2023). Clinical Practice Guidelines for Diabetes.
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



