A Guide to Determining the Number of Dental Implants for Edentulous Patients. From minimum placement based on jawbone condition (All-on-4, All-on-6) to full-arch implants, we present a customized digital implant-based treatment plan.
“I have no teeth at all; how many implants should I have placed?”
“People around me say dentures are more comfortable, while others say they had more than 10 implanted… What is the right method for me?”
This is the most common question asked by those considering implant surgery when they are missing all their teeth (edentulous). Much like an architect deciding how many pillars are needed to build a sturdy house, patients want to know the safest and most effective number of implants for their specific oral structure.
In this article, we will cover everything from the core principles of determining the number of implants for edentulous patients to minimal placement methods like All-on-4 and All-on-6, as well as the specific factors that influence these numbers to help ease your concerns.
1. Core Principles of Determining the Number of Implants for Edentulous Patients
The number of implants needed for an edentulous patient varies greatly depending on the treatment goals and oral condition. Some patients desire the restoration of full function similar to natural teeth, while others aim for minimal functional recovery considering practical circumstances.
1) Restoring Natural-Tooth Level Function with Maximum Placement
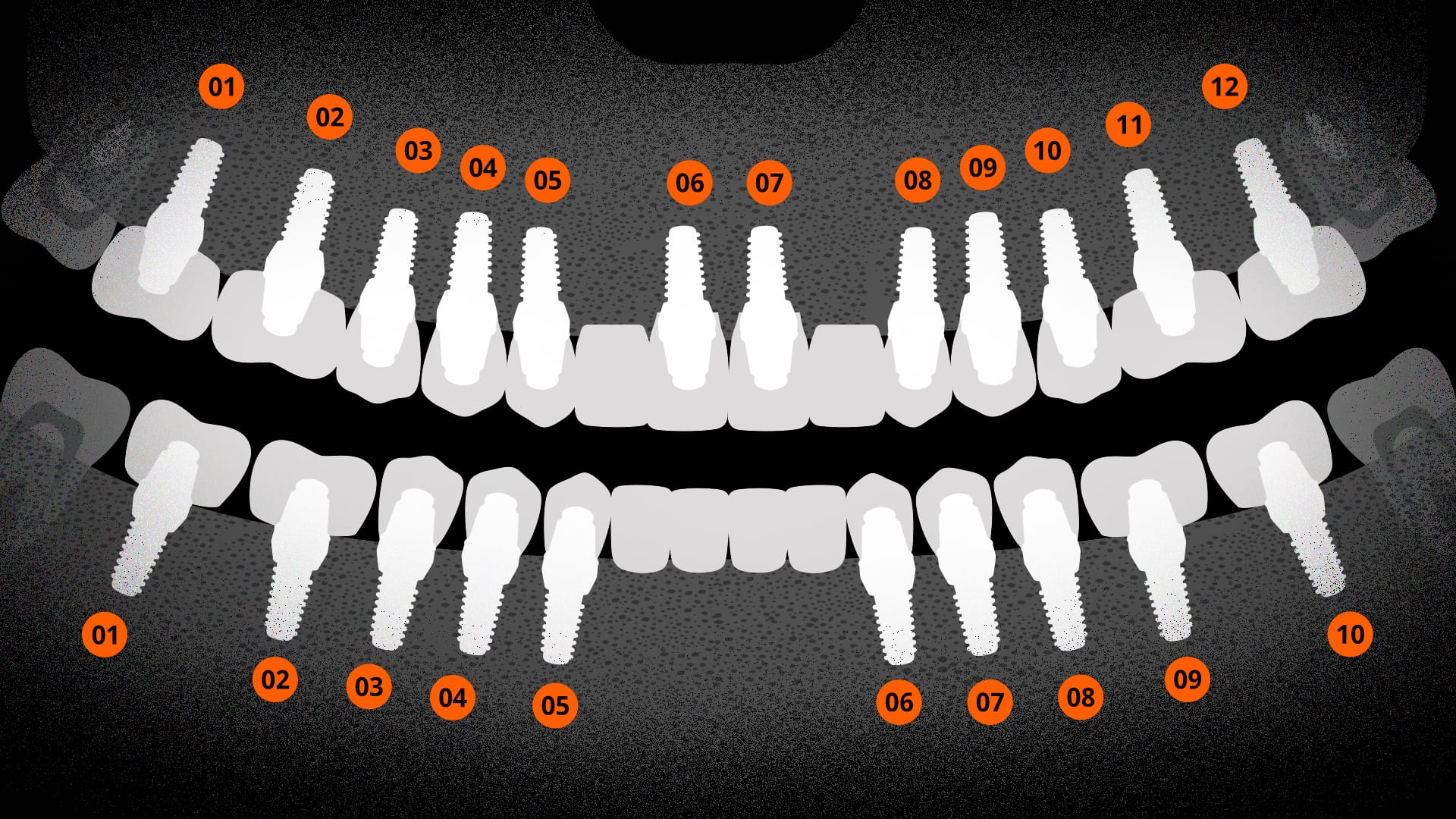
- Goal: Restore chewing power, speech, and aesthetics as close to natural teeth as possible.
- Recommended Number (General Range): 10–12 for the upper jaw, 8–10 for the lower jaw.
- When Bone Condition is Good: Plan for 6–10 per arch → Balancing function and durability.
- Advantages: Distributes load and improves prosthetic stability by placing a generous number of support pillars (implants).
- Note: It is unnecessary to recreate all 28 teeth; the design should focus on a reasonable number of teeth considering load distribution, hygiene, and space.
2) Functional Recovery with Minimum Placement – Implant-Supported Overdentures

- Goal: Reduce cost and surgical burden while improving stability for daily meals.
- Representative Combination: 4 implants in the upper jaw and 2 in the lower jaw to support a denture.
- Upper Jaw (4 implants): Evenly distributed across the molars and front area → Stable denture support.
- Lower Jaw (2 implants): Placed near the front or molars → Acts as a snap (attachment) to reduce movement.
- Advantages: Removable for easy cleaning; relatively easier to reduce surgical scope and duration.
- Limitations: May have limitations in chewing power and aesthetics compared to fixed options → Choose based on lifestyle goals.
3) Minimum Placement, Fixed Implants – All-on-4, All-on-6
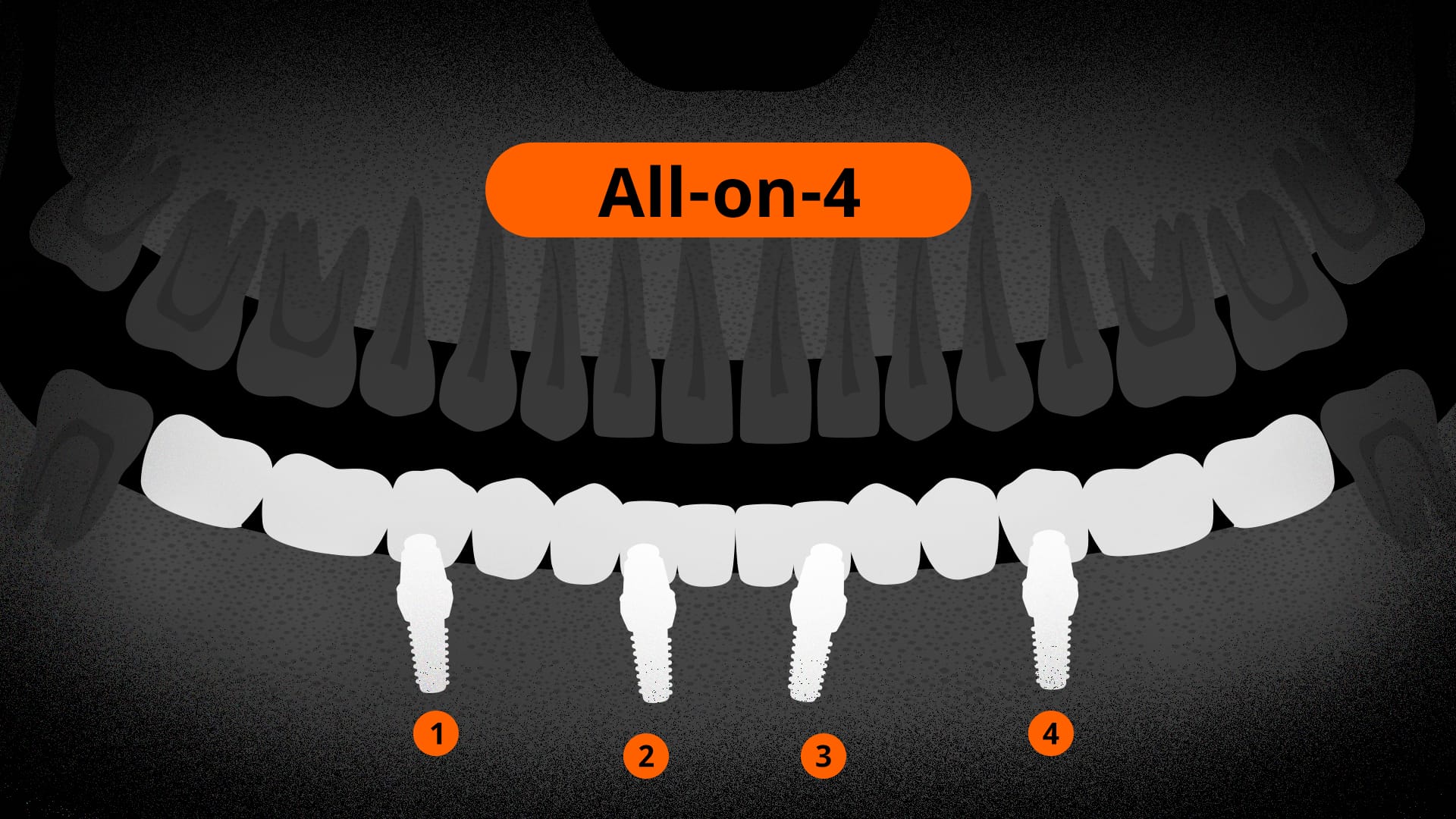
All-on-4
- Number of Implants: 4
- Method: Distributes load through posterior tilted placement; frequently applied to the lower jaw.
- Advantages: Can minimize bone grafting surgery; useful when implants cannot be placed in the lower molar area. Fixed prosthetics are possible. Efficient and allows for fast adaptation with temporary teeth if conditions are met.
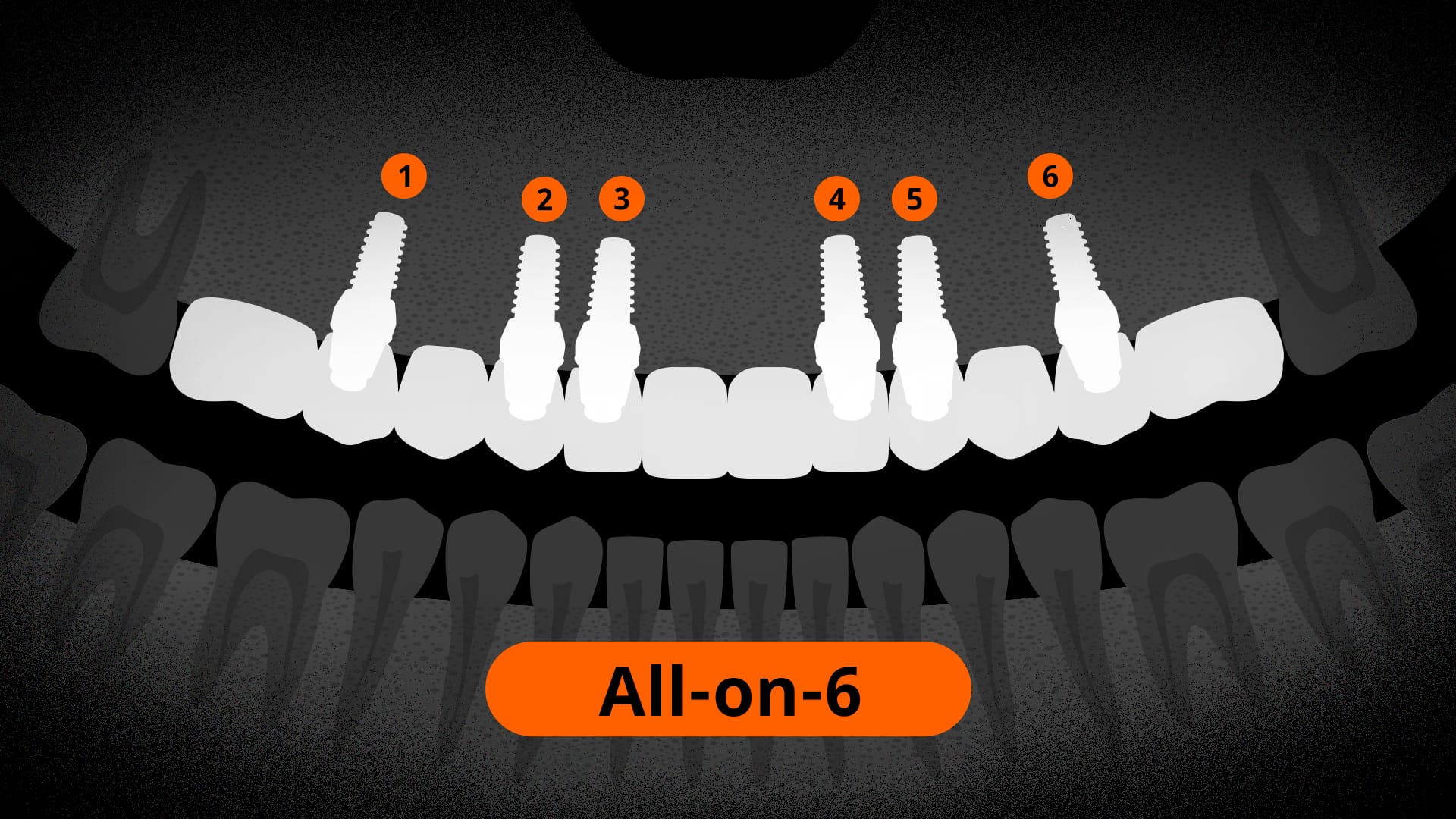
All-on-6
- Number of Implants: 6
- Method: Distributes load through posterior tilted placement; frequently applied to the upper jaw.
- Advantages: Can minimize bone grafting or sinus lift surgery. Fixed implant prosthetics are possible with a minimum number of implants. Expanded support base → enhanced stability and durability, often advantageous for the upper jaw.
The important point here is that because only a minimum number of implants are placed, the patient's chewing habits, jaw structure, and gum bone condition must be checked meticulously. It is most important to establish the most effective treatment plan tailored to each individual patient’s condition.
Summary: The number of implants for an edentulous patient varies from a minimum of 4 (Implant-supported dentures) to a maximum of 12 (Full-arch implants) depending on the target level of functional recovery.
2. Three Key Factors That Determine the Number of Implants
When considering implants for an edentulous state, a customized plan considering your oral structure, health, tooth position, distribution of biting force, budget, and consultation with an expert is more important than simply "how many."
1) Patient’s Oral and Alveolar Bone Condition The patient’s overall oral health, and particularly the condition of the alveolar bone, is the most important factor in determining the number of implants.
- Alveolar Bone Density: Stronger bone allows for stable results with fewer implants.
- Alveolar Bone Thickness: Sufficient thickness is required for placement.
- Alveolar Bone Height: A critical consideration, especially in the molar areas.
2) Tooth Position and Distribution of Biting Force
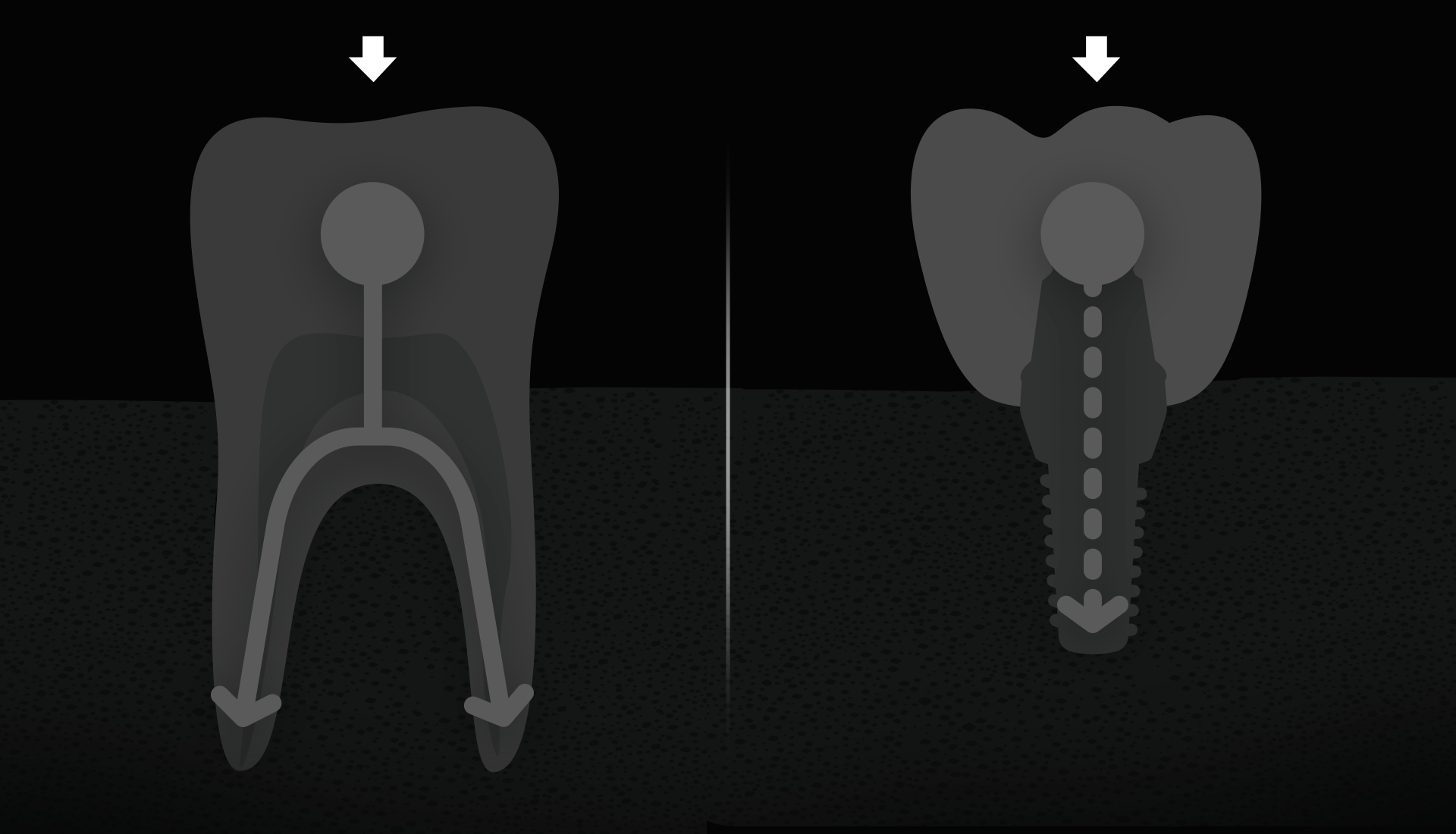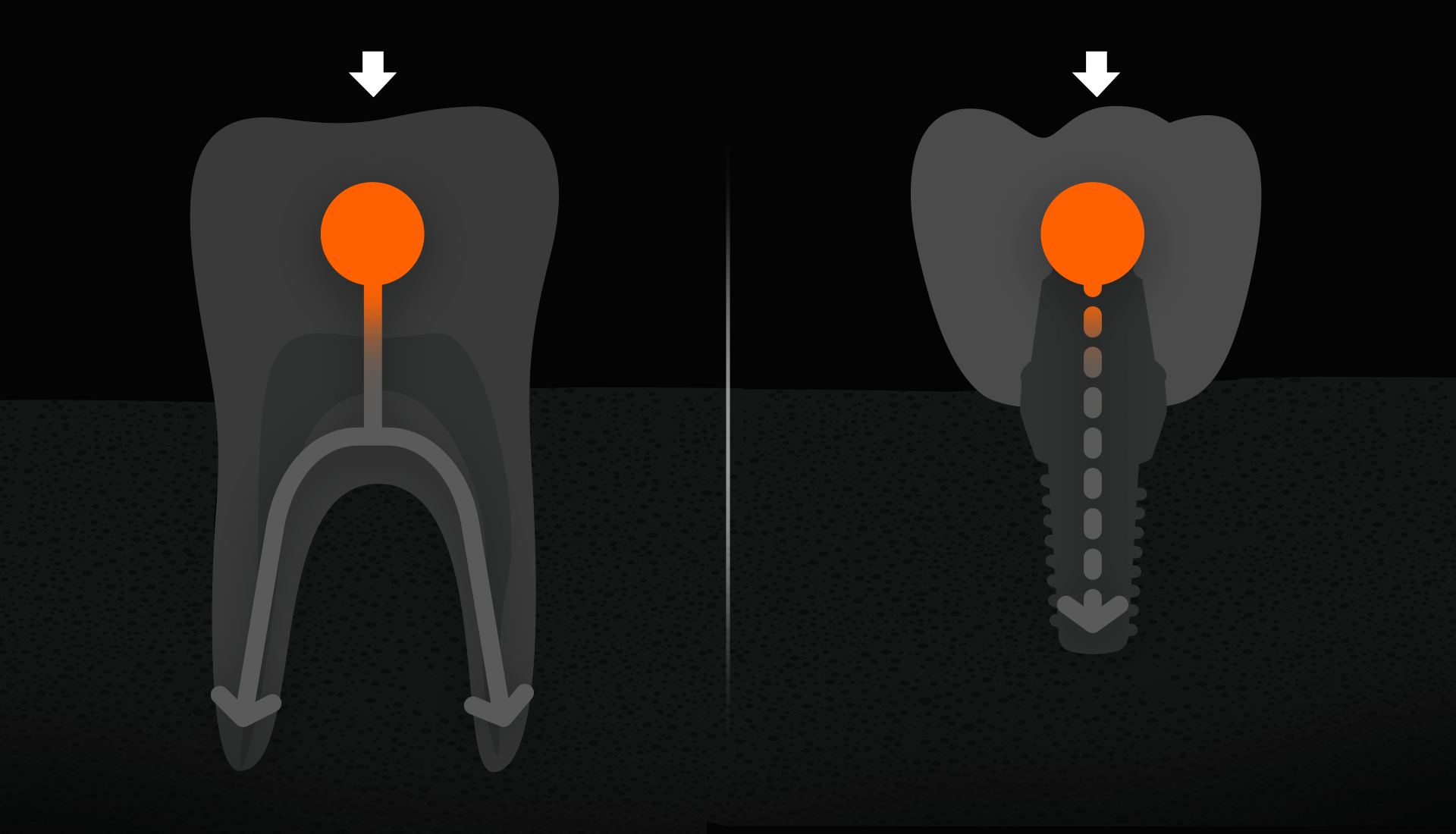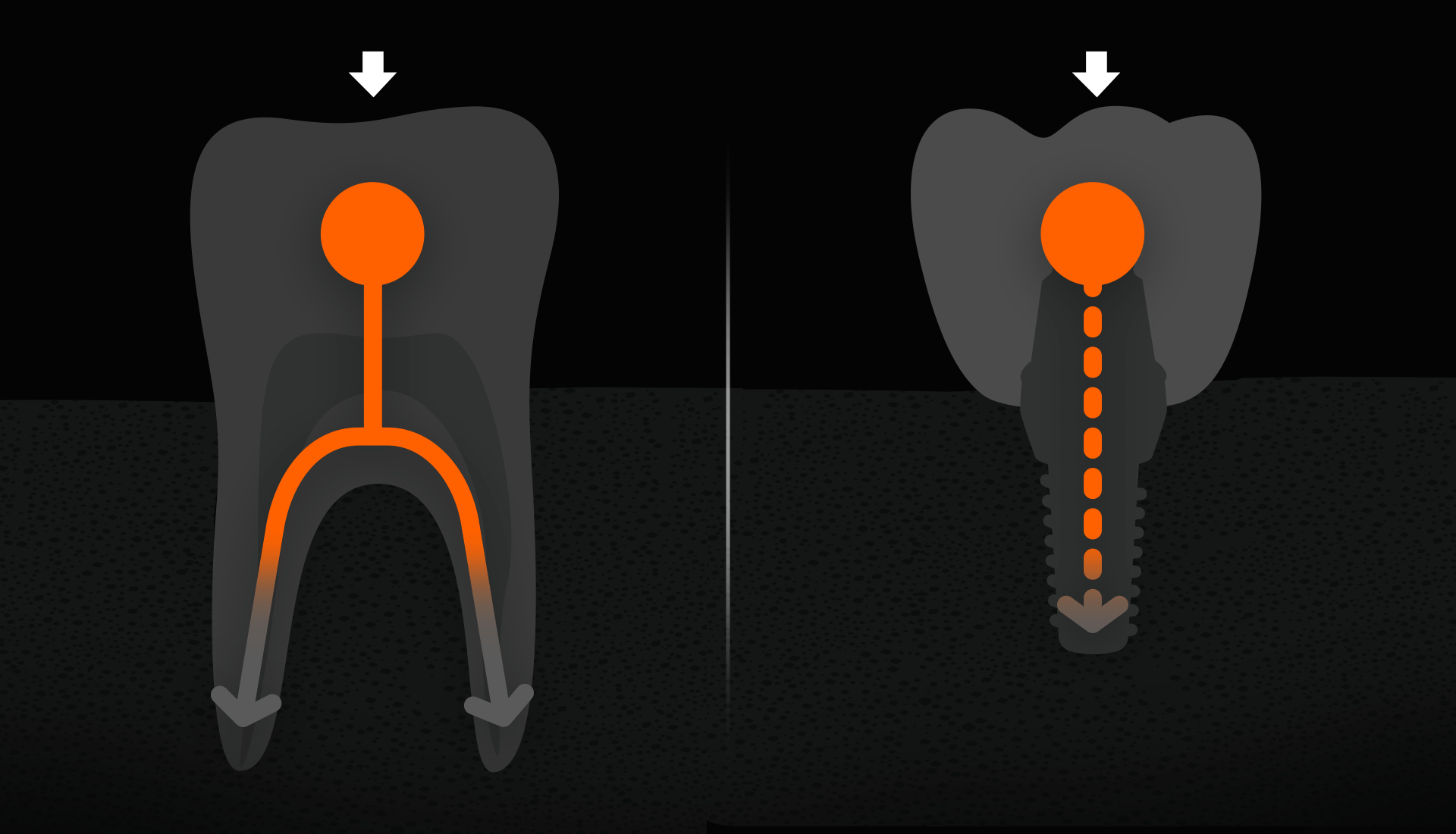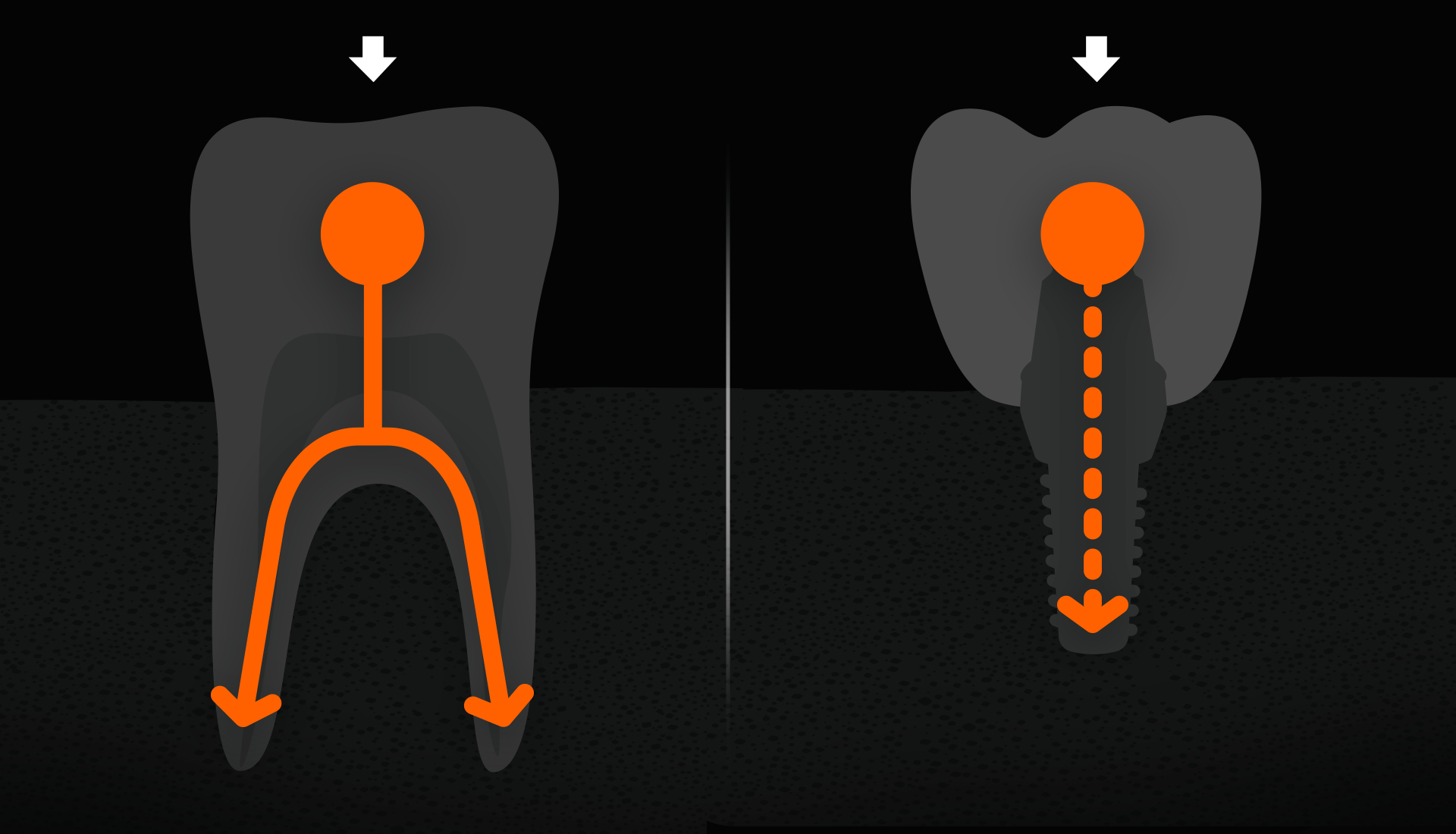
Molars receive the most force when chewing. Natural molars have multiple roots (3 for upper, 2 for lower) to distribute force efficiently, but an implant root is about half the size of a natural root. Therefore, placing one implant each in the premolar and molar areas helps distribute force and ensure stability.
The front teeth are smaller and receive less biting force, making it difficult to place an implant for every tooth. Generally, one implant is placed at each canine, and the middle part is connected to create six teeth.
3) Consideration of Cost and Practical Requirements
The financial burden of full-arch implants or other practical circumstances can also be a significant factor.
Rather than an over-engineered treatment, it is better to adjust the number of implants toward achieving maximum effect at the most appropriate level.
Summary: The number of implants must be determined through a customized approach considering the gum bone condition, distribution of biting force, and practical requirements.
3. Frequently Asked Questions (FAQ)
Q. What problems can occur if the number of implants is too low?
If the number is too low, excessive force (overload) is concentrated on each implant, increasing the risk of the implant shaking or the surrounding alveolar bone being absorbed. Especially in the molars, a minimum number of implants is crucial to secure sufficient support. Falling below the appropriate number may lead to prosthetic damage or a shortened lifespan for the restoration.
Q. Are All-on-4 or All-on-6 possible even if the gum bone (alveolar bone) is lacking?
Yes, All-on-4 and All-on-6 are treatments designed for cases with insufficient bone. By tilting the implants into the front area where the bone is densest, stable fixation can be achieved without bone grafting in many cases. However, if bone resorption is severe, additional bone augmentation may be required, so a precise diagnosis is necessary first.
Q. What is the difference in chewing power between full-arch implants and regular dentures?
Full-arch implants are fixed directly into the jawbone and provide chewing power similar to natural teeth, recovering over 80% of natural masticatory force. Conversely, regular dentures sit on top of the gums, providing only 10–20% of natural chewing power, making it difficult to eat tough foods and potentially causing gum pain.
Q. What preparations are needed to start treatment for an edentulous mouth?
First, a precise diagnosis using 3D CT scans and oral scanners is required. Through this digital implant analysis, the patient's bone condition can be accurately grasped to establish the optimal implant count and treatment plan. It is important to inform the medical staff about any medications (especially aspirin, blood pressure meds, etc.) and systemic diseases (diabetes, hypertension, etc.).
Full-arch implants are an important process for regaining your "quality of life." The best number of implants is not a fixed number, but the "optimal number" tailored to each patient's health, bone quality, and desired functional level.

Sources
- Korean Academy of Prosthodontics. (2023). Dental Implant Prosthodontics. Daehan Narae Publishing.
- Korean Academy of Oral & Maxillofacial Implantology. (2024). Implant Treatment Guidelines.
- Malo, P., Nobre, M. de A., Lopes, A. (2007). All-on-4 immediate function concept for completely edentulous maxillae: a clinical report. The International Journal of Oral & Maxillofacial Implants, 22(5), 717–724.
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



