If treatment is delayed after losing teeth, bone resorption, sinus expansion, and deterioration of bone quality make treatment more difficult and complex; therefore, it is best for patients not to delay treatment.
“It’ll be fine even if one is missing…”
You might have overlooked a missing tooth, only to be surprised a few months later when told that an implant is more complex and takes longer than expected. In this article, we will guide you through what changes accumulate in the mouth over time, why the difficulty of full-arch implants increases as a result, and the management methods you should practice right now.
1. What Happens Inside the Mouth After Tooth Loss?
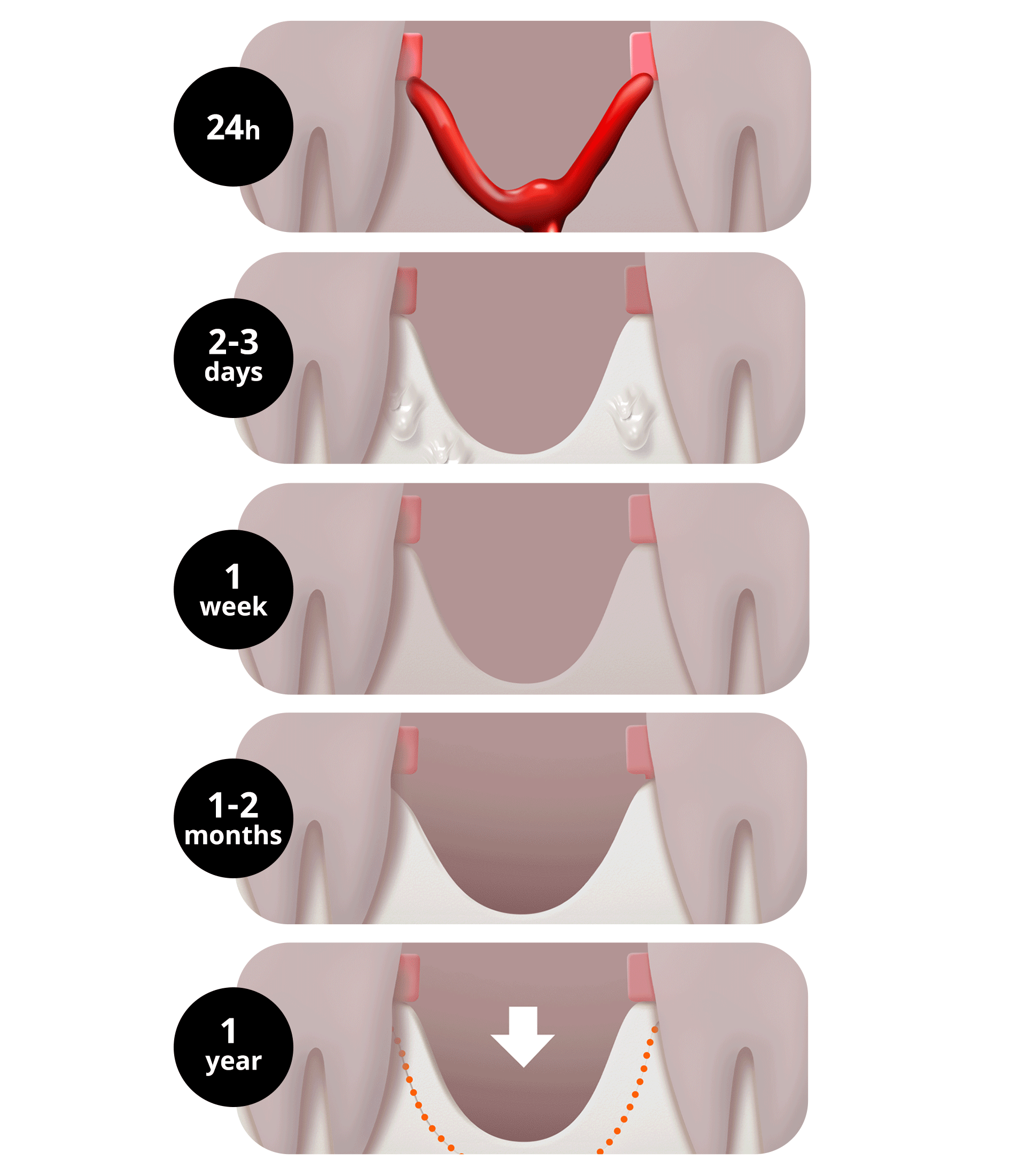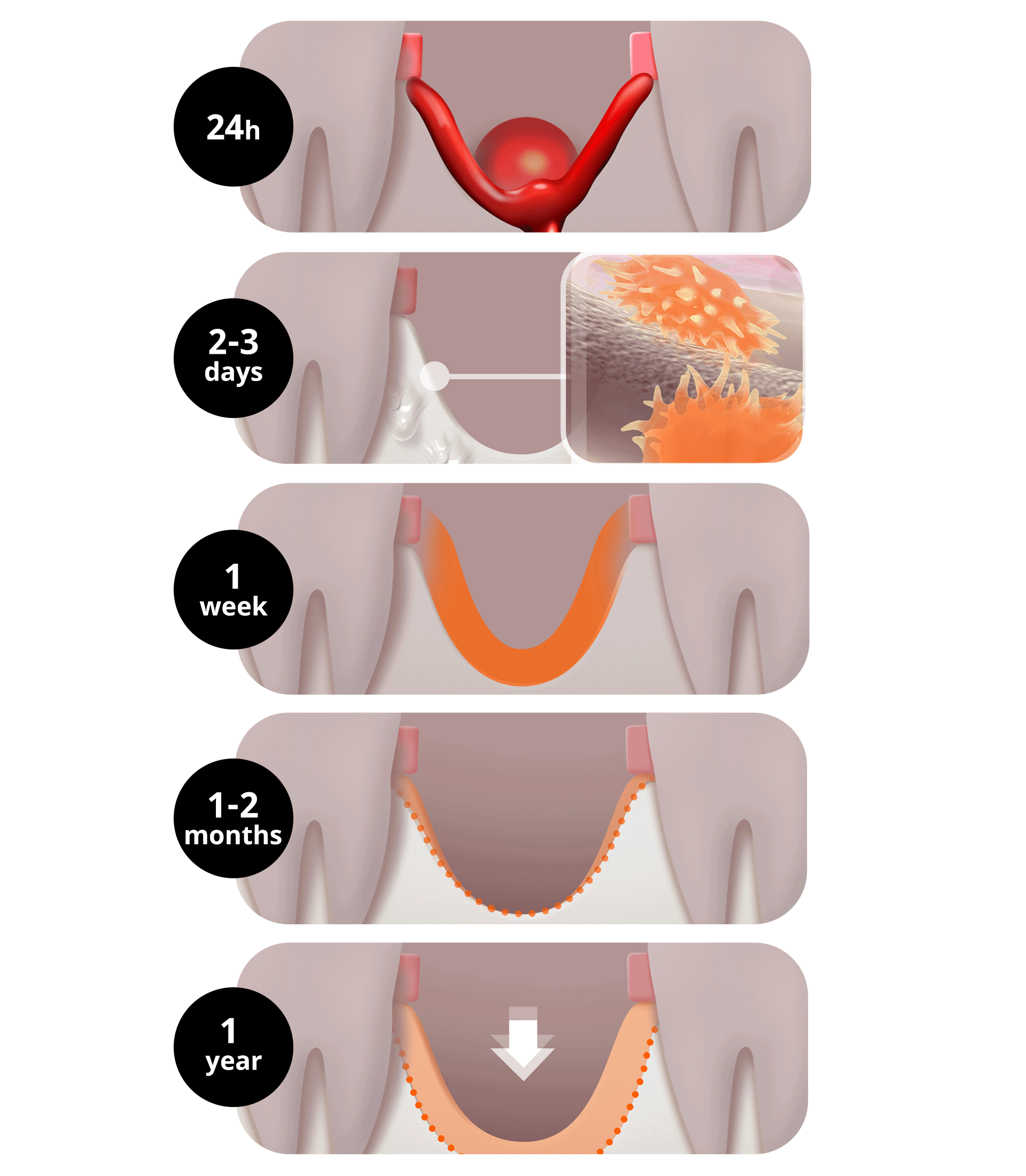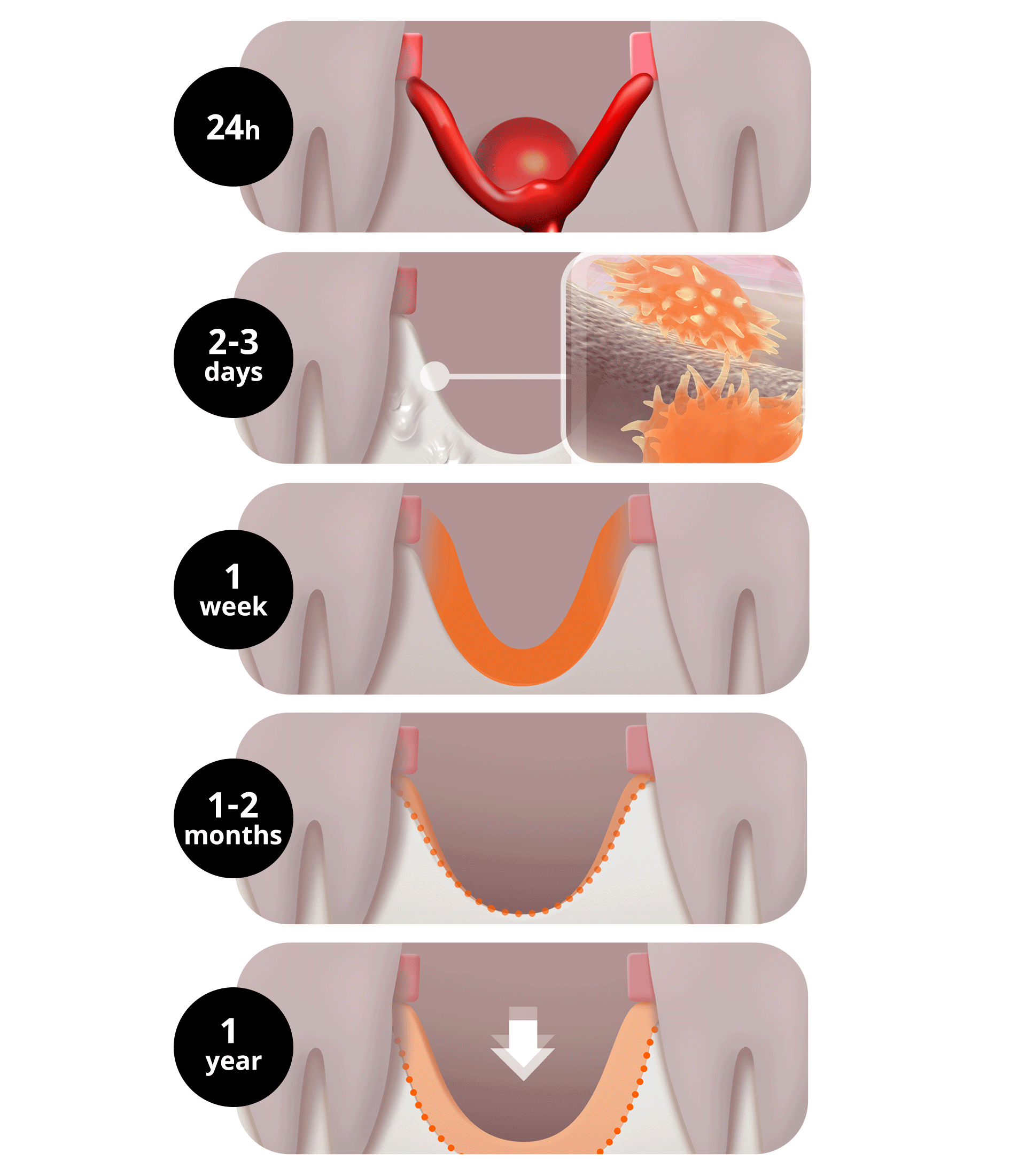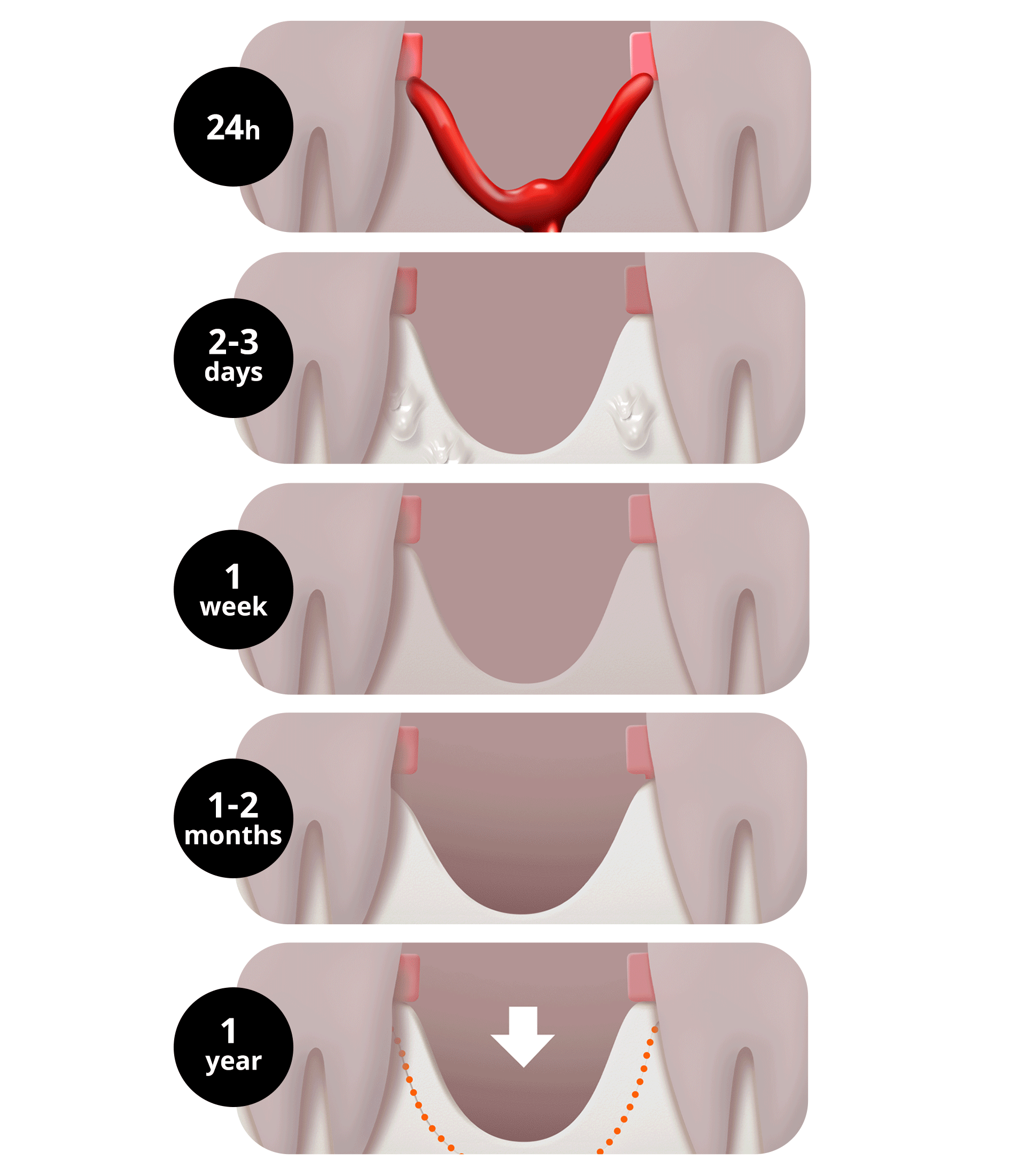
From the moment a tooth is lost, the alveolar bone (gum bone) no longer receives functional stimulation and begins to be resorbed. Just as the ground collapses when the pillars supporting a building disappear, the phenomenon of bone loss occurs.
- Immediately after extraction (~24 hours): Alveolar bone resorption begins. A blood clot (thrombus) forms and starts healing the extraction site.
- After 2–3 days: Wound healing begins in earnest. Osteoblasts and osteoclasts become active.
- After 1 week: The blood clot is gradually replaced by granulation tissue.
- After 1–2 months: New bone begins to form little by little, but since this is not complete bone, the height and width of the alveolar bone continue to decrease.
- Within 3 months of extraction: About two-thirds of the alveolar bone volume disappears, and the most severe resorption occurs.
- After 1 year: Up to half of the original bone can be lost, and the bone continues to decrease gradually thereafter. Especially in areas where the original bone is thin, such as the upper front teeth, bone loss appears more severely.
2. Differences in Bone Loss After Tooth Loss
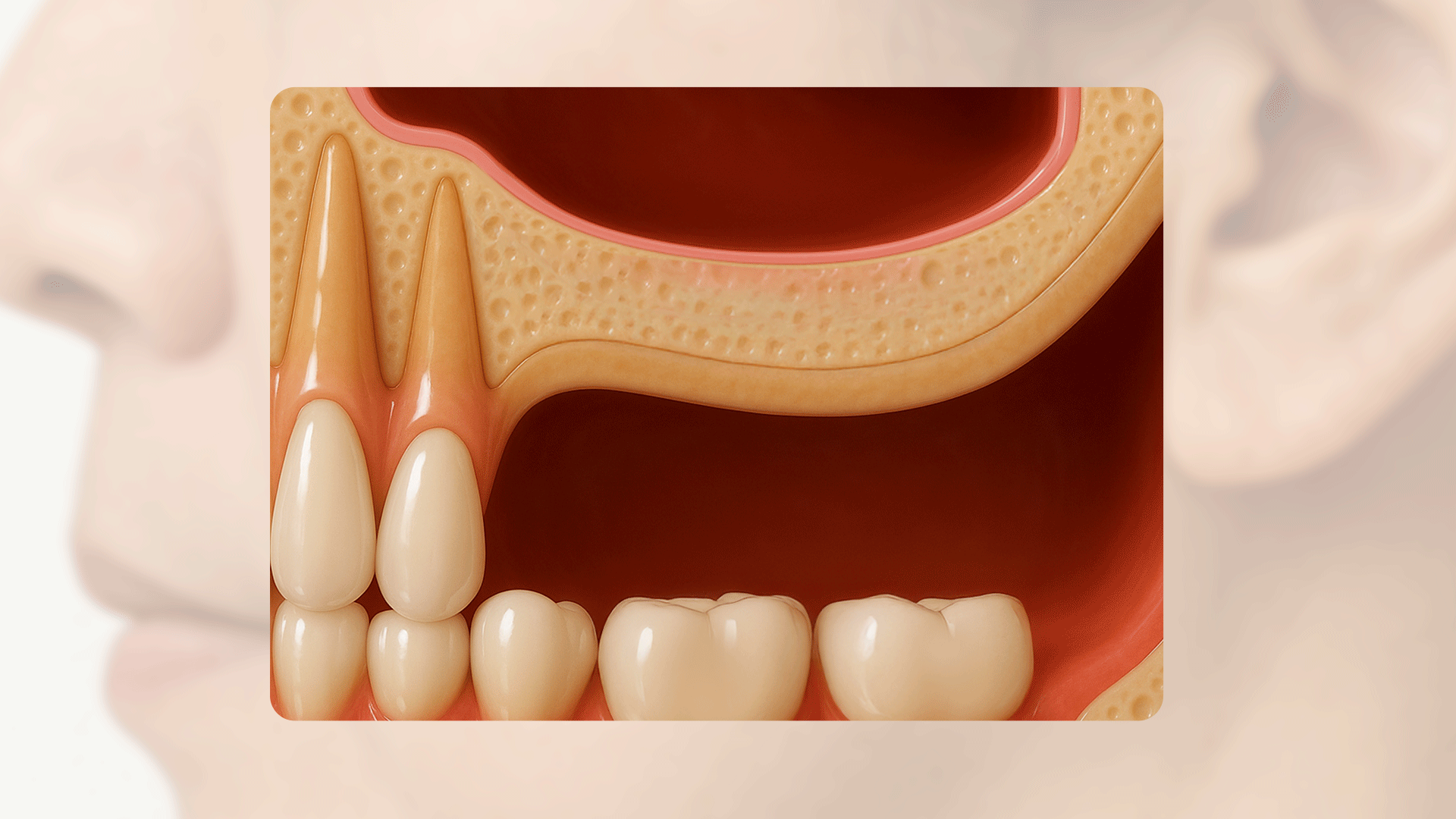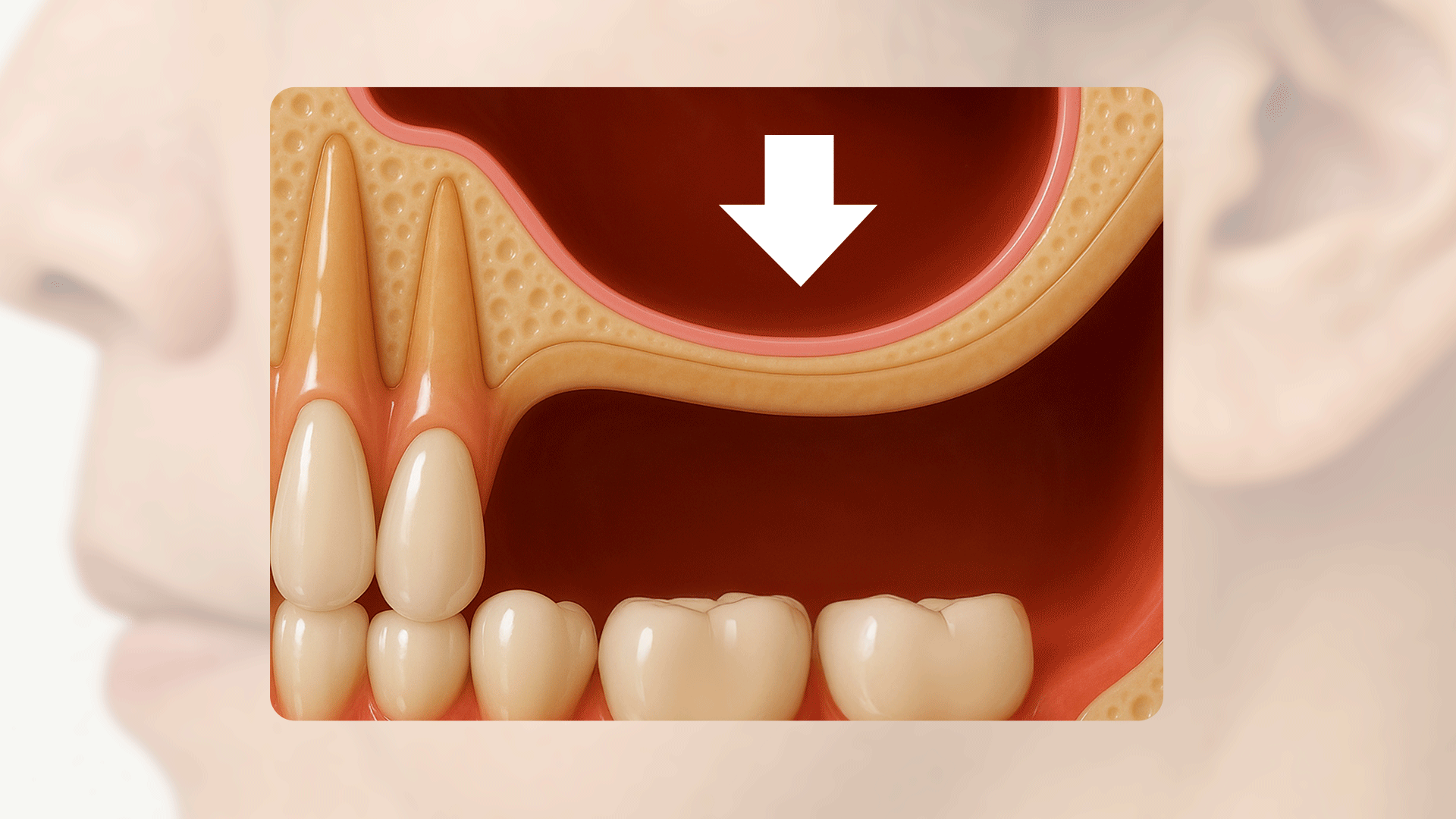
Bone loss appears differently depending on whether it is the upper or lower jaw and the position of the tooth. Generally, bone resorption progresses more dramatically in the upper jaw (maxilla) than in the lower jaw (mandible), and in the front teeth area than in the molar area.
In particular, if an upper molar is missing, the maxillary sinus—a hollow space located inside the upper jawbone—expands downward simultaneously with jawbone resorption. This can lead to a situation where the amount of bone available for implant placement becomes woefully insufficient.
It is not just the volume of bone that decreases over time. The quality of the bone itself also deteriorates. For example, the bone in the upper molar area is originally thin and has low mineral content, often making it difficult for an implant to be firmly fixed.
Such poor bone quality negatively affects the "osseointegration" process—where the implant and bone fuse firmly—and can lower the implant success rate. Implants are not successful simply because there is a lot of bone; success rates can be increased only when there is sufficient healthy and strong bone.
3. Reasons Why Implants Become Difficult as Time is Delayed

1) The required amount of bone grafting increases.
For long-term stability, an implant must be surrounded by healthy bone at least 2mm thick.
However, as mentioned earlier, if a lot of bone has been resorbed after tooth loss, "bone grafting"—supplementing the bone volume using graft materials—is essential.
Placing an implant forcibly without a bone graft may result in the implant not being sufficiently surrounded by healthy bone, which can lead to the implant shaking or falling out in the long term. Bone grafting, verified through numerous clinical studies and success stories, is a safe and effective treatment.
2) Additional surgeries may be required.
If bone volume becomes insufficient after a period following tooth loss, it is difficult to resolve with standard full-arch implant surgery. In the case of the upper jaw, the bone becomes too thin due to the expanded maxillary sinus, necessitating an additional procedure called a "sinus lift."
In the case of the lower jaw, the distance to the nerve canal becomes closer, creating difficulties in determining the implant placement position.
These additional procedures not only make the treatment process complex but can also increase the treatment period and the patient's discomfort.
3) Periodontal disease may occur.

If you lost natural teeth due to severe periodontal disease, the same problem can occur with implants if you do not change your existing eating or oral hygiene habits. This is "peri-implantitis."
Implants do not get cavities, but if inflammation occurs in the surrounding gums, the bone around the implant can melt away, leading to the unfortunate event of having to remove the implant. After receiving full-arch implant surgery, more meticulous management and regular check-ups are essential.
4) Treatment costs increase.
When additional surgeries such as bone grafting or sinus lifts are accompanied, the treatment process naturally becomes complex. The treatment period also inevitably becomes longer. This increase in complex procedures naturally leads to a rise in the cost of full-arch implant treatment.
Issues that could have been easily resolved if treated early result in major surgery and high costs as time passes.
Additionally, complex surgeries can cause various discomforts such as gum swelling, food impaction, and prosthetic damage, and can also increase the possibility of complications.
4. Frequently Asked Questions (FAQ)
Q. It has been quite a while since I lost my teeth. What additional treatment do I need to get implants now?
If a long time has passed since tooth loss, it is very likely that the space to place an implant is insufficient because a lot of bone has been resorbed. Therefore, you should consider bone grafting almost essential. Especially in the upper molar area, the bone may have thinned while the maxillary sinus has descended, which may require a high-difficulty additional surgery called a sinus lift. These additional treatments are major causes of increased duration and cost for full-arch implants.
Q. Is bone grafting absolutely necessary before placing an implant? Can't it just be placed where there is a lot of bone?
For long-term stability, an implant must be surrounded by healthy bone at least 2mm thick. Forcing an implant into a state of insufficient bone increases the failure rate because the implant cannot be surrounded by a sufficient amount of hard bone. Furthermore, it can lead to the bone around the implant melting in the long term, causing the implant to shake or fall out. Bone grafting is a safety device to increase the long-term success rate of the implant.
Q. They say a lot of bone disappears within 3 months after extraction. Should I get the implant immediately after pulling the tooth?
The most ideal approach is early intervention to preserve bone from immediately after extraction. It is best to visit a dentist and consult with medical staff immediately after a tooth is lost. While "immediate implant placement after extraction" is possible in some cases, it depends on the infection or bone status. In any case, starting a professional diagnosis and preservative treatment within 3 months—when the most bone is resorbed after extraction—is the key to reducing the difficulty, duration, and cost of future implants.
Q. If I pulled a tooth because of severe gum disease, can the implant fall out due to the same problem?
Yes, it is possible. If the causes of the periodontal disease that led to the loss of natural teeth (bad eating habits, poor oral hygiene management, etc.) are not improved, "peri-implantitis" can occur, where inflammation develops in the gums around the implant. If peri-implantitis becomes severe, the bone around the implant can melt away, and eventually, the implant may need to be removed. Therefore, even after treatment, meticulous management and regular dental check-ups are very important in determining the longevity of the implant.
Q. How much longer does implant treatment take if a bone graft is done?
It depends on the amount and difficulty of the bone graft, but usually several months (more than 3–6 months) of additional recovery time may be required until the grafted bone becomes completely hard and can safely support the implant. Since bone grafting is an important process for the success of implant placement, it is essential to have a sufficient recovery period following the instructions of the medical staff to ensure the stability of the implant.
Tooth loss is not just a simple inconvenience but the beginning of serious changes that cause alveolar bone resorption and deterioration of bone quality. The key to reducing the difficulty and cost of implant treatment and increasing the success rate lies in early intervention without wasting time. Do not leave missing teeth neglected; consult an expert right now to start a plan to regain a healthy smile and oral function.

Sources
- Korean Academy of Periodontology. (2022). Management of Peri-implant Tissue and Bone Grafting Guide.
- Korean Academy of Prosthodontics. (2023). Principles of Implant Prosthodontic Treatment for Edentulous Patients.
- Araujo, M., & Lindhe, J. (2011). Dimensional ridge alterations following tooth extraction. Journal of Clinical Periodontology, 38(s11), 187–196.
※ The copyright for all content on this blog belongs to Medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



