This guide outlines the timing, procedure, and differences between All-on-4 and All-on-6 for patients in their 50s and 60s who require full-mouth restoration.
"I heard it’s better to just pull them all and get implants..."

You may have heard this from acquaintances, but when it becomes your own reality, the decision is much harder. Many patients in their 50s and 60s—especially those with a few remaining teeth or those currently wearing dentures—find themselves torn between the fear of extraction and the daily discomfort of failing teeth.
Full-mouth implants are more than just "planting" teeth; they are a comprehensive treatment to restore biting force, aesthetics, and the structural stability of the mouth. This post explains when this treatment is necessary and clarifies the latest methods, including All-on-4, All-on-6, and Full-mouth implants.
1. When is a Full-Mouth Implant Necessary?
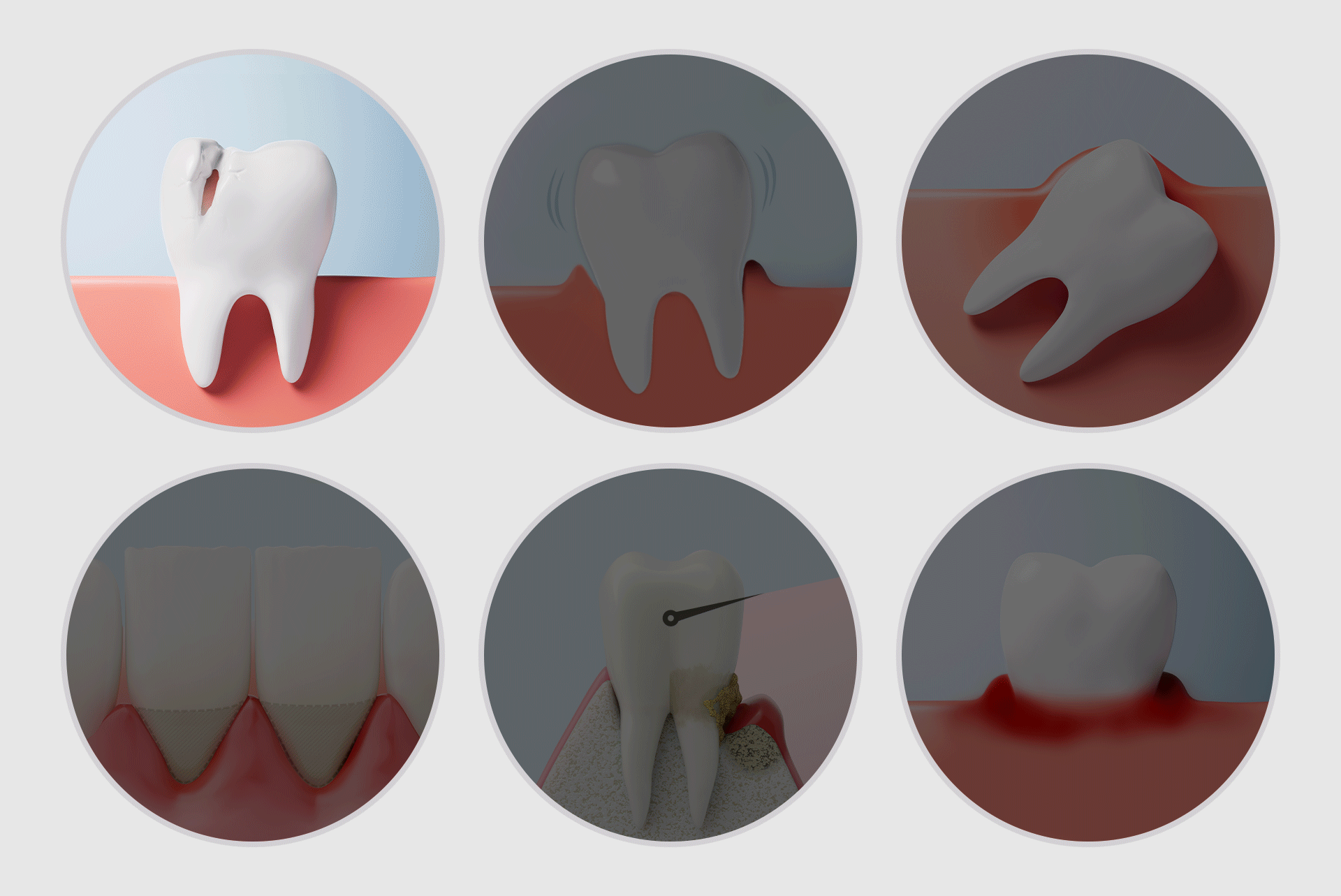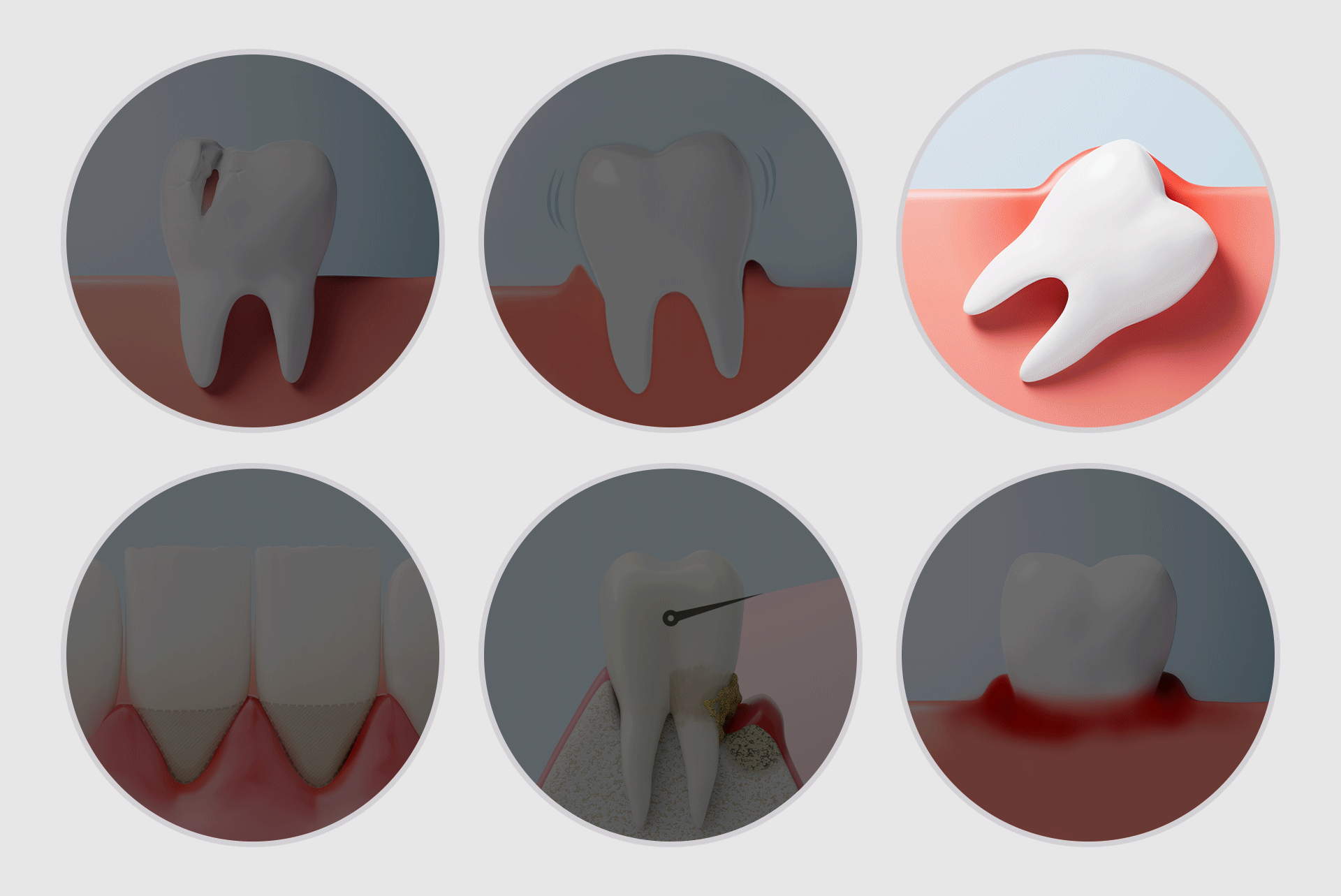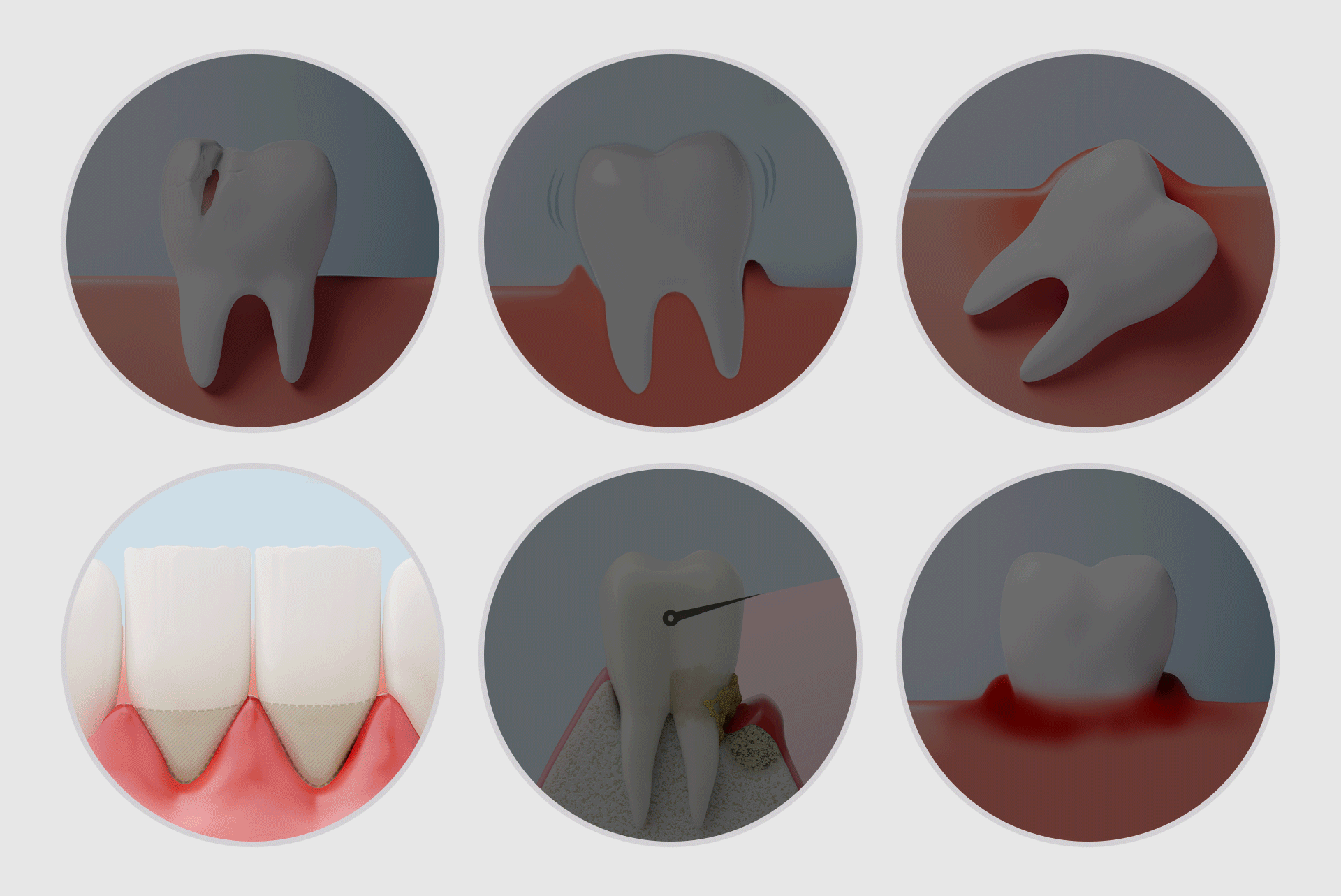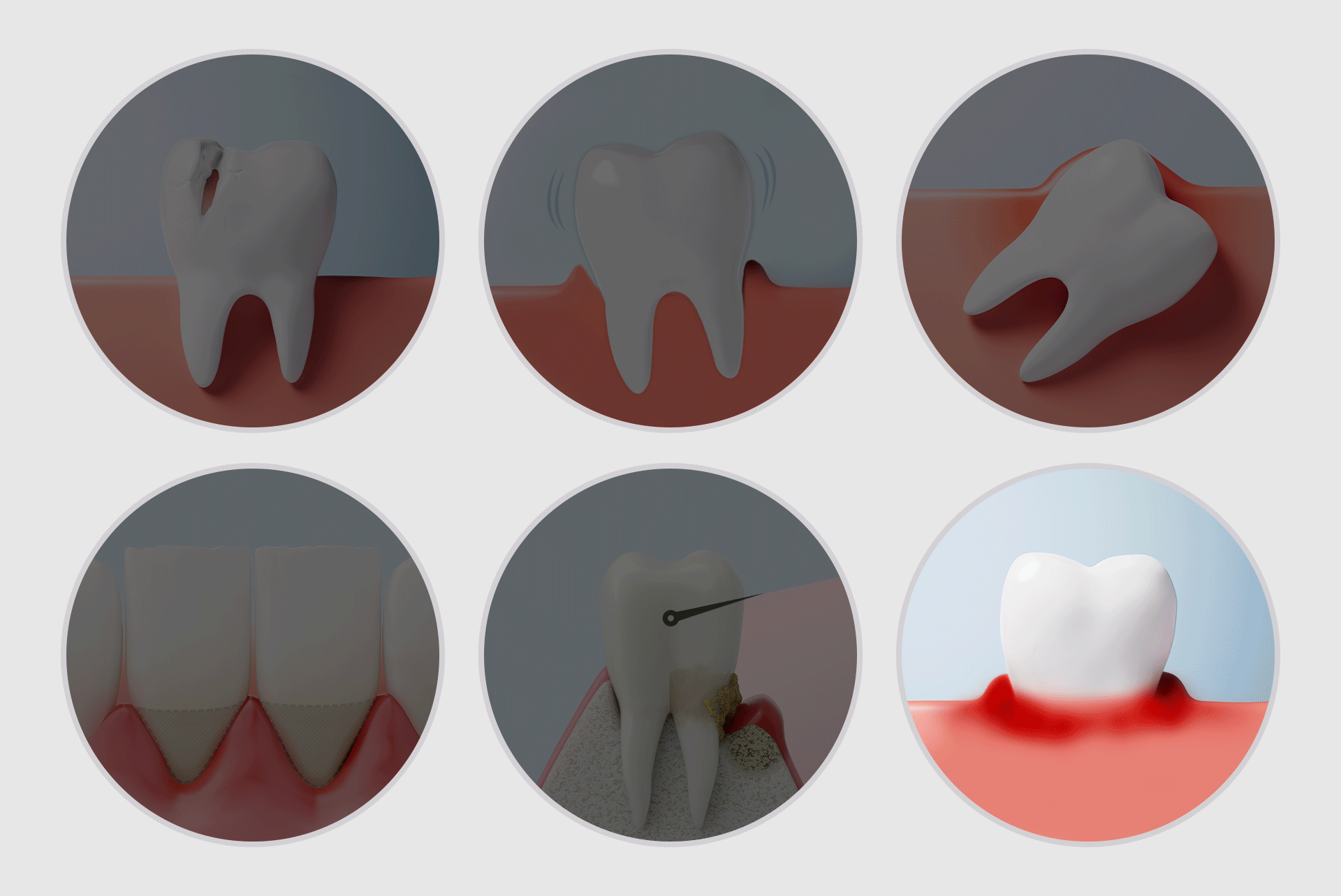
Implants are not just for replacing missing teeth; they are needed when the overall balance of the mouth collapses due to functional decline or weakened jawbone. Here are six representative situations:
- Teeth are present but non-functional: Poor chewing ability affects digestion and nutritional intake. If remaining teeth are mobile and painful, they have effectively lost their function.
- Severe gum disease causing tooth mobility: Periodontitis destroys the supporting tissue. If teeth continue to shake despite repeated treatments, full-mouth restoration may be required.
- A collapse of balance due to repeated "patchwork" treatments: Continual partial treatments can lead to occlusal imbalance and overload, causing a chain reaction of failure in the remaining teeth.
- Weakened jawbone from long-term denture use: Dentures accelerate bone resorption over time. As the bone diminishes, the stability for future implants becomes more challenging to achieve.
- Neglected dental health due to delay: Postponing treatment due to dental phobia or financial concerns often leads to visiting the clinic only after acute pain starts, by which time multiple teeth may be unsalvageable.
- Teeth weakened by genetic factors or systemic diseases: Conditions like diabetes, osteoporosis, and rheumatism can accelerate bone loss, requiring a holistic management approach.
2. Types of Full-Mouth Implants
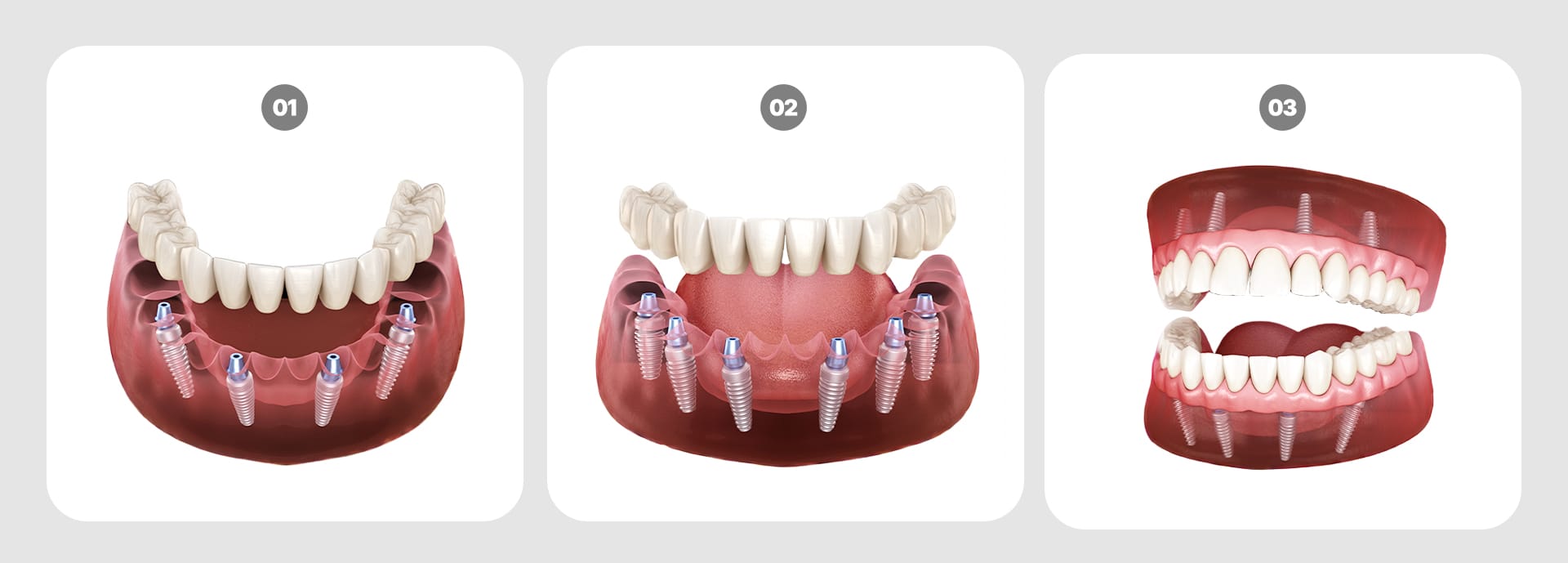
The method chosen depends on the condition of the remaining teeth and jawbone.
- All-on-4:
- Supports a full arch with only four implants.
- Often possible without bone grafting, reducing surgical burden.
- Allows for the attachment of temporary teeth on the same day.
- All-on-6:
- Provides stronger support with six implants.
- Ideal for patients with a weaker jawbone.
- Offers superior long-term durability and maintenance.
- Full-Mouth Implants:
- Typically involves placing 6 or more implants per arch.
- Necessary for patients with total tooth loss or long-term denture users.
- Often involves bone grafting to ensure maximum stability.
3. The Procedure for Full-Mouth Implants
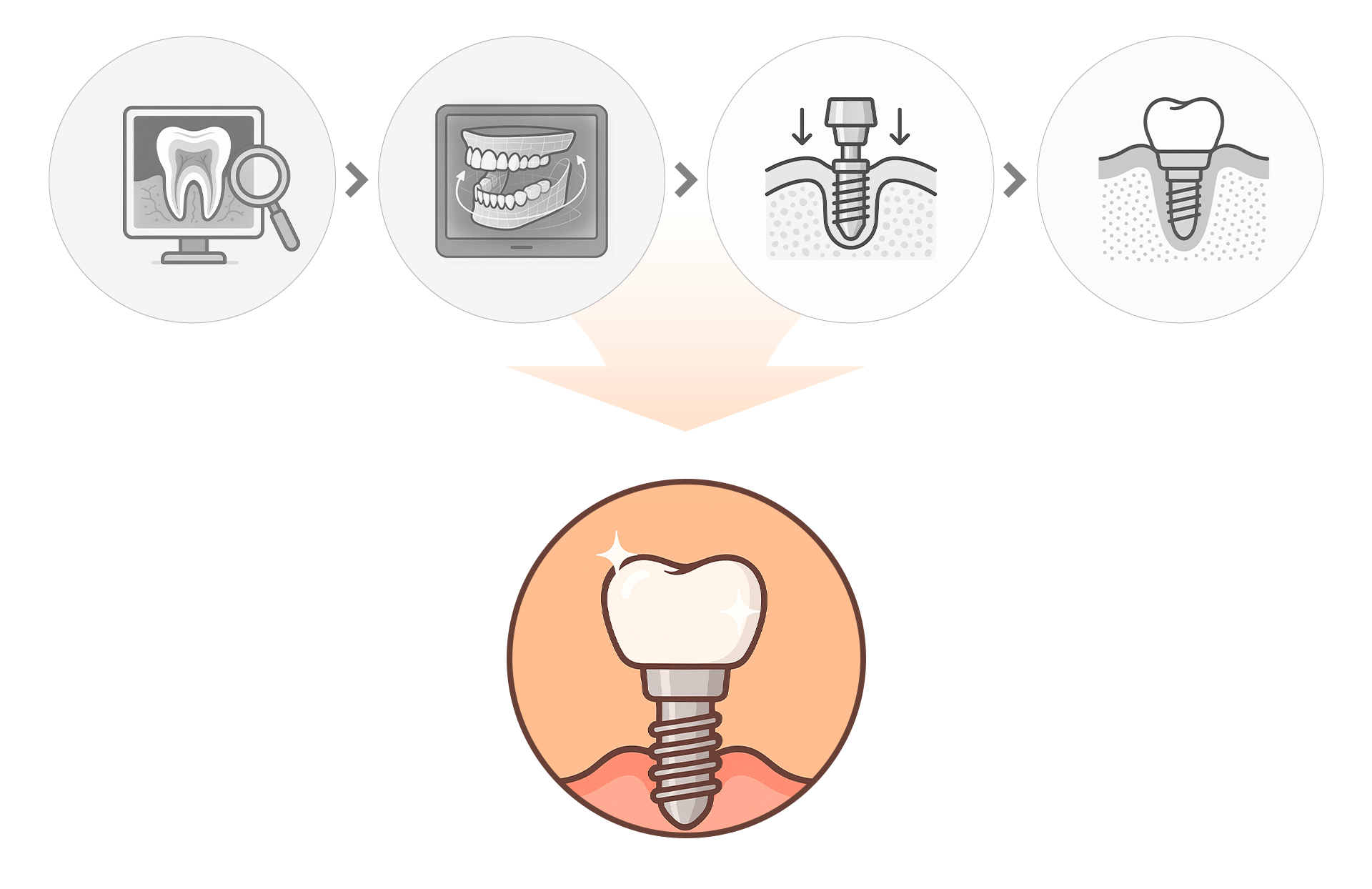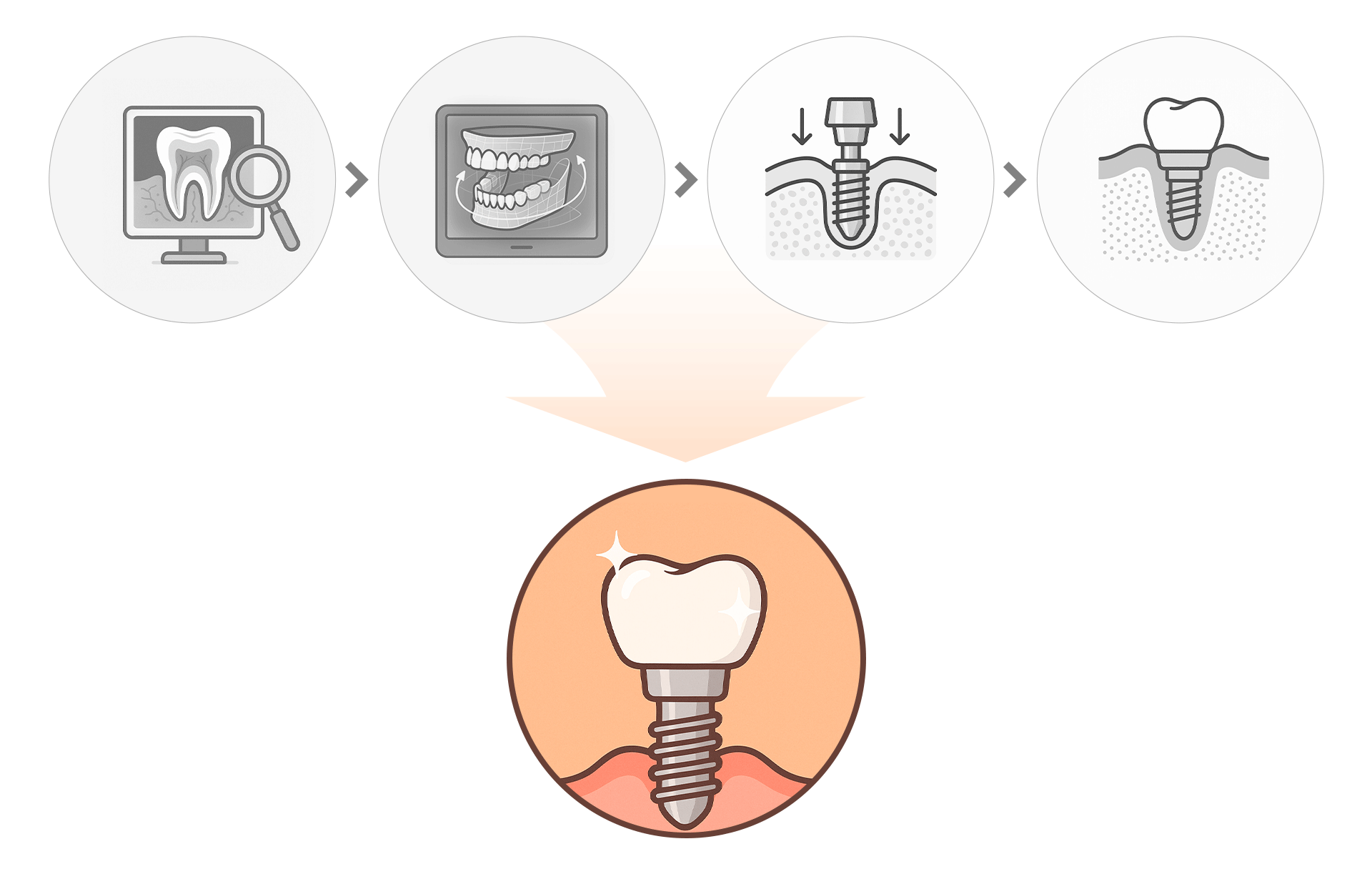
This process is a precise engineering task based on digital diagnostics.
- Precision Diagnosis: X-rays and 3D CT scans to check bone and nerve positions.
- Digital Analysis: Using oral scanners and CAD/CAM to create customized surgical guides.
- Implant Placement: Placing 4–6 implants, with temporary teeth attached on the same day if possible.
- Osseointegration Period: A 2–6 month healing phase where the bone and implants fuse.
- Final Prosthetic Attachment: Crafting and attaching the final customized bridge to complete the bite and aesthetics.
4.Frequently Asked Questions (FAQ)
Q. Why are full-mouth implants better than dentures?
They provide vastly superior stability, allowing you to chew naturally. They also preserve the jawbone, preventing facial sagging, and feel much more natural. Most importantly, there is no need to remove them at night.
Q. Is bone grafting absolutely necessary?
If the bone is thin or weak, it is essential for success. However, techniques like All-on-4 can sometimes avoid bone grafting by tilting the implants into areas with higher bone density.
Q. Can I eat on the day of surgery?
Yes, if the bone density is sufficient and the surgery is stable, temporary teeth can be attached for immediate function. This is known as "immediate loading," allowing you to speak and eat soft foods right away.
Q. Are these possible for elderly patients?
Age is not the primary factor; systemic health and bone volume are. If conditions like diabetes or high blood pressure are well-managed, patients in their 70s or 80s can successfully receive full-mouth implants.
Q. When is the best time to start treatment?
The best time is when you first notice your chewing function declining. Waiting until all teeth are lost can lead to severe bone loss, making the eventual treatment more complex and costly.

Full-mouth implants are not just a dental procedure; they are a treatment to reclaim your quality of life. The first step is getting an accurate diagnosis rather than letting symptoms worsen. We recommend consulting with an experienced medical team to discuss the best path forward for your specific needs.
Sources
- Pjetursson, B. E., et al. (2014). “A systematic review of the survival and complication rates of implant-supported fixed dental prostheses (FDPs) after an observation period of at least 5 years.” Clinical Oral Implants Research, 25(6), 576–592.
- Korean Academy of Oral & Maxillofacial Implantology. (2023). 임플란트 치료 가이드라인.
- Esposito, M., et al. (2013). “Interventions for replacing missing teeth: Different types of dental implants.” Cochrane Database of Systematic Reviews.
※ The copyright for all content on this blog belongs to Medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads