When it comes to thyroid dysfunction, it is difficult to accurately distinguish the condition based on symptoms alone. That is why understanding the correlation between blood test numbers (TSH, Free T4) is crucial. Here, we outline the decisive differences between hyperthyroidism and hypothyroidism, their respective treatment directions, and why the focus should be on 'management' rather than a 'complete cure'.
"Doctor, what exactly is the difference between hyper and hypo?", "How long do I need to take this medication?"

The names are similar and easy to confuse, but these two conditions have entirely opposite causes and treatment directions. Rather than relying on unverified information online, it is important to understand the principles behind your body's numbers.
If you have felt anxious about your treatment due to confusing terminology, this guide will help you establish clear criteria for judgment.
1.Why Differentiate with Numbers When Symptoms Overlap?

Managing the thyroid in our body is similar to 'driving a car'. Thyroid hormone (Free T4) is the 'fuel' that runs the engine, and Thyroid Stimulating Hormone (TSH) is the 'dashboard signal' sent by the brain to control the speed. Applying this analogy makes the flow of both conditions clear:
- Hyperthyroidism (Speeding): A state where there is excessive fuel, causing the engine to overheat. Because the car keeps running without stopping, you cannot tolerate heat, your heart beats fast (tachycardia), and you lose weight as you burn through all your energy.
- Hypothyroidism (Stalled): A state where the engine is shutting down due to a lack of fuel. You feel cold easily, and because your metabolism slows down, you gain weight and experience swelling even without an appetite.
The key point to note is that symptoms of the two conditions can overlap. For instance, 'extreme fatigue' or 'muscle weakness' can appear in both. Particularly in older adults, hyperthyroidism may present only with a loss of appetite and lethargy, making it easy to misinterpret based on symptoms alone. Therefore, medical professionals look at the 'paradox of numbers'. The dashboard (TSH) and the actual speed (T4) move in opposite directions.
- Hyperthyroidism: If there is too much hormone (T4), the brain commands production to stop. Thus, the stimulating hormone (TSH) level is suppressed below normal.
- Hypothyroidism: If hormone (T4) is lacking, the brain shouts to produce it quickly. Therefore, the stimulating hormone (TSH) level rises above normal.
In short, remember the principle that 'your body's hormone (T4)' and 'the brain's signal (TSH)' move inversely.
[Identifying Subclinical (Asymptomatic) Conditions through Numbers]
- Subclinical Hyperthyroidism: Low TSH level / Normal Free T4 level
- Subclinical Hypothyroidism: High TSH level / Normal Free T4 level
Even without symptoms, whether to proceed with follow-up observation is determined based on the numerical pattern and risk factors (age, cardiovascular disease, etc.).
2.'Graves' and 'Hashimoto', What is My Diagnosis?
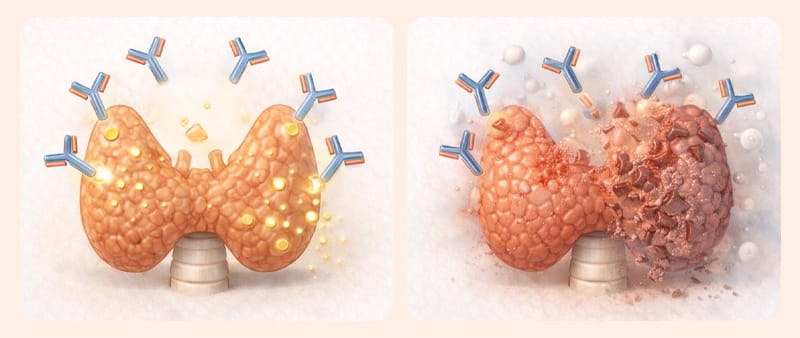
Before understanding the diagnosis, it is necessary to differentiate between 'thyrotoxicosis' and 'hyperthyroidism'.
Thyrotoxicosis refers to a 'state' (overheated engine) where there are high levels of hormones in the blood, regardless of the cause. If hormones temporarily leak due to thyroiditis, it falls under thyrotoxicosis, but it is different from 'hyperthyroidism' where the factory itself is overheated. Distinguishing between the two prevents the unnecessary use of antithyroid medications.
The core to identifying the true cause is the 'autoimmune antibody'. Graves' disease is the primary cause of hyperthyroidism. Immune cells create an antibody (TRAb) that forces the engine's accelerator pedal down, causing the thyroid to endlessly pump out hormones.
On the other hand, Hashimoto's thyroiditis is the main cause of hypothyroidism. Immune cells cause inflammation that slowly damages the engine itself, eventually reducing its hormone production capacity.
[Checking the Antibody Names on Your Test Results]
- TSH Receptor Antibody (TRAb): If positive, there is a high likelihood of Graves' disease (hyperthyroidism).
- Anti-Thyroid Peroxidase Antibody (TPOAb): If positive, there is a high likelihood of Hashimoto's thyroiditis (hypothyroidism).
3.When Medication Isn't Enough for Hyperthyroidism Treatment
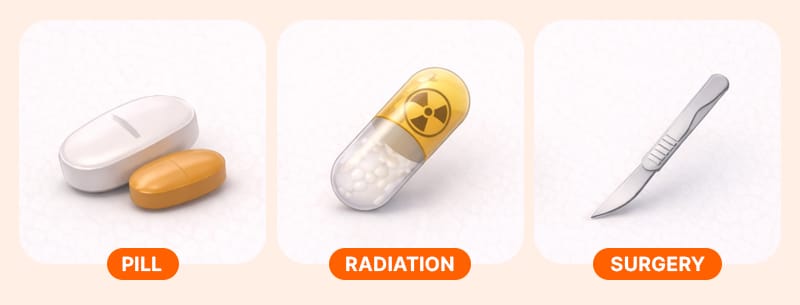
If diagnosed with hyperthyroidism, the primary goal of treatment is to 'cool down the overheated engine'. Domestic clinical guidelines strongly recommend taking antithyroid drugs (Methimazole, PTU, etc.) as the first step.
However, if medication side effects (elevated liver enzymes, rashes, etc.) are severe or relapses are frequent, other methods must be considered. The characteristics of the main treatments are as follows:
| Treatment | Principle and Characteristics | Recommended For |
|---|---|---|
| Antithyroid Drugs | Suppresses hormone production. The most common first-line treatment. | Most patients, including pregnant women, children, and first-time patients. |
| Radioactive Iodine | Destroys excess cells with radiation. Possibility of lifelong hypothyroidism. | When there are medication side effects or frequent relapses. |
| Surgery | Removes thyroid tissue. Has the lowest recurrence rate but leaves a scar. | When the thyroid is very large or cancer is suspected. |
Particularly, Radioactive Iodine (RAI) therapy is advantageous for lowering recurrence rates, but caution is needed if active Thyroid Eye Disease (TED) is present, as it can worsen symptoms. During treatment, TSH and Free T4 levels must be periodically checked to adjust the medication dosage.
4.Hypothyroidism Medication: Do I Have to Take It for Life?
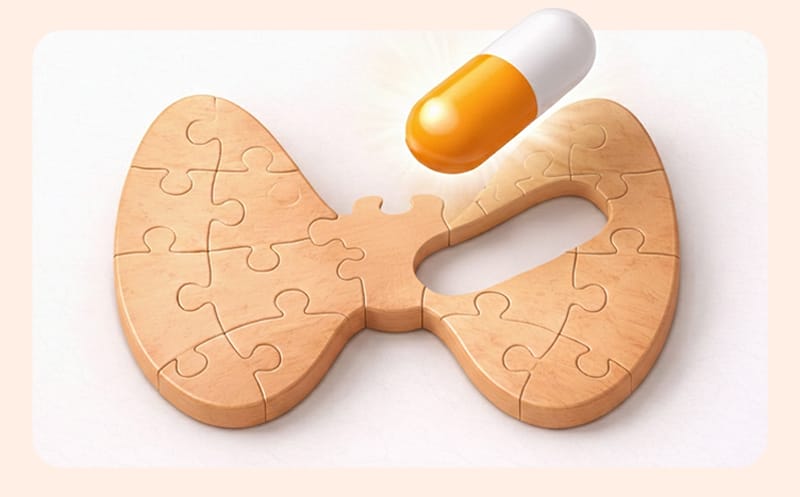
The core of hypothyroidism treatment is to replenish the lacking fuel from the outside. The Levothyroxine used here is not just a simple drug; it is a concept of directly supplementing the hormone that our body cannot produce.
Therefore, rather than worrying, "Will I build a tolerance by taking medication?", it is safer to understand it as "maintaining normal function to prevent complications." The duration of taking the medication varies depending on the cause. If the thyroid was removed via surgery or its function is lost long-term due to Hashimoto's thyroiditis, long-term administration is required.
However, if it is a temporary cause such as postpartum thyroiditis, the medication may be stopped based on the medical staff's judgment. In particular, subclinical (asymptomatic) hypothyroidism has more detailed treatment criteria. This is when TSH is high but T4 is normal.
- Treatment Recommended: TSH 10 mIU/L or higher, planning for pregnancy, high cardiovascular risk group, or accompanied by severe symptoms.
- Observation: Elderly, slightly elevated levels with no symptoms.
Using medication unnecessarily in the latter case can actually harm bone health or increase the risk of arrhythmias. 'Always taking medication' is not the answer; the decision should be tailored to your body's specific risks (age, cardiovascular disease, etc.).
[Good Points to Check During Consultation]
- Is my current condition temporary inflammation or a chronic autoimmune disease?
- What are the specific numerical criteria for reducing or stopping the medication?
- Are there any precautions regarding heart palpitations or bone health management during the treatment process?
5.Why 'Remission' and 'Long-term Management' are the Goals, Not a 'Complete Cure'

Many patients ask, "When can I stop taking the medication completely?", but thyroid diseases should be approached with the concepts of 'remission' and 'management' rather than an 'absolute end' to reduce confusion.
Hyperthyroidism, especially Graves' disease, aims for a 'remission' state where hormone levels remain normal after medication treatment.
However, since a risk of relapse is reported within the first year after stopping the medication, regular check-ups are essential even without symptoms. Remission is not the 'end' but a 'stable period requiring observation'.
The same goes for hypothyroidism. Just like checking a car's engine oil periodically, the 'long-term management' of consistently adjusting the hormone concentration your body needs is the treatment itself.
Stopping the medication arbitrarily just because levels are normal can slow down your metabolism again and increase the risk of hyperlipidemia or heart disease. Thyroid treatment is not a sprint, but a marathon of pacing your body throughout your life.
6.Frequently Asked Questions(FAQ)
Q. My T4 level is normal but only my TSH level is abnormal. Do I need treatment?
Retesting and risk assessment take priority over immediate medication. This is called 'subclinical (asymptomatic) thyroid dysfunction'. Treatment is considered if the TSH level is high at 10 mIU/L or above, or low at below 0.1, but mild cases are often just observed. However, if you are preparing for pregnancy or have heart disease, you should consult with your medical staff to take proactive measures.
Q. Does taking thyroid medication make you gain or lose weight?
It is not a side effect of the medication, but a process of metabolism normalizing. Taking hypothyroidism medication (hormone pills) normalizes a slowed metabolism, which can reduce swelling and lead to weight loss. Conversely, taking hyperthyroidism medication returns excessive metabolism to normal, which can cause previously lost weight to be regained.
Q.Should I eat a lot of iodine-rich seaweed and kelp?
Excessive intake can actually be harmful. Koreans already consume enough iodine through their regular diet. There is no need to forcefully consume extra seaweed for thyroid health, and high-dose intake in the form of health supplements like kelp extract can ruin thyroid function and requires caution.
Q. When is hospital consultation or visitation absolutely necessary?
When symptoms persist or if you fall into a specific risk group. Tests are needed if you experience unexplained weight changes, extreme fatigue, persistent palpitations, or if the front of your neck appears swollen. Pregnant women and the elderly, in particular, should visit to get a blood test if they notice even small changes, as it can affect fetal or cardiovascular health even without clear symptoms.

The most important criteria when dealing with thyroid diseases are three things.
First, an accurate diagnosis. Rather than relying solely on symptoms, you must accurately determine whether it is thyrotoxicosis or hyperthyroidism through the relationship between TSH and Free T4 levels, and the presence of antibodies.
Second, treatment tailored to the cause. Choose medications that cool the engine for hyperthyroidism, and hormone pills that replenish fuel for hypothyroidism, while adjusting treatment options according to your situation (pregnancy, eye disease, etc.).
Third, consistent follow-up management. Rather than clinging to the concept of a 'complete cure', focusing on 'regulation' to consistently maintain your body's condition through regular check-ups is the path to protecting your health. Current numerical changes are merely signals sent by your body. If you stably manage the numbers through appropriate treatment, you can lower the risk of complications and fully continue a healthy daily life.
Sources
- Korean Endocrine Society/Korean Thyroid Association, Domestic Recommendations for Subclinical Hypothyroidism (2023).
- Korea Disease Control and Prevention Agency National Health Information Portal, Health Information on Hyperthyroidism/Hypothyroidism.
- NICE. Thyroid disease: assessment and management (NG145). 2019.
- Korean Thyroid Association, Clinical Practice Guidelines for Hyperthyroidism (2018).
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



