Not all cases of implant pain or gum swelling require re-surgery. We have clearly outlined when re-surgery is necessary based on the stage of damage and how the implant can be saved through non-surgical and conservative treatments. Check out our treatment guide for implant conditions from early to late stages at a glance.
“My implant hurts, do I need surgery again?”

When an implant feels achy, or when gums swell and bleed, many people immediately think of "re-surgery." However, re-surgery is not required in every case. In fact, if the issue is in the early to middle stages, it can often be fully recovered through non-surgical and conservative treatments.
In this blog, we will clearly explain when re-surgery is truly necessary and which treatments can save your implant without surgery, categorized by the stage of damage.
1. When and how can you save the implant instead of re-surgery?
Implants are precious artificial teeth that should last a long time, just like our natural teeth. However, problems can arise due to neglected maintenance or unexpected issues. Just as you would identify and fix a specific part when a car breaks down, the treatment for an implant varies depending on the extent of the damage.
To start with the most important conclusion: implant re-surgery is primarily necessary only when the implant is severely damaged (late-stage damage). In other words, implants can be saved without re-surgery when problems occur during the early to intermediate stages.
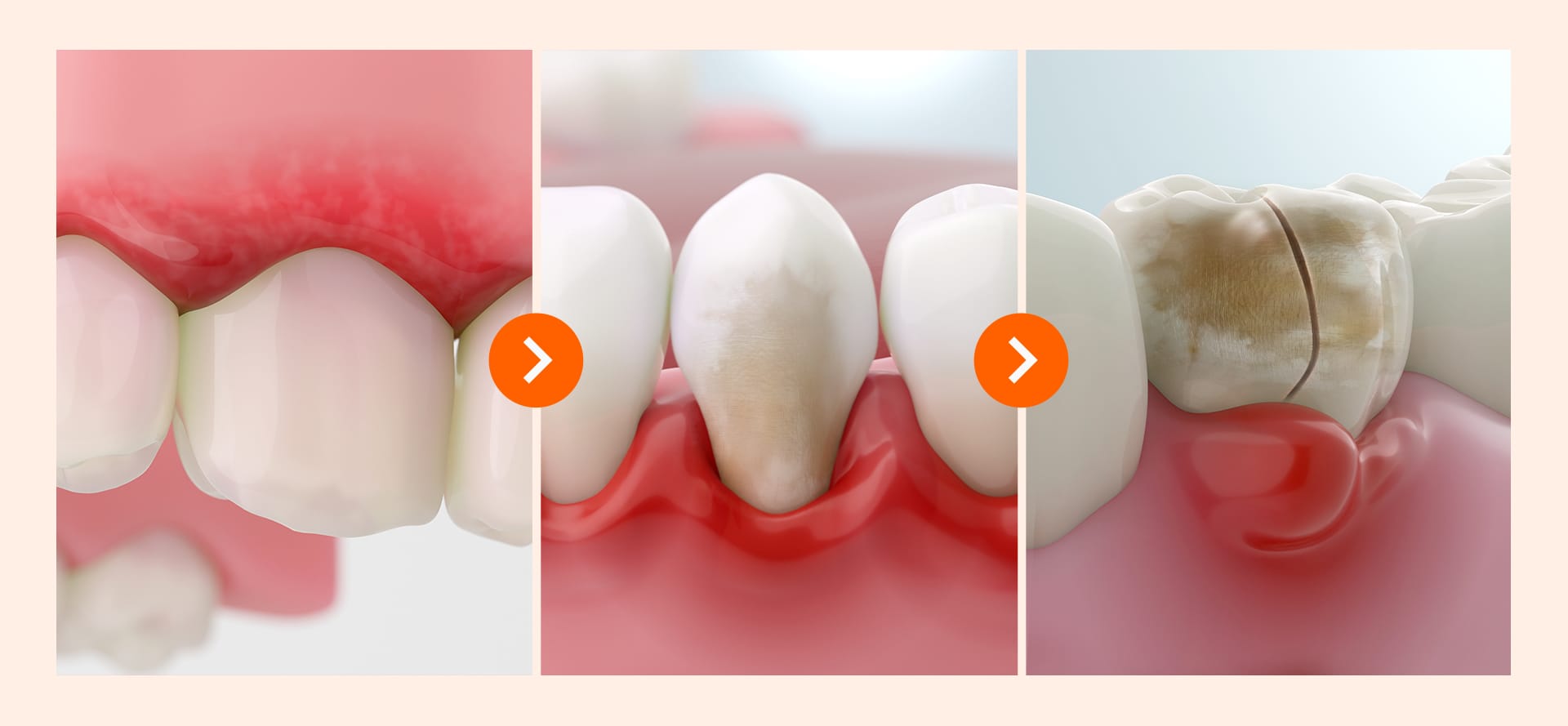
Particularly in the very early stages of inflammation where bone loss is minimal, various non-surgical treatments can lead to a full recovery. Let’s look at the three stages of implant damage: early, middle, and late.
2. Early damage: How does non-surgical treatment work?
Think of this stage as a "yellow light" just turning on for the gums around the implant. The gums might be slightly swollen or bleeding. Much like an early cold, it can be cured quickly with relatively light treatment.
What is the condition?
- Inflammation in the gums around the implant may cause swelling and bleeding.
- The pain is usually not severe, making it easy to overlook.
- At this stage, implant re-surgery is not necessary at all.
How is it treated? Scaling is performed to clean away the harmful bacterial clusters (plaque and tartar) causing peri-implantitis. It is like a deep cleaning for your implant.
| Treatment Name | Description |
| Mechanical Cleaning | Plaque and tartar around the gums are gently removed using specialized implant tools. Since the surface is more delicate than natural teeth, meticulous care is required. |
| Disinfectant Therapy | A mild disinfectant solution or gel is applied to the inflamed area to eliminate bacteria. Repeated treatment over 3-4 weeks is highly effective. |
| Antibiotic Therapy | If inflammation is severe or gum pockets are deep, oral or topical antibiotics are used to alleviate inflammation. |
| Anti-inflammatory Laser | Specialized lasers kill bacteria and promote gum regeneration. This creates a synergistic effect when combined with drug therapy. |
More than 90% of patients treated at this stage fully recover without re-surgery. The treatment period is also relatively short, usually taking about 4 to 6 weeks.
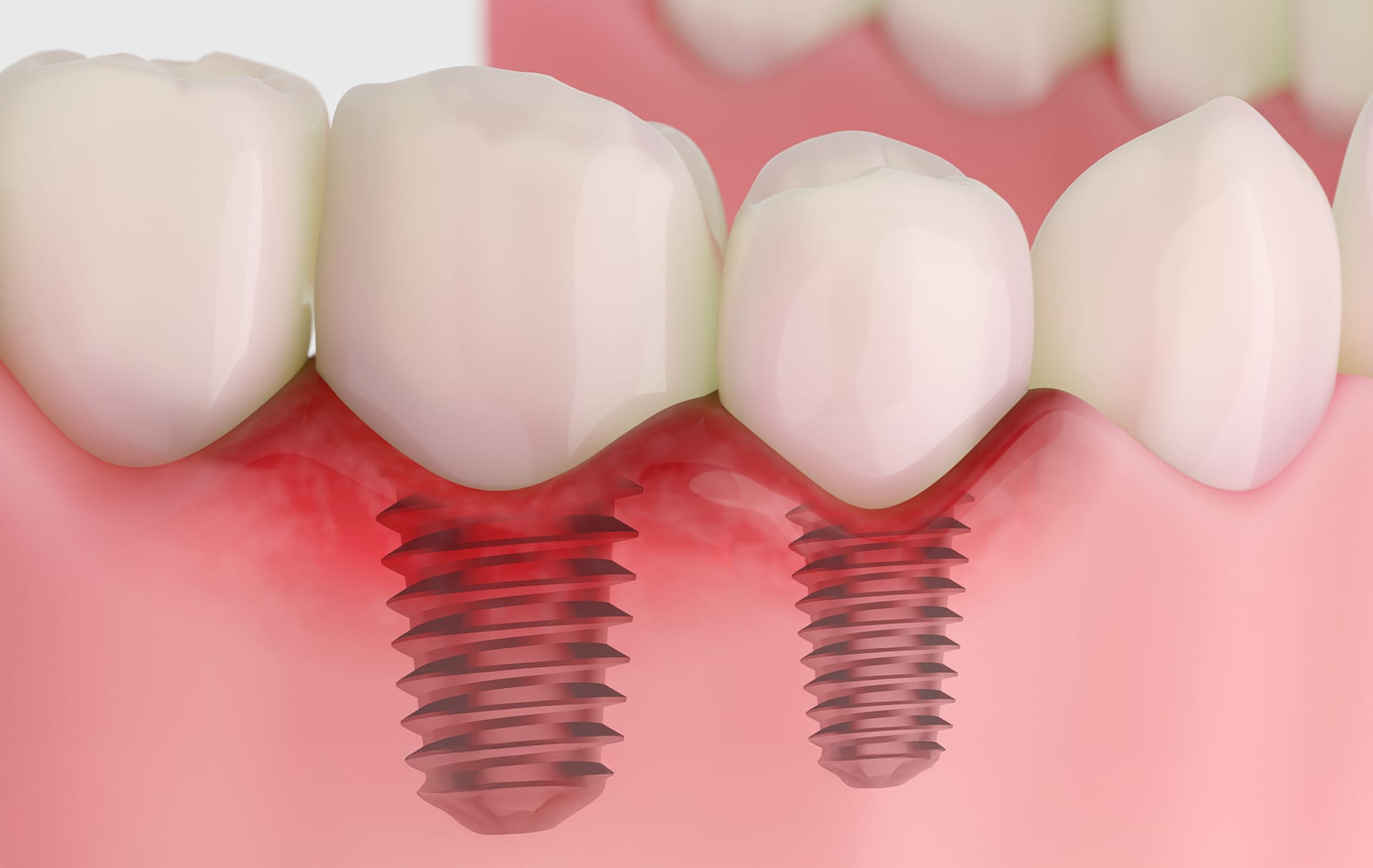
3. Middle-stage damage: Can it be saved with bone regeneration?

Now the "warning light" is flashing. The jawbone is starting to dissolve slightly, and the implant may feel a bit loose. While this stage requires more active treatment than the early stage, it is still possible to treat without re-surgery.
What is the condition?
- Partial dissolution of the jawbone occurs.
- Significant gum swelling and pain may occur.
- Bone loss around the implant is visible on X-rays.
How is it treated? Although the bone surrounding the implant is damaged, the implant itself may still be stable. In this case, regeneration therapy to restore the damaged bone can save the implant without the need for re-surgery.
3-1. Bone Grafting
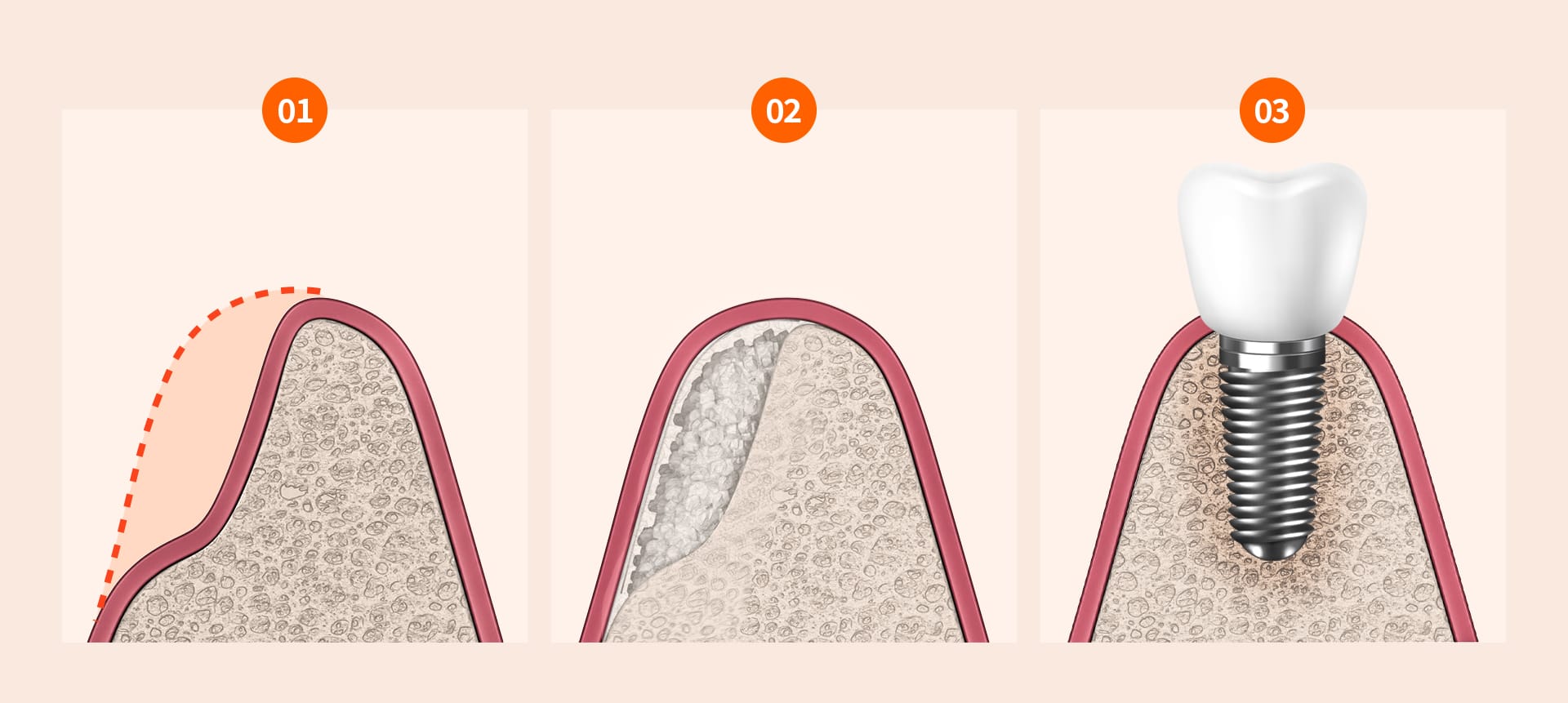
In areas where bone is lacking, materials such as the patient's own bone or synthetic bone are placed to help new bone grow. This helps the implant and bone bond together again.
3-2. Guided Bone Regeneration (GBR)
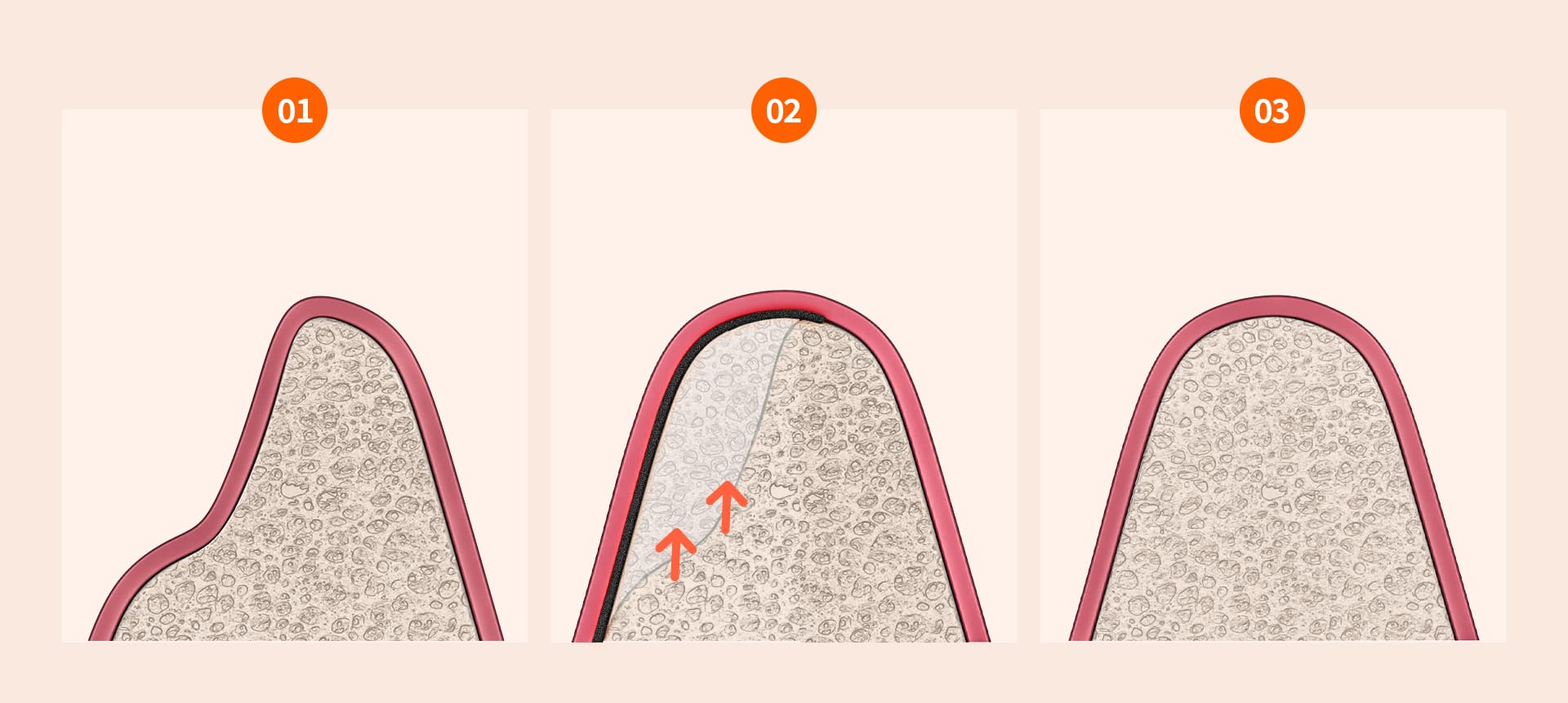
A specialized membrane is placed over the area where bone needs to grow. This prevents gum cells from filling the space first, giving bone cells enough time to grow.
3-3. Regeneration Promoters
- PRP (Platelet-Rich Plasma) Therapy: Platelet-rich plasma is separated from the patient's blood and applied around the implant. It is rich in growth factors that promote bone formation.
- BMP (Bone Morphogenetic Protein): A key growth protein that induces bone cell differentiation and new bone formation, promoting regeneration in areas with poor bone quality.
4. Late-stage damage: Is re-surgery unavoidable?
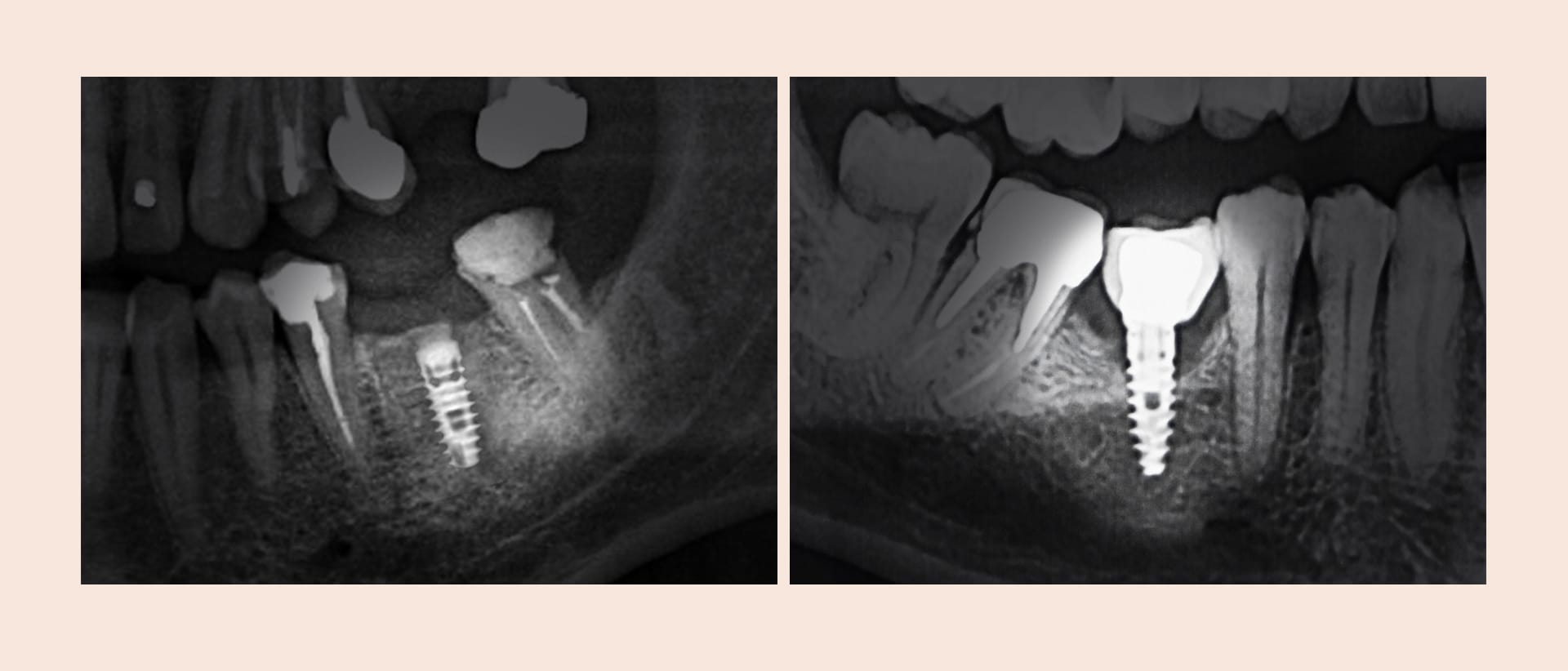
This is when the "danger signal" sounds. This occurs when the root of the implant breaks or the surrounding jawbone has dissolved so severely that the implant itself faces major issues. Unfortunately, at this stage, it is highly likely that re-surgery—placing a new implant—will be necessary.
What is the condition?
- The implant root is significantly exposed, leading to continuous bone loss.
- The surrounding jawbone has dissolved too much for the implant to function.
- Severe pain and inflammation persist.
How is it treated?
| Treatment Stage | Description |
| Precision Diagnosis | Digital equipment like 3D CT is used to analyze the extent of implant damage, bone absorption, and the spread of inflammation. |
| Removal of Damaged Area | Broken implants, screws, inflamed tissue, and necrotic bone are thoroughly removed to create an environment where new tissue can regenerate. |
| Bone Reconstruction | Autogenous or synthetic bone graft materials are applied to the damaged area. Recovery can take several months to a year. |
| New Implant Placement | Once the bone has regenerated and become sufficiently strong, a new implant is placed at the precise position and angle. |
5. The most reliable 'Lifestyle Habit' guide to avoid re-surgery
An implant can be maintained for a long time only when 50% of the patient's effort is combined with 50% professional dental care. It is crucial to catch inflammation before it invades the jawbone. Use the checklist below to monitor your maintenance habits.
| Patient Action Guide | Check Items |
| 1. Regular Check-ups | Visit the dentist every 6 months for X-rays and oral examinations. |
| 2. Professional Cleaning | Have tartar removed using specialized implant tools during regular check-ups. |
| 3. Use Auxiliary Products | Use interdental brushes, floss, and oral irrigators daily to clean gaps. |
| 4. No Smoking/Drinking | Smoking and alcohol exacerbate peri-implantitis and must be avoided. |
| 5. Immediate Visit | If symptoms like swelling, bleeding, or looseness occur, visit the dentist immediately. |
6. Frequently Asked Questions (FAQ)
Q. How can I tell the early symptoms of peri-implantitis and when it's time for re-surgery?
Early peri-implantitis presents with mild symptoms like swollen, red gums or bleeding during brushing. At this stage, there is no bone loss, and it can be resolved with treatment. However, if the implant becomes noticeably loose and the bone has dissolved extensively, re-surgery must be considered.
Q. What can I do daily to avoid implant re-surgery?
Oral hygiene is most important. Besides a regular toothbrush, you must use interdental brushes or floss to clean the tiny gaps between the implant and gums. Additionally, visiting the dentist every 6 months for professional scaling—the foundation of saving an implant—is key to preventing re-surgery.
Q. Can bone graft surgery completely prevent the need for re-surgery?
In middle-stage damage where bone loss is not severe, bone grafting can restore stability. While this is an effective way to avoid re-surgery, if the bone loss is already too extensive or the implant root is damaged, it may eventually lead to a full re-implantation procedure.
Q. My implant area is swollen and painful; what should I do now in case I need re-surgery?
Rather than worrying vaguely, diagnosing the current state of the implant is the priority. Since the pain is likely due to early inflammation, visit a dentist immediately for a 3D CT scan. Early diagnosis is the first and most cost-effective step to saving your implant.

It is easiest to protect an implant when there are "no problems." Most re-surgeries can be avoided by catching inflammation early and restoring support through regeneration in the middle stage. Do not worry alone; visit a dentist to receive an accurate diagnosis and consult on a treatment plan to save your implant.
Sources
- Korean Academy of Periodontology. (2020). Guidelines for the Diagnosis and Treatment of Peri-implantitis.
- Ministry of Health and Welfare. (2022). Oral Health Survey and Implant Management Guidelines.
- Jepsen, S., et al. (2015). Primary prevention of peri-implantitis: managing gingivitis in implant patients. Journal of Clinical Periodontology, 42(S16), S1-S6.
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads