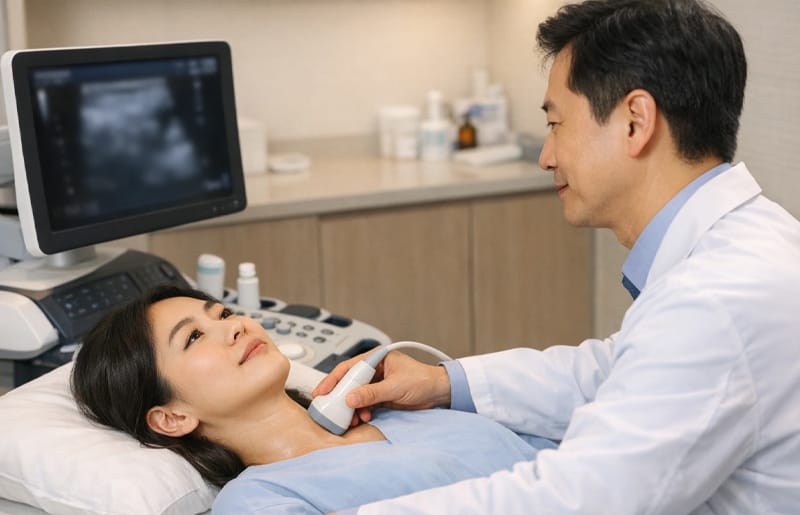
If your health checkup shows TSH (Thyroid Stimulating Hormone) levels outside the reference range, does it mean you need immediate treatment? We explain the medical principles of TSH interpretation, the criteria for deciding on medication based on clinical evidence, and the conditions under which a retest is necessary.

"There is a red arrow on my report; could it be a serious illness?"
Many people urgently open a search engine after receiving their checkup results in a state of panic. Especially for office workers or homemakers in their 30s and 40s who often feel fatigued, discovering an abnormal value can be frightening.
However, unlike what many fear, being slightly outside the reference range on a checkup report does not mean everyone must immediately begin taking hormone medication. Understanding the accurate meaning hidden behind the numbers can help reduce unnecessary anxiety.
1. Does 'High TSH' Immediately Mean 'Thyroid Failure'?
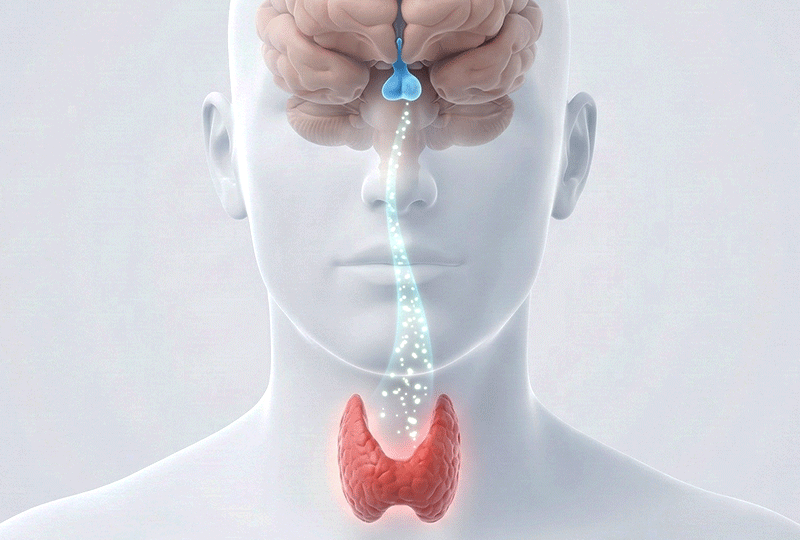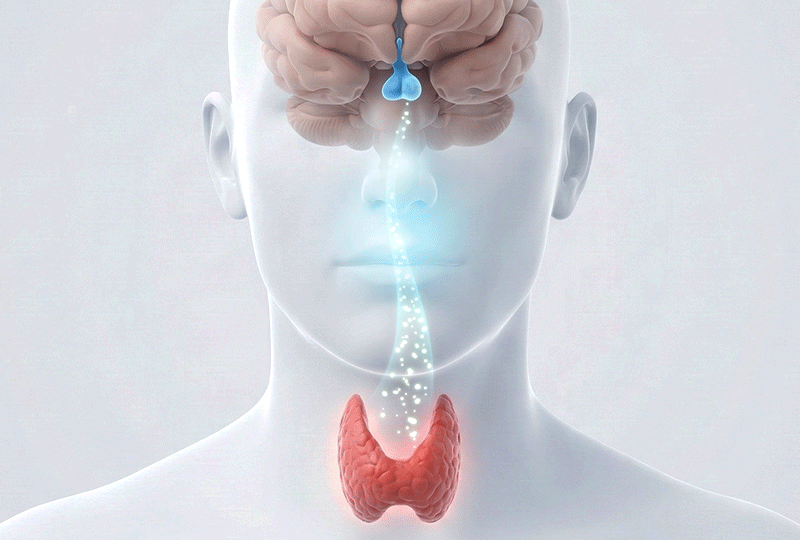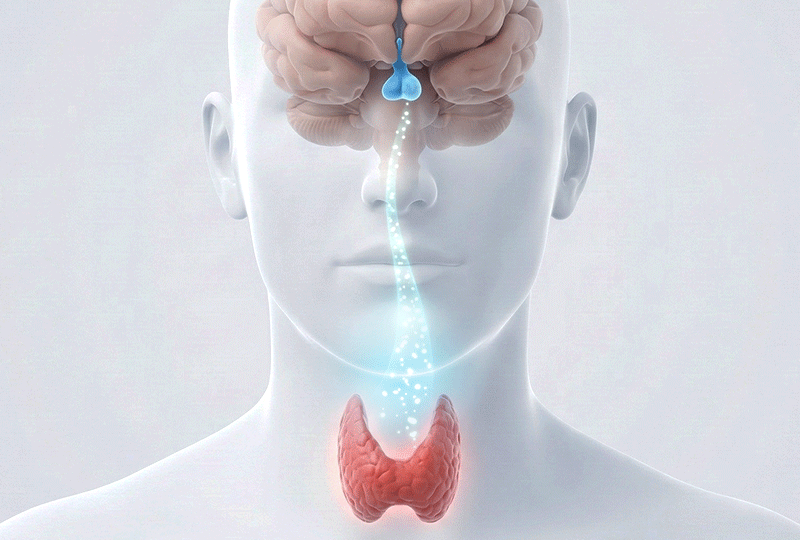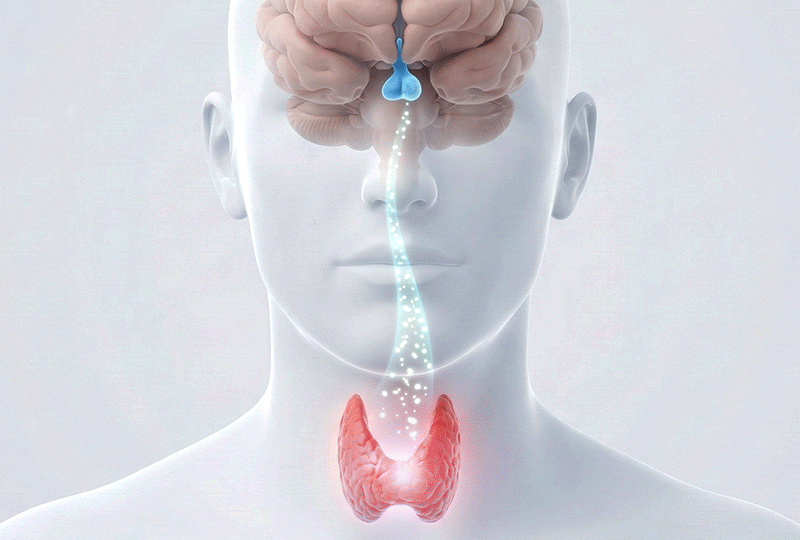
Our body's thyroid hormone regulation system is very similar to the relationship between a 'boiler (thyroid)' and a 'thermostat (pituitary gland).'
In this analogy, TSH is the signal from the brain (thermostat) saying, "The room is cold, so turn up the heat," and Free T4 is the actual "temperature (hormone)" inside the room.
What if the temperature in the room is warm enough (Normal Free T4), but the thermostat keeps sending a signal (Elevated TSH) to "burn more fuel"? This could mean the boiler is not completely broken, but its efficiency has dropped slightly, so it only maintains the temperature if a stronger signal is sent.
Medically, this state is called 'Subclinical (Inapparent) Hypothyroidism.' Literally, there are almost no visible symptoms, or they are very subtle, and it is a state where only the brain's signal (TSH) is elevated on a blood test.
In fact, many people who show abnormal TSH levels in health checkups fall into this stage, which is clearly distinguished from 'Overt Hypothyroidism,' which requires immediate treatment.
There is no need to conclude that the "thyroid is broken" just because the TSH level is high. It is closer to an 'early warning' that our body is struggling to maintain normal hormone concentrations. The important thing is the process of distinguishing whether this warning is a temporary malfunction or a situation where a boiler component has actually failed and requires repair.
To confirm this, a diagnosis is usually not made with a single test; instead, changes in the values are observed through a retest after a certain period.
2. If the Result is Outside the 'Normal Range,' Is Medication Mandatory?
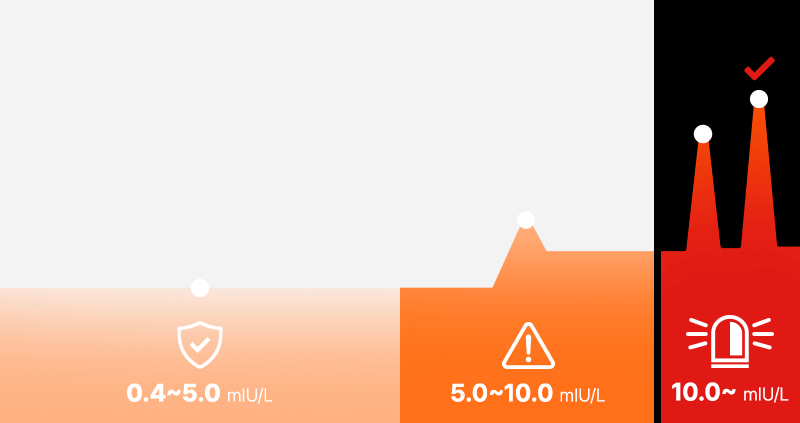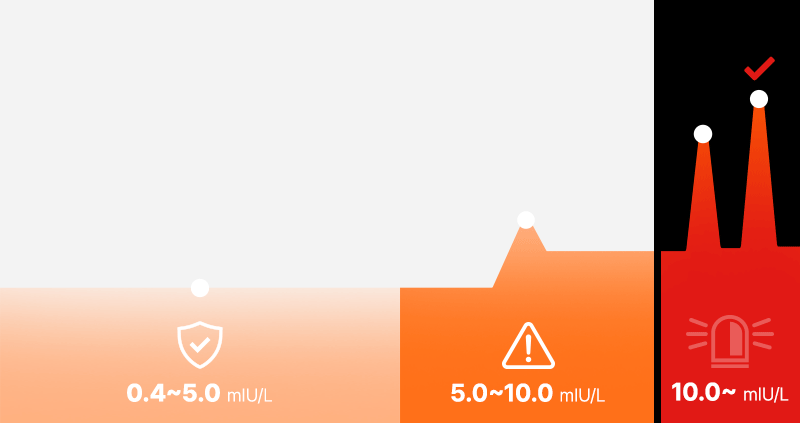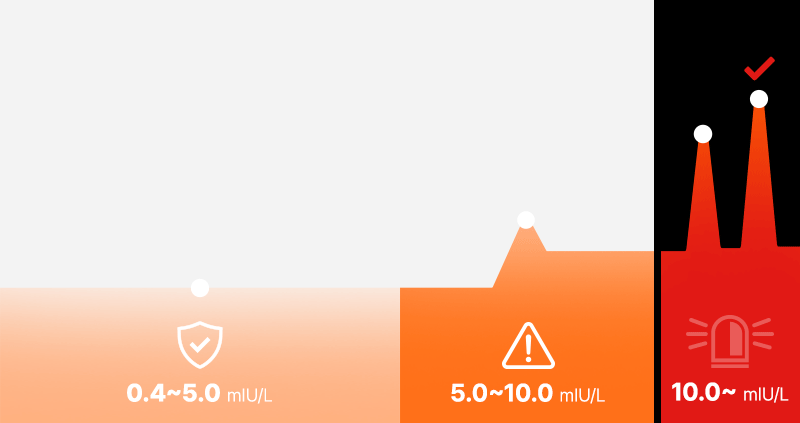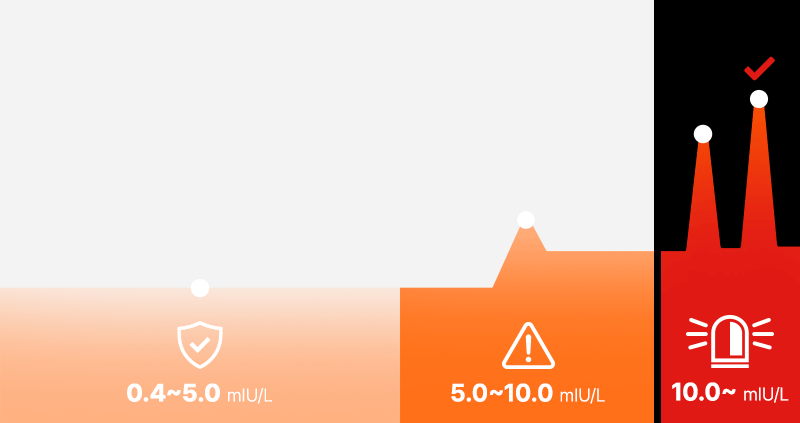
Just because a result is outside the 'Normal Reference Range (usually 0.4–4.0 or 5.0 mIU/L)' written on the report does not mean everyone becomes a candidate for treatment.
Reference values can vary slightly depending on the reagents, equipment of the testing institution, and the statistical distribution of the reference population. Most importantly, the 'laboratory reference value' and the 'criteria used by doctors to decide treatment (Cut-off)' are different. Just as clothing sizes vary slightly by brand, the reference value is merely a statistical range and not an absolute boundary between health and disease.
Major domestic and international guidelines (NICE, ATA, etc.) generally strongly consider drug treatment when TSH is repeatedly confirmed to be 10 mIU/L or higher.
Conversely, if TSH is below 10 (especially between 4 and 10) and Free T4 is normal, follow-up observation is often recommended rather than hastily using medication. For your understanding, we have summarized the general response guide by numerical range:
| TSH Level (mIU/L) | Free T4 Status | General Recommended Action |
| 0.4 – 4.0 | Normal | Normal: No special action required (Maintain regular checkups) |
| 4.0 – 10.0 | Normal | Follow-up: Retest recommended in 2–3 months (Possibility of subclinical state) |
| 10.0 or higher | Normal/Low | Consider treatment: Decide on medication through specialist consultation |
| Regardless of value | Low | Treatment required: High possibility of overt hypothyroidism |
Domestic experts, such as the Korean Thyroid Association (KTA), may view the TSH range between 6.8 and 10 as a 'warning light' zone, considering the characteristics of Koreans. In this zone, if there are no special risk factors, it may be safer to watch whether the levels stabilize on their own through a retest rather than immediate medication.
One must comprehensively judge whether 'my body is in a situation that requires medication' rather than mechanically taking medicine just because the number on the report is red.
3. Why the 3040 Generation Should Check 'This' Before 'Fatigue'

For patients in their 30s and 40s, especially women, the interpretation criteria can change completely depending on whether they have a 'plan for pregnancy or infertility treatment.'
Since the mother's thyroid hormone is absolutely necessary in the early stages of fetal brain development, much stricter criteria are sometimes applied to those preparing for pregnancy or in the early stages of pregnancy compared to general adults.
To use the boiler analogy again, the temperature of the 'room where the baby grows' must be regulated much more sensitively, so the allowable range of the thermostat (TSH) is kept narrow.
If TSH is measured at around 5 to 6, a person would usually hear "let's watch it" in a general situation, but if they are planning a pregnancy, the medical staff may consider intervention to lower the value. The target value applied at this time can vary depending on the gestational age and hospital guidelines, so consultation with the attending physician is necessary.
On the other hand, simply thinking, "I'm so tired lately; is it because of my thyroid?" and self-diagnosing based only on symptoms requires caution. According to large-scale studies such as the TRUST clinical trial published in NEJM (2017), many patients with a slight elevation in values did not see clear improvement in symptoms like fatigue even after being administered medication.
The criterion for judgment for the 3040 generation should not be 'how tired I am,' but rather 'whether there are pregnancy-related issues' and 'whether autoimmune antibodies are present.' This is because symptoms are subjective, but risk factors confirmed by blood tests are objective.
4. When and What Should Be Checked for a 'Final Diagnosis'?

The TSH level is highly volatile depending on the condition on the day of the checkup, medications being taken, and the time of the test (morning/afternoon).
It is not rational to decide whether to take medication for a lifetime based on a single test. Medical staff usually check whether the value has spiked temporarily or is in a persistently high state (persistence) through a retest after 2 to 3 months. It is a process of waiting to see if the boiler has malfunctioned briefly or is in a state of failure requiring parts replacement.
The most important additional item during a retest is the 'Anti-TPO Antibody (Thyroid Peroxidase Antibody)' test. This antibody is an indicator showing whether our body's immune cells are mistakenly attacking the thyroid as an enemy.
If TSH is slightly high and this antibody is also positive, the probability that thyroid function will permanently decline in the future increases, so more active management is required. Conversely, if the antibody is negative and the shape on the ultrasound is clean, one can wait with more ease, keeping in mind the possibility of a temporary numerical fluctuation.
[Retest Checklist]
- Confirm Free T4: Did you reconfirm the Free T4 level along with TSH?
- Add Antibody Test: Did you include the Anti-TPO antibody test in your request?
- Share Pregnancy Plans: Did you inform the medical staff that you are preparing for pregnancy?
- Review Medications: Are there any iodine supplements or herbal medicines you have taken recently?
If you approach the retest by checking the items above, it will help reduce unnecessary worry and assist in receiving a more accurate diagnosis.
5. Can the Korean Table, 'Seaweed Soup,' Change the Levels?

"I heard it's good for the thyroid, so I ate seaweed soup every day." This is a story frequently heard in the consultation room. However, Korea belongs to a group of countries with very high iodine intake globally.
While iodine is an important nutrient that serves as the raw material for thyroid hormones, if consumed excessively, our body may activate defense mechanisms (such as the Wolff-Chaikoff effect) that temporarily inhibit the production of thyroid hormones.
In the boiler analogy, this is similar to an overload state where too much fuel (iodine) is poured in, so combustion does not occur properly. In this process, the brain senses that hormone production has decreased and increases TSH secretion; consequently, excessive iodine intake can be a cause of a temporary rise in TSH levels.
In fact, even when TSH appears high despite no special underlying disease, it has been reported that numerical fluctuations tend to decrease when intake patterns are adjusted and follow-up tests are conducted.
If TSH appeared high in your checkup results, it is better to first check your usual eating habits rather than blindly looking for foods said to be good for the thyroid. While side dishes like dried seaweed or seaweed soup consumed in a general meal are not a major problem, stopping the intake of highly concentrated products in the form of 'kelp pills' or 'concentrated extracts' before taking a retest is a way to reduce confusion in numerical interpretation.
Considering the special environment of Korean food culture is a very important criterion for judging numerical interpretation.
6.Frequently Asked Questions(FAQ)
Q. My TSH is a bit high, around 5 to 7; should I start medication?
If there are no special symptoms and no pregnancy plans, a retest is usually recommended after 2 to 3 months rather than starting medication immediately. As in the boiler analogy mentioned earlier, if the room temperature (Free T4) is still normal, the boiler might not be in a state of complete failure. However, the decision is made considering the presence of antibodies according to the judgment of the medical staff.
Q. Why is only my TSH high while Free T4 is normal?
This is called 'subclinical hypothyroidism.' It is a state where the brain senses that thyroid function is about to drop slightly and sends a strong signal (TSH) in advance to maintain function. It can be seen as a result of a compensatory action to maintain our body's homeostasis.
Q. When is the most accurate time for a retest?
Usually, 2 to 3 months after the first test date is recommended. This is because thyroid hormone levels tend to change gradually rather than abruptly overnight, and sufficient time is needed for temporary factors (stress, medication, viral infection, etc.) to be resolved.
Q. Do I absolutely need to get an Anti-TPO antibody test?
It is recommended to identify the cause in cases where TSH levels are repeatedly high or if there is a family history. If this antibody is confirmed positive, it means there is a high possibility of progressing to hypothyroidism in the future, so it serves as an important indicator for deciding whether to perform simple follow-up observation or start treatment.

The core of thyroid value interpretation is not to be happy or sad about a single number. First, you can know the true state of your body only by checking the balance with Free T4 rather than the TSH value alone. Second, if you are in your 30s or 40s and of childbearing age, you must remember that more careful management may be required than the general standards. Third, the process of clearly distinguishing whether this is a temporary episode or a disease requiring treatment through retesting and antibody confirmation is essential. The red numbers on the checkup report are precious signals our body sends, but they do not mean a confirmed diagnosis of a disease in themselves. Based on the criteria summarized today, we hope you prepare for the next test calmly rather than being anxious, and establish a rational plan together with medical staff.
Sources
- Korean Thyroid Association (KTA). (2023). Management Guideline for Subclinical Hypothyroidism.
- Moon et al., Reference range of TSH in Korean adults, Korean J Intern Med, 2018.
- NICE Guideline [NG145], Thyroid disease: assessment and management, 2019.
- Stott DJ, et al., Thyroid Hormone Therapy for Older Adults with Subclinical Hypothyroidism, N Engl J Med, 2017.
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.