This guide covers everything patients in their 40s to 60s need to know about peri-implantitis—from its underlying causes and symptoms to treatment options and lifelong maintenance strategies.
"I thought implants would last a lifetime without issues. Why does it hurt again?"

Mr. A, a patient in his early 60s, received dental implants seven years ago. Despite his diligent brushing habits, he recently visited the clinic due to gum swelling and pain. The diagnosis was peri-implantitis. He was shocked.
In reality, peri-implantitis is not caused by poor hygiene alone. It is often a complex combination of hidden structural flaws, systemic diseases, and lifestyle habits. This article will walk you through the causes, symptoms, and essential management of this condition.
1. Is Peri-implantitis Just Due to Poor Brushing?
While the direct cause is bacterial plaque, brushing alone cannot prevent all risks. Unlike natural teeth, implants do not provide early warning signals like mobility until bone loss has progressed by more than 10%. This makes regular check-ups and early detection vital.
2. Major Causes of Peri-implantitis

Bacterial infection is the immediate trigger, but structural defects that create an environment for bacteria to thrive are often the root cause.
① Insufficient Placement Depth: Implants should ideally be placed 2–3mm below the bone ridge. If placed too shallowly, the protective gum layer thins, increasing the risk of bone loss and screw exposure.

② Lack of Inter-implant Distance: When placing multiple implants, a distance of at least 3mm is required. Narrow gaps can block blood flow, leading to bone necrosis and inflammation.
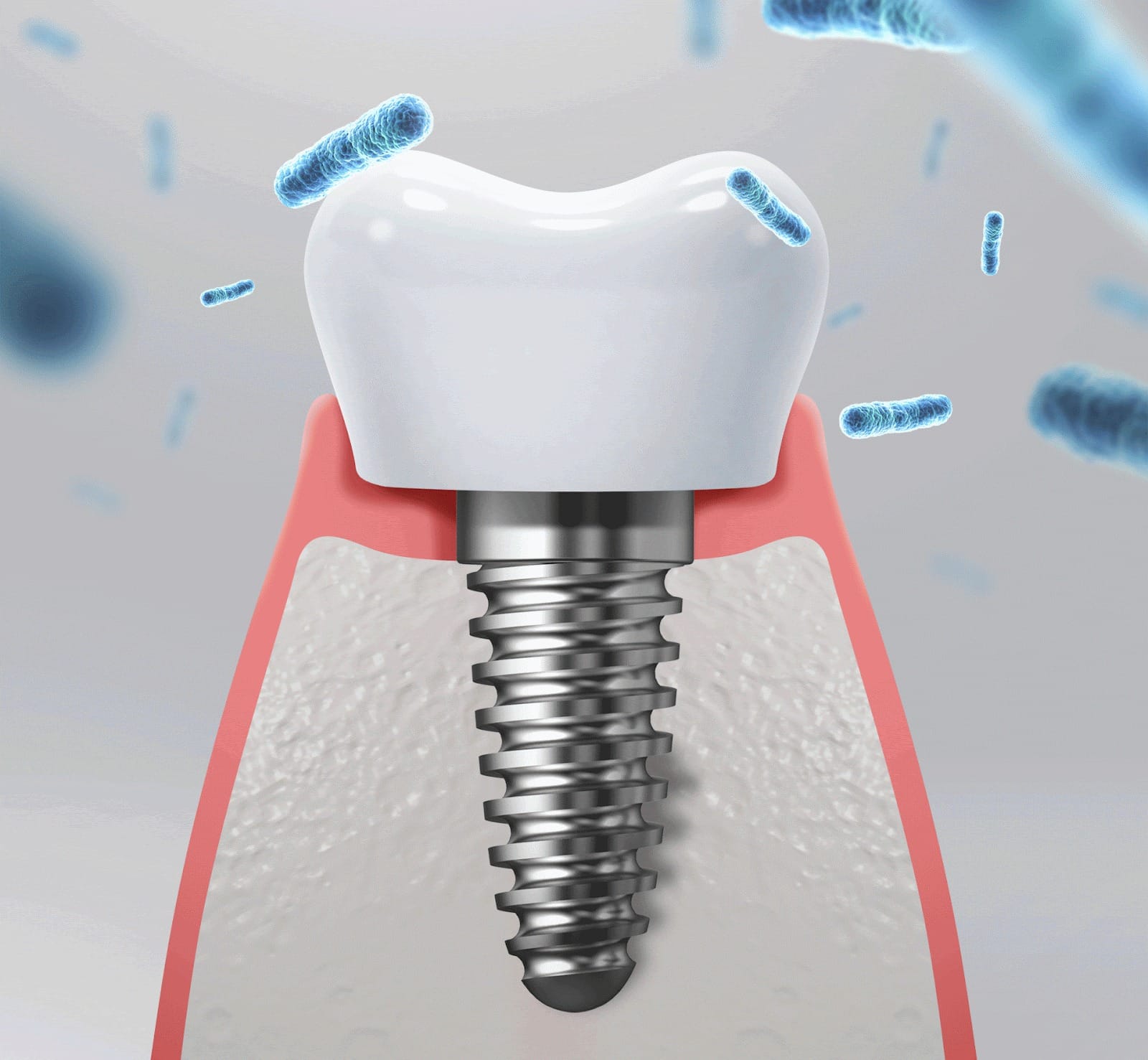
③ Residual Cement: Excess cement used to bond the prosthetic is difficult to detect even via X-ray. It becomes a breeding ground for plaque, causing chronic inflammation and bone resorption.

④ Improper Prosthetic Shape/Angle: Overly convex crowns create "undercuts" where toothbrushes cannot reach. An emergence angle greater than 30° makes bacterial access easier.

⑤ Microgaps at the Abutment Connection: A microscopic gap (20–200㎛) between the implant and abutment can allow bacterial infiltration. "Platform switching" designs are helpful in preventing recurrence.
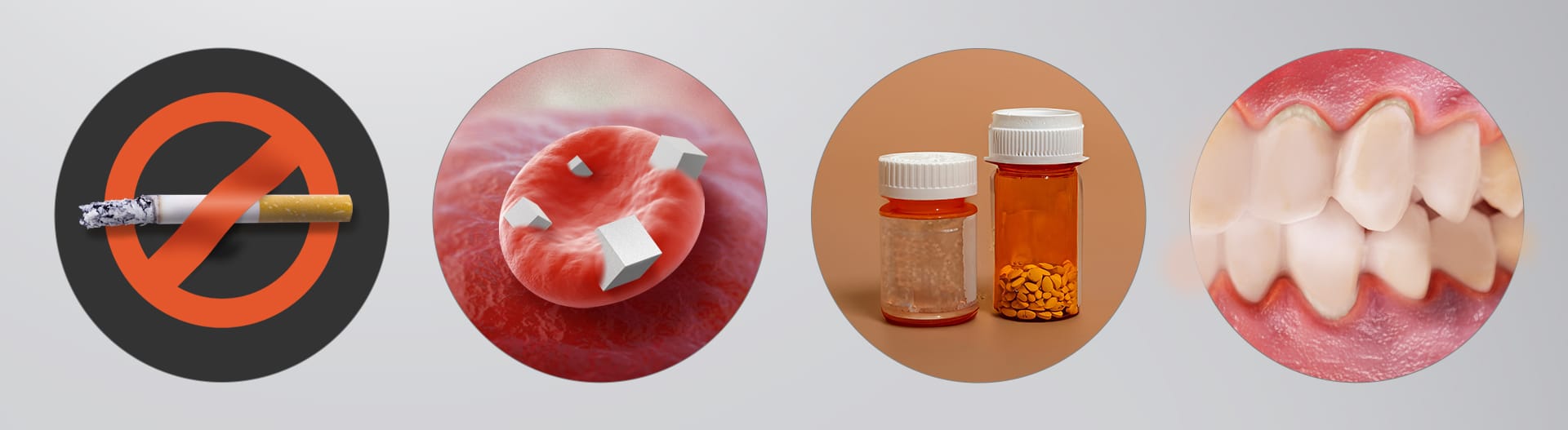
⑥ Systemic Health & Habits:
- Smoking: Reduces blood flow and immunity, increasing the incidence rate by 2–3 times.
- Diabetes: Delays wound healing and increases vulnerability to infection.
- Medications: Certain drugs (e.g., for osteoporosis) may increase the risk of jawbone necrosis.
- Bruxism/Excessive Force: Implants lack a shock-absorbing ligament, so excessive force leads to mechanical bone loss.
3. Symptoms of Peri-implantitis
- Gum swelling and redness
- Persistent bleeding
- Halitosis (bad breath)
- Pain while chewing
- Implant mobility (looseness)
4. Treatment Methods
Treatment depends on the stage of progression.
| Stage | Symptoms | Treatment Method |
|---|---|---|
| Early | Gum swelling and bleeding | Scaling, laser disinfection, medication |
| Moderate | Partial bone loss | Bone grafting, regenerative surgery |
| Late | Mobility and severe pain | Removal and re-implantation (Revision) |
5. Lifelong Management Guidelines
An implant is not the "end of treatment" but the "beginning of management."
- Regular Check-ups: Every 6 to 12 months.
- Precision Diagnosis: Periodic CT scans if necessary.
- Lifestyle Management: Quitting smoking, controlling blood sugar, and preventing teeth grinding.
- Specialist Consultation: Choose a clinic with extensive experience in managing complications and revision surgeries.
6. Frequently Asked Questions (FAQ)
Q. Do I have to remove the implant if there is inflammation?
No. If bone loss is not severe, the implant can be saved through inflammation removal and regenerative therapy.
Q. What should I do if the implant feels shaky?
This could indicate osseointegration failure or severe inflammation. Seek an immediate clinical examination.
Q. Can diabetic patients maintain implants long-term?
Yes, as long as blood sugar is well-controlled. However, strict adherence to regular check-ups is mandatory.
Q. Does peri-implantitis recur easily?
It can recur if the underlying cause is not corrected. Consistent lifestyle management and regular professional cleaning are essential.

An implant is more than just a device; it is a vital partner for your quality of life. When detected and managed early, it can be used comfortably for a long time. Do not worry alone—checking your current status is the most certain first step to protecting your implant. Treatment results, duration, and experiences may vary depending on the individual's condition. Decisions must be made through a consultation with a qualified dentist.
Sources
- Berglundh, T., et al. (2018). Peri-implant diseases and conditions: Consensus report of workgroup 4. Journal of Periodontology.
- Chrcanovic, B. R., et al. (2014). Risk factors for peri-implantitis. Journal of Dental Research.
- Schou, S., et al. (2003). Prognosis of implant treatment in patients with peri-implantitis. Clinical Oral Implants Research.
- Renvert, S., & Polyzois, I. (2015). Treatment modalities for peri-implant mucositis and peri-implantitis. Periodontology 2000.
- Rinke, S., et al. (2011). The frequency of peri-implant diseases: A systematic review. Int J Oral Maxillofac Implants.
※ The copyright for all content on this blog belongs to Medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



