Determining implant candidacy requires a comprehensive assessment of bone and gum health, the management of systemic diseases, and the availability of an environment suitable for long-term maintenance. Review these implant candidacy factors to establish a realistic treatment plan with your medical team.
"Am I too old for implants?"
"Is it okay since I'm taking diabetes medication?"
These are the most common questions heard in the consultation room. Deciding on a treatment that requires significant time and cost often brings anxiety about whether the procedure is possible or if problems will arise later. For those living abroad who must travel long distances, the concern is even greater—fearing they might hear "treatment is difficult as planned" only after arriving in Korea.
To alleviate these concerns, here are the criteria for determining implant eligibility. The planning and process of an implant are similar to 'building a sturdy house.' You must check if the ground (bone and gums) is solid, if the weather (systemic diseases and medications) will interfere with construction, and if the finished house can be maintained regularly. By checking your readiness before your consultation, you can find the safest method tailored to your needs.
1. Is an implant impossible if bone is lacking or gums are weak?
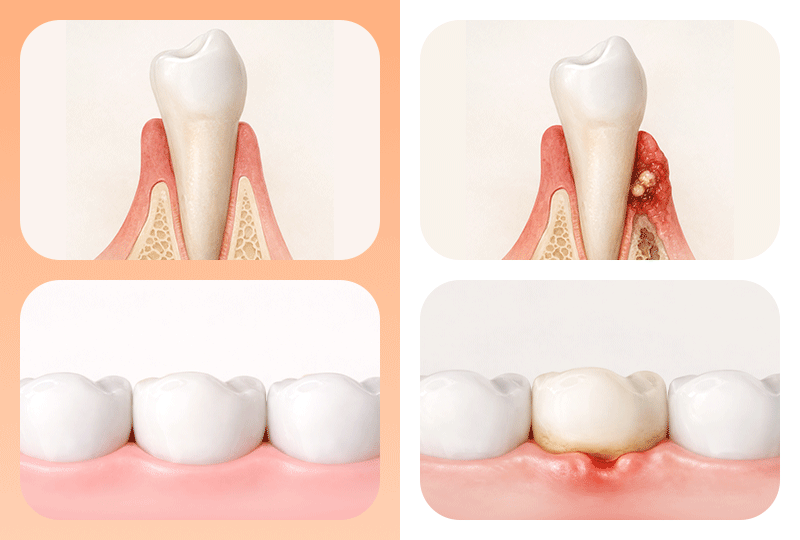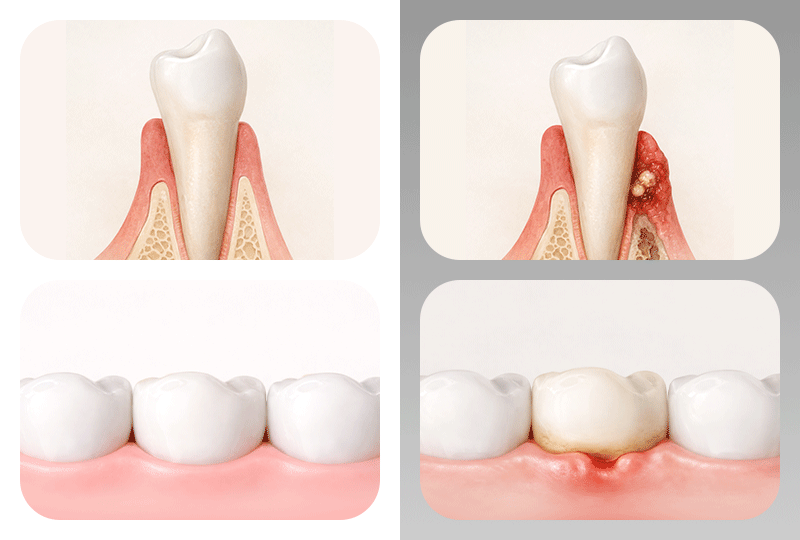
The first step in an implant consultation is checking the 'foundation' that will firmly hold the artificial tooth root—namely, the health of the jawbone and gums. Many believe that "if there is not enough bone, an implant is absolutely impossible," but it is more accurate to view this as a 'branching point' where additional treatment steps are required.
1) Depth and Width of the Ground (Bone Condition Scenarios)
Just as a tree needs soil for its roots to spread, an implant screw needs space to be fully submerged in the bone. Two cases typically emerge based on the condition:
- Case A (Sufficient Bone Volume): If the bone condition is good, the implant can be placed immediately after extraction, or the prosthetic process can begin relatively quickly, making the schedule efficient.
- Case B (Insufficient Bone Volume): If the bone has dissolved due to periodontitis or if a long time has passed since extraction, foundational work like 'bone grafting' or a 'sinus lift' (lifting the empty space in the upper jaw) is necessary. This does not mean the procedure is impossible; rather, it is a branching point where a healing period for the bone to harden is added to the overall timeline.
2) Weeding and Leveling the Ground (Inflammation Management)
Even the best land is hard to build on if it is overgrown with weeds. The 'environment (inflammation)' is just as important as the 'material (bone).' Even with strong bone, severe gum inflammation (periodontitis) increases the risk of peri-implantitis.
- If you frequently experience bleeding or swelling in your gums, steps like scaling or periodontal treatment must be performed to subside inflammation before implant placement.
- For expats, as intervals between visits can be long, it is essential to check for inflammatory responses (bleeding, swelling) even if there is no pain to ensure safe results.
2. What should I prepare if taking diabetes or blood pressure medication?
Even with a solid foundation, construction is difficult during a storm. A patient's systemic health and medications are like the 'weather' that dictates the safety and healing of the surgery. The key criterion is not "it's impossible because of a chronic illness," but rather the status of 'control' and 'medical coordination.'
1) Diabetes: Control Status is More Important than the Figure
Diabetes itself is not a signal that an implant is impossible. What matters is 'how stably the blood sugar is being controlled.'
- Controlled Cases: If HbA1c levels are stable and there are no complications, the procedure can often proceed as planned with extra attention to infection management.
- Difficult to Control Cases: Persistent high blood sugar slows wound healing and increases infection risk. In such cases, it is safer to consult with a primary care physician to stabilize blood sugar first or adjust the timing of the procedure. Bringing recent blood test results to your consultation helps the medical team create a plan that minimizes risk.
2) Bone Metabolism Medications and Medical Coordination
If you are taking osteoporosis medications (bone resorption inhibitors, etc.) or blood thinners, you must inform the medical team. Some osteoporosis medications have been reported to rarely affect jawbone healing (related to MRONJ), requiring caution.
Arbitrarily stopping medication can be more dangerous. Therefore, a coordination process between the dentist and the prescribing physician must occur to adjust the 'continuation of medication' or 'drug holiday' period. If you cannot remember the names of your medications, taking a photo of your prescription or medication list is the most reliable way.
3. As an expat, how should I schedule my Korea visit?

For those living abroad, an implant is not just a treatment but a major project involving flight schedules and stay durations. Rather than asking "How many times do I need to visit?", it is more realistic to plan across three pillars: Visits, Stay, and Aftercare.
1) Visits: Considering 'Branching Points' based on Condition
- Basic stages include diagnosis, surgery, suture removal, impressions, and final placement.
- However, as mentioned, if bone grafting or gum treatment is added, or if inflammation is discovered, the number of visits may increase. Therefore, instead of aiming for the minimum number of visits, it is safer to keep a "flexible schedule for additional treatments."
2) Stay: Time for Healing and Stability
- Long-distance flights immediately after surgery can be burdensome. Especially if a sinus lift was performed in the upper jaw, pressure changes during flight can have an impact, so you may need to avoid flying for a certain period according to the medical team's instructions.
- Recovery speeds vary significantly by individual, so it is best to finalize your return schedule after consulting with the medical team based on your post-operative progress.
3) Aftercare: Preparing a Local Connection System
- An implant is not the "end of surgery" but the "beginning of management." Regular checks for screw loosening or gum inflammation are necessary for long-term use.
- Identify a local dental clinic where you live that can provide basic scaling and checkups.
- Request your surgical records, implant specifications, and X-ray images in English from your dentist in Korea. This will allow for much faster and more accurate responses if a problem arises at your local clinic.

An implant is not merely filling a vacant space; it is a precious treatment that becomes a part of your body and restores the joy of eating. Based on today's discussion, please consider the following three points before your consultation:
First, understand that additional steps like bone grafting may extend the schedule depending on your bone and gum condition.
Second, if you have chronic illnesses or take medications, do not hide them; prepare your records to find the safest timing with your medical team.
Third, if you are an expat, include finding a local clinic and securing your Korean dental records in your plan for post-operative care.
Your oral health is not a binary of 'possible or impossible,' but a journey to find the safest way to reduce risk and achieve optimal function. With thorough preparation and clear communication with your medical team, you can achieve a strong and healthy second set of teeth.
Sources
- Korean Academy of Periodontology, National Consensus on Peri-implant Diseases, 2025.
- Domestic Multidisciplinary Recommendations, Clinical Practice Guidelines for MRONJ, 2025.
- Comprehensive Systematic Reviews (Based on SSOT Summaries).
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads



