Laminate veneers are a effective way to improve the appearance of teeth, but they are an irreversible procedure that requires careful consideration. Understanding the causes of common issues—such as chipping, debonding, and marginal discoloration—is essential for long-term success. While no-prep options are popular, they are only suitable for specific cases to avoid gum inflammation and unnatural results. Success depends on a combination of precise medical bonding, enamel preservation, and consistent patient lifestyle habits.
"When I look at laminate reviews, some people are satisfied, but I also see stories about them breaking or falling off, which makes me nervous."

It is perfectly natural to feel this way. Laminate treatment involves attaching thin porcelain restorations to the front of the teeth to improve their shape and color. While the benefits are clear, the conditions that lead to failure or side effects are also well-documented.
Furthermore, laminates are an irreversible procedure; once you start, it is difficult to return to the original state of your teeth. Rushing into a decision without addressing your concerns can increase the risk of dissatisfaction.
This guide covers why laminates chip or fall off, why color issues occur, the limitations of no-prep laminates, and the essential maintenance steps to preserve your smile.
1. Why Do Laminates Chip or Crack?
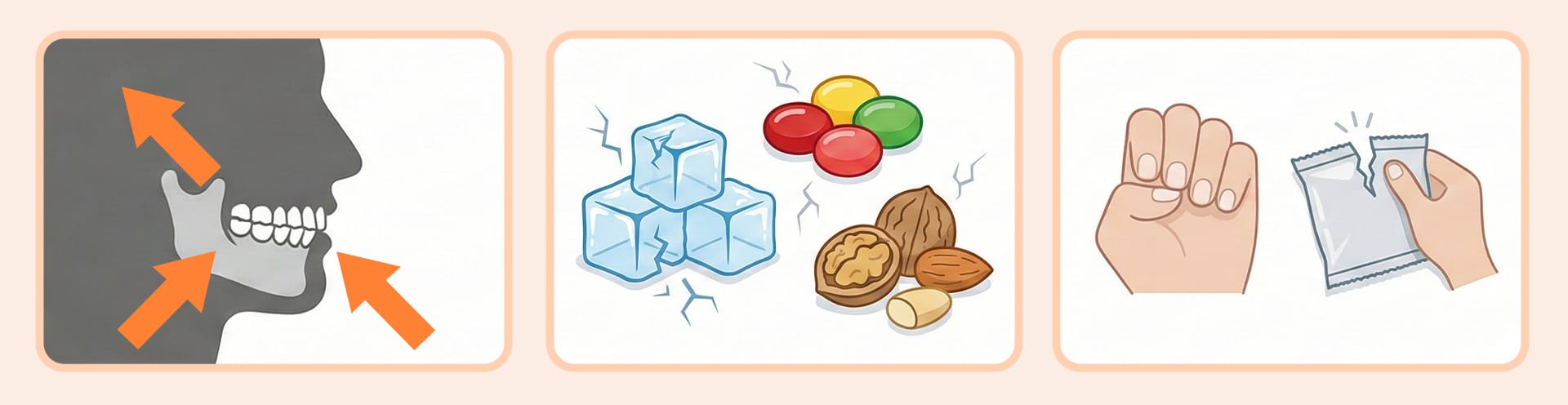
Fracture is one of the most frequently mentioned issues in laminate failure. Because laminates are thin porcelain restorations, they are more sensitive to impact than thicker restorations like crowns.
Factors that increase the risk of chipping often stem from daily habits and occlusal (bite) issues:
- Occlusion-related: Habits such as teeth grinding (bruxism) or clenching significantly increase pressure on the teeth during sleep.
- Food-related: Frequently biting into ice, hard candy, or nuts with the front teeth can cause damage.
- Lifestyle-related: Using front teeth as tools—such as tearing open packaging or biting fingernails—repetitively stresses the restoration.
The first step in preventing chips is to avoid biting hard objects with your front teeth. It is also helpful to undergo an occlusal analysis before the procedure to identify habit-related risks. If necessary, wearing a night guard after treatment can help distribute forces more evenly. Remember, chipping is not just a material issue; it is a result of the direction and frequency of the forces applied to it.
2. What Causes Laminates to Fall Off?
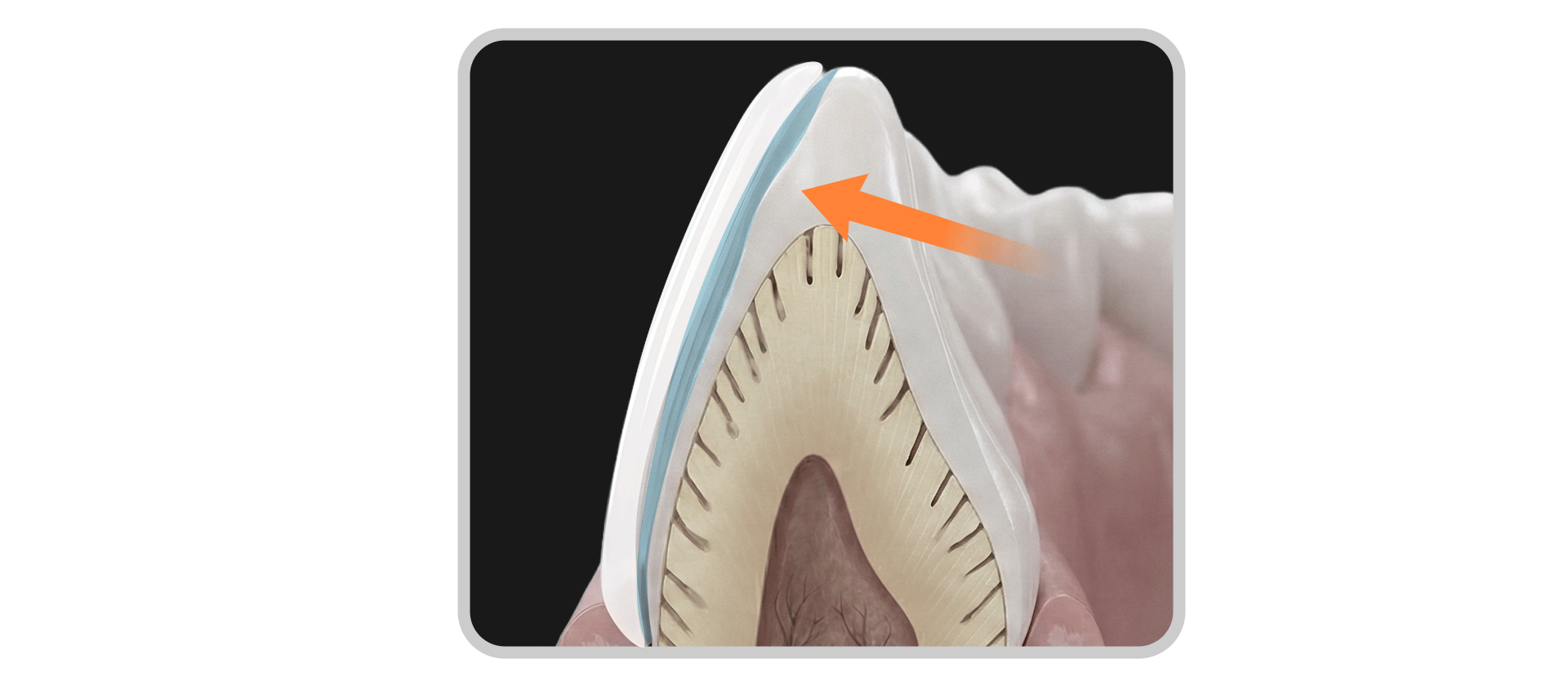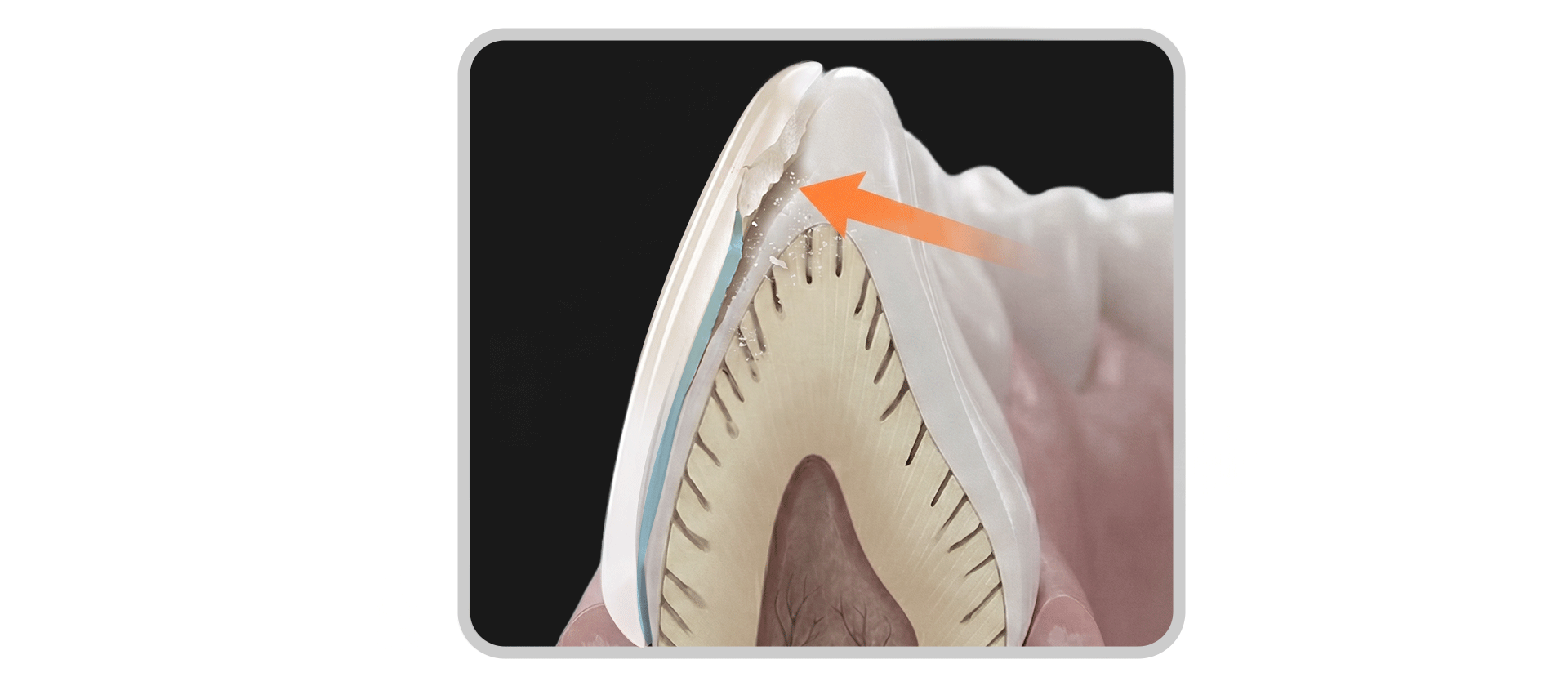
Debonding occurs when the adhesive interface between the tooth and the laminate cannot withstand occlusal forces or external impact. Contrary to popular belief, it is rare for a laminate to fall off entirely in its original shape.
Instead, it more commonly appears as "partial fracture and debonding," where a piece of the restoration chips away upon impact. This is usually the result of cumulative stimulation or an unexpected force, rather than a simple failure of the adhesive alone.
Therefore, the key to preventing debonding and ensuring long-term maintenance is the skill of an experienced medical team that can perfectly manage the bonding process according to the specific situation. Since laminate bonding is a sophisticated process that integrates a very thin porcelain piece with the tooth, the practitioner's expertise significantly impacts the outcome.
3. Why Do Colors Look Different or Become Discolored?
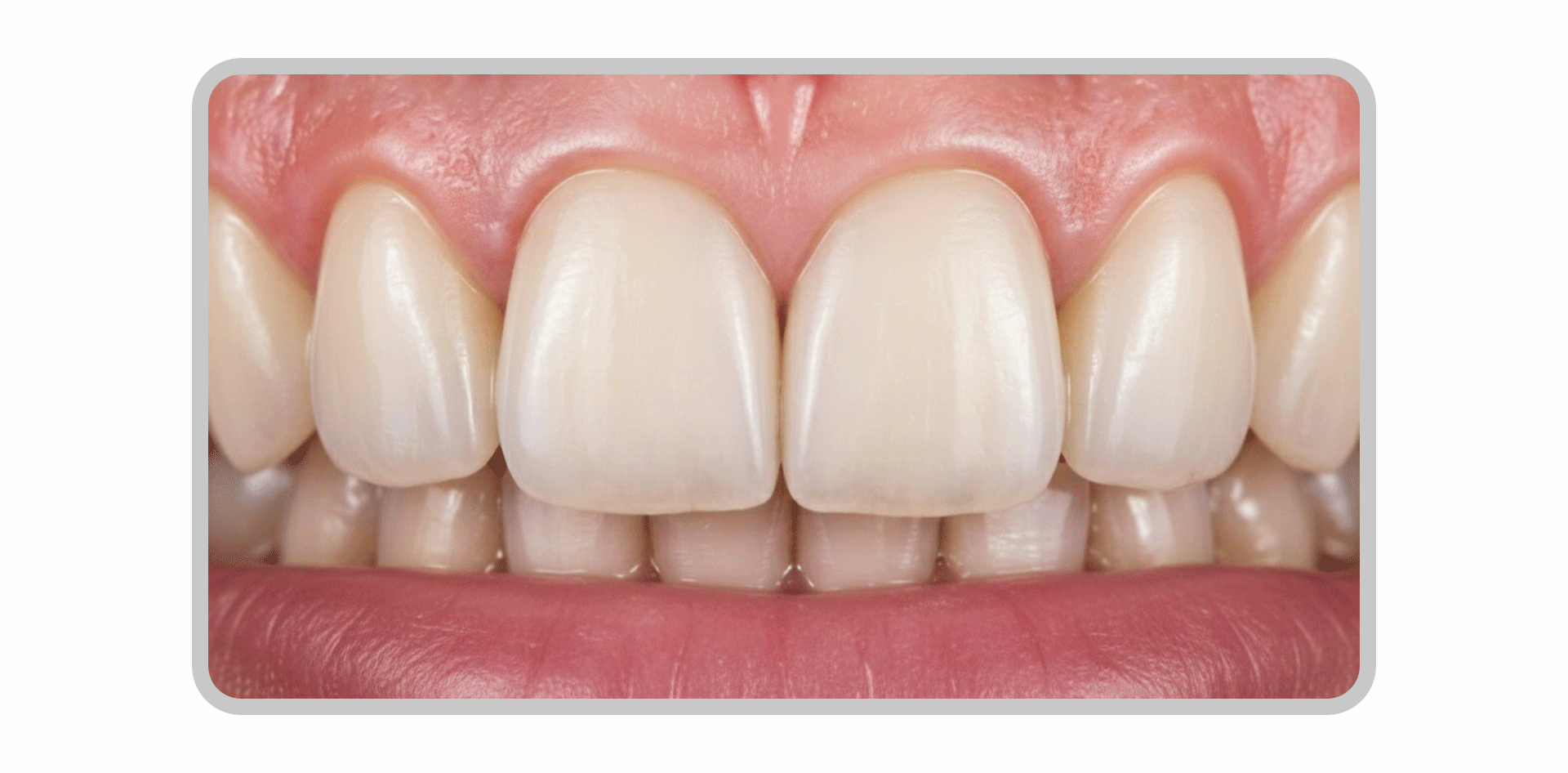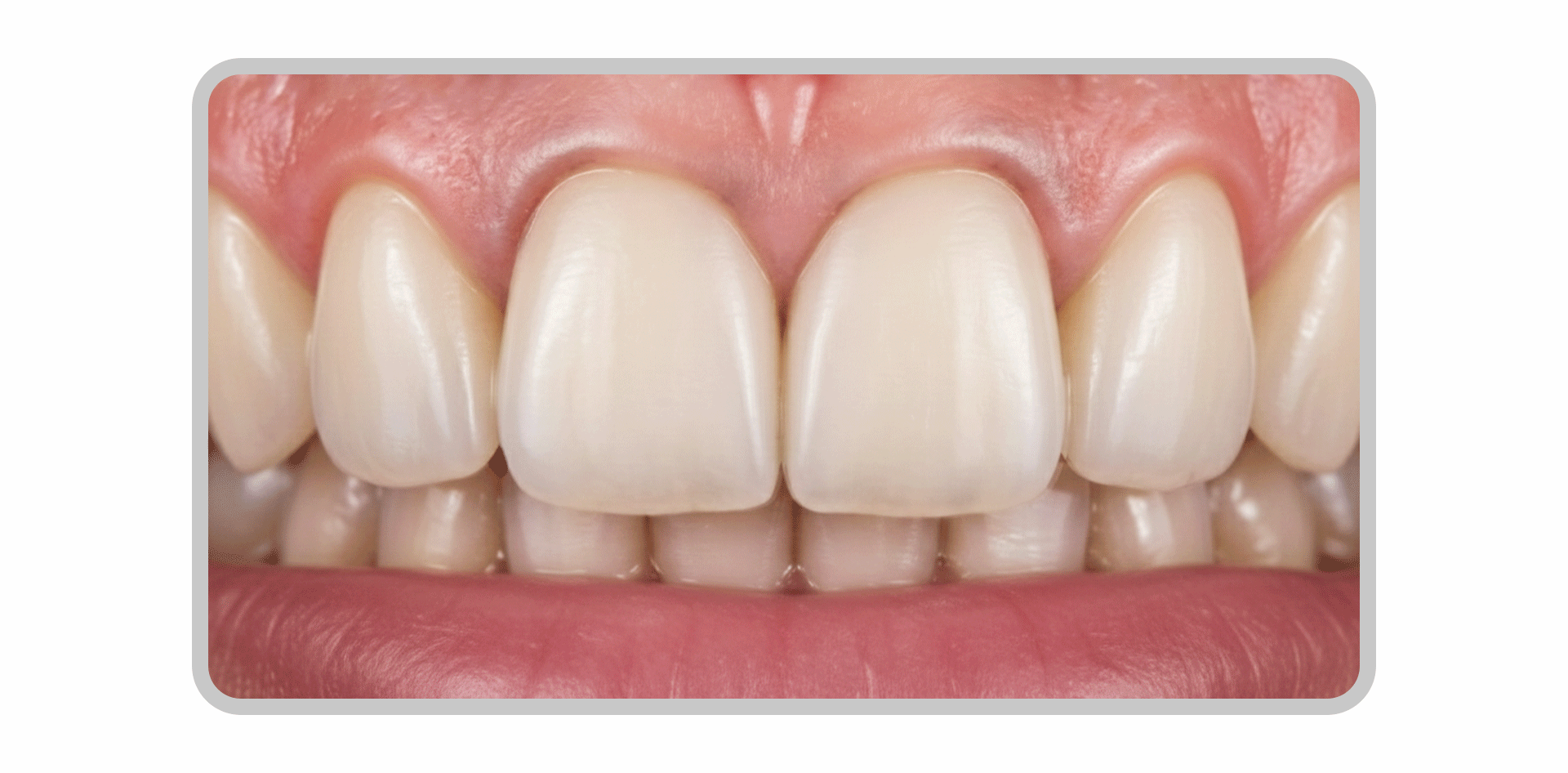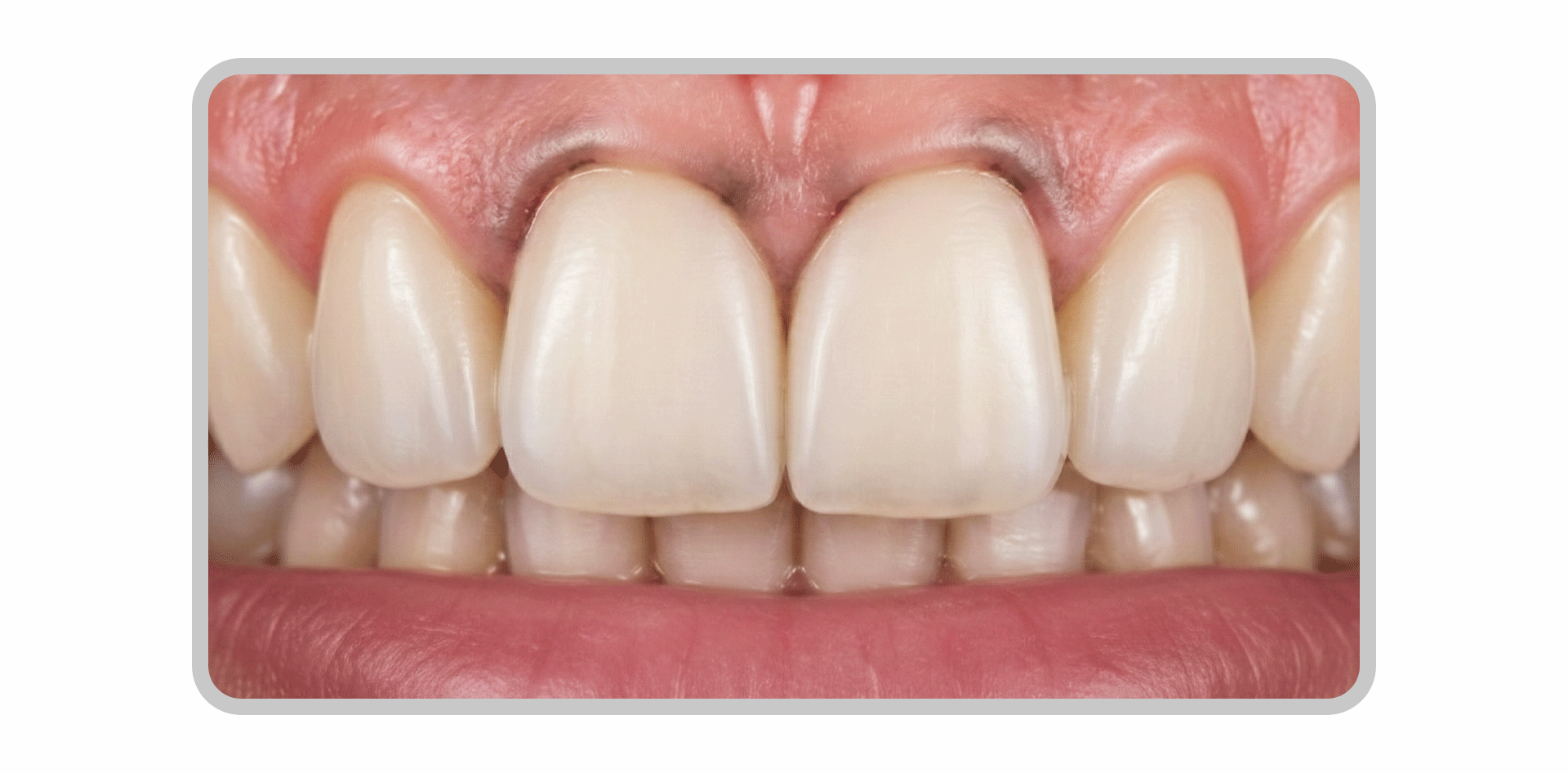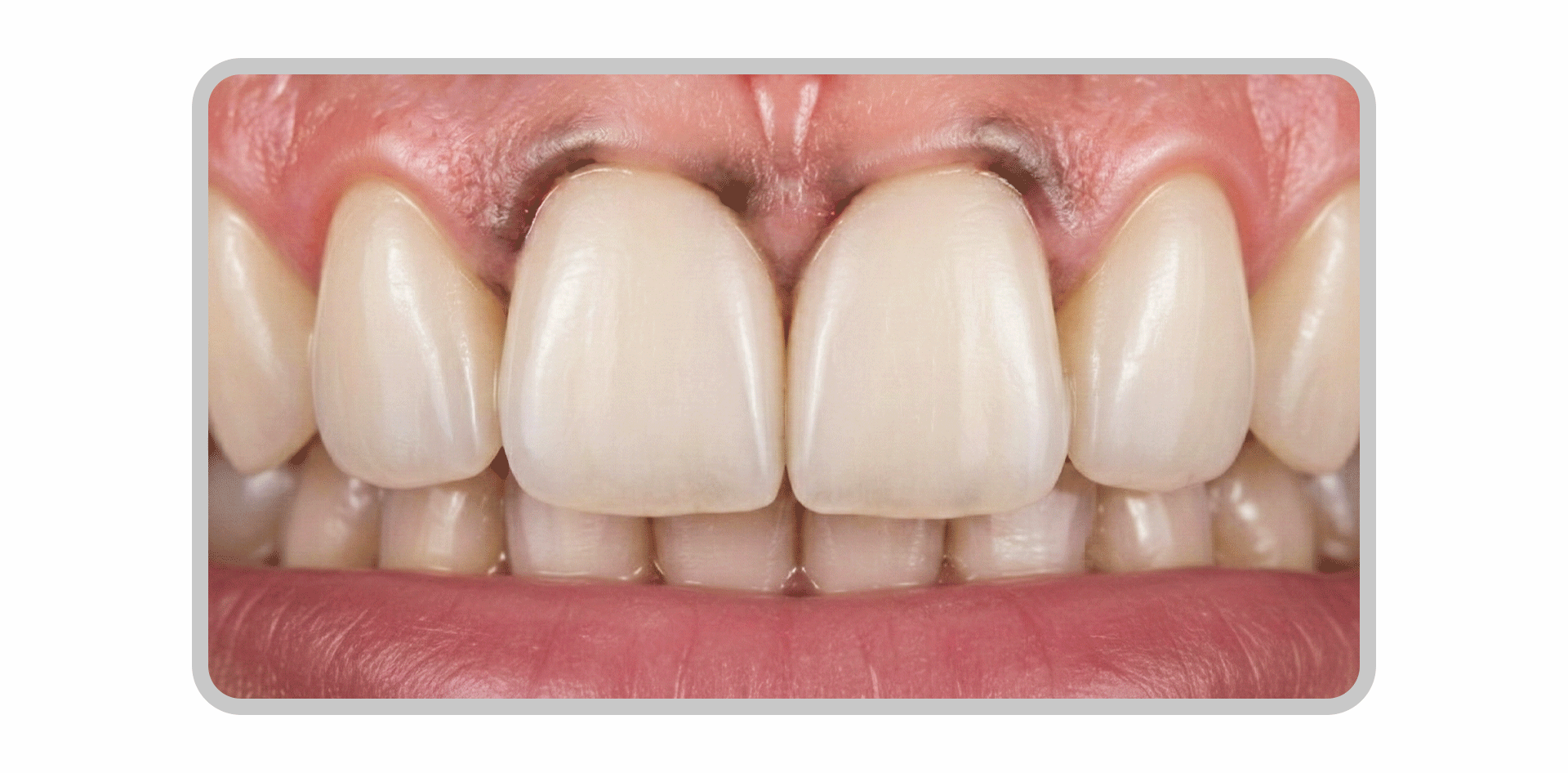
Because laminates are thin, the final shade is influenced not only by the color of the porcelain itself but also by the natural tooth color and the shade of the bonding cement.
While the results may look good immediately after the procedure, the edges may darken over time or develop band-like staining, known as marginal discoloration.
Primary Causes of Discoloration or Color Mismatch:
- Passage of Time: Aging of the bonding cement or microscopic gaps at the margins where pigments can seep in.
- Lifestyle Habits: Frequent consumption of highly pigmented foods like coffee, tea, or curry, or accumulated exposure to smoking.
- Original Tooth Shade: If the natural tooth is significantly dark or severely discolored, a thin laminate may not fully mask the underlying shade, leading to a result different from expectations.
To minimize color issues, target shades should be verified through a "try-in" (color simulation) before final placement. Afterward, plaque around the margins must be managed consistently with flossing and interdental brushes. It is realistic to view long-term color maintenance as a product of daily habits rather than just the procedure itself.
4. Is No-Prep Laminate Truly "Just Stick and Go"?
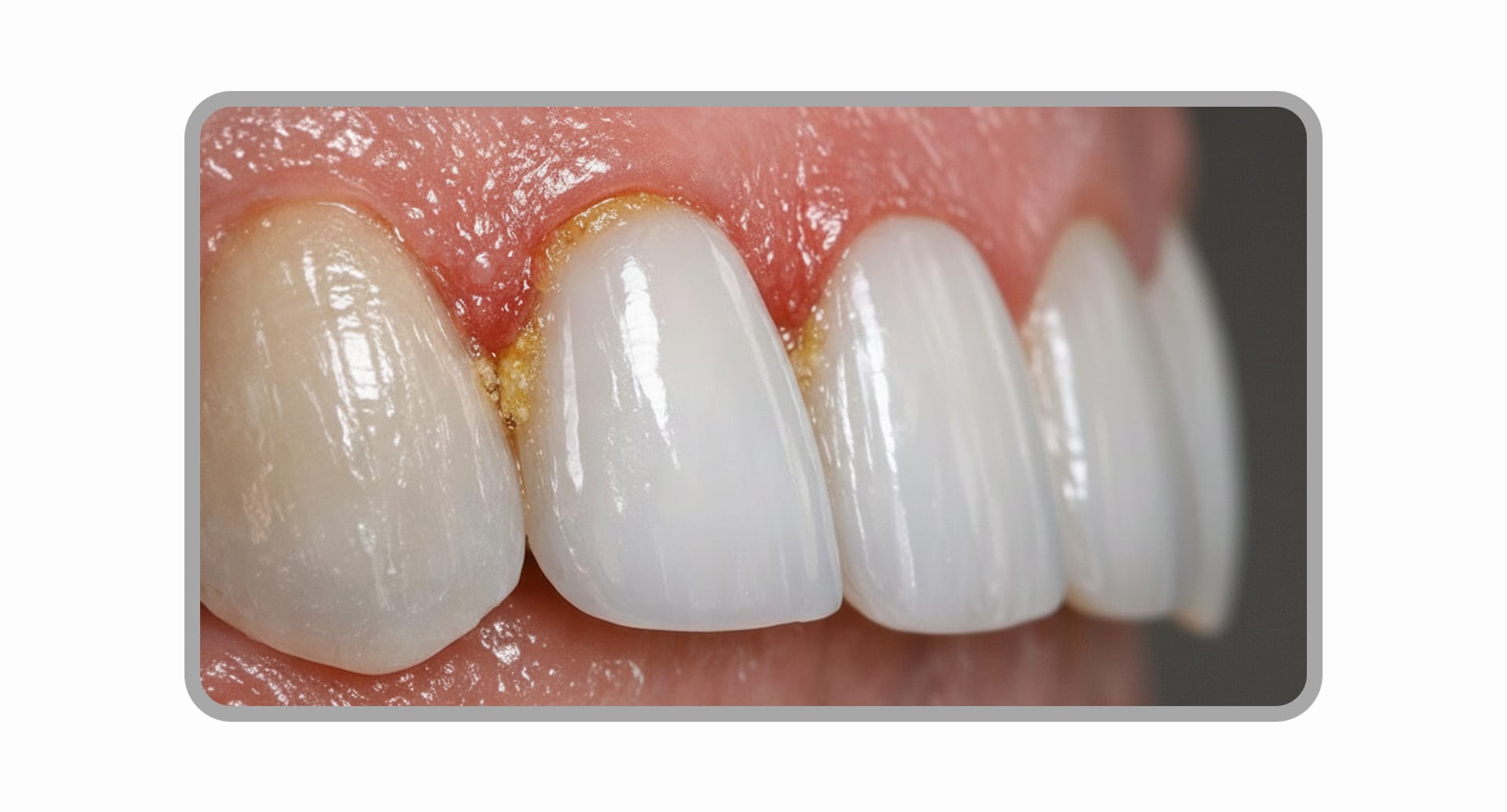
No-prep laminates are attractive because they do not require tooth reduction, but their application is very limited. Adding porcelain without removing any tooth structure inevitably increases the volume of the tooth, which can lead to several problems.
Common Issues with No-Prep Laminates:
- Gum Health Issues: If the restoration protrudes at the gum line (over-contouring), food particles can easily get trapped, leading to plaque buildup, gum inflammation, or bad breath.
- Aesthetic Limitations: If applied to misaligned or protruding teeth without reduction, the result is likely to look thick, bulky, and unnatural.
To use an analogy: forcing thick clothes into a closet that has no space will prevent the door from closing. Similarly, placing porcelain on a tooth without sufficient space or reduction can compromise both aesthetics and gum health. No-prep should only be carefully considered for cases where "adding volume still results in a natural shape," such as microdontia (undersized teeth) or wide gaps between teeth.
5. Frequently Asked Questions (FAQ)
Q. What is the first thing I should do to reduce the risk of chipping?
It is most important to stop using your front teeth as tools, such as biting hard objects or tearing open packages. If you suspect you grind or clench your teeth, consult your dentist about using a protective occlusal guard.
Q. If a laminate falls off, must I always get a new one made?
If the cause is a bonding environment issue and the restoration is intact, rebonding may be possible. However, if the restoration or the tooth is damaged, a replacement will be necessary. An evaluation at the clinic is required first.
Q. What should I do if my teeth remain sensitive for a long time after the procedure?
Initial sensitivity can be temporary, but if it persists or the pain worsens, the pulp or the margins must be checked. Since this varies by individual, a professional examination is necessary.
Q. When should I seek an urgent dental consultation?
You should visit the clinic if the laminate feels loose, if you feel a chipped edge, if you experience pain while chewing, or if the margins suddenly darken or are accompanied by gum swelling and bleeding.

Laminate failure typically manifests in predictable forms such as chipping, debonding, marginal discoloration, or sensitivity, and the prevention points are clear. The keys to reducing risk are minimal-prep techniques that preserve enamel, precise bonding processes, and an evaluation of occlusion and habits. No-prep laminates are a limited option suitable only for specific tooth conditions. For younger patients, it is important to judge the treatment from a long-term perspective, considering tooth preservation and the potential for future replacement. Creating and following a plan tailored to your tooth condition and lifestyle is the most realistic way to avoid regret.
Sources
- Korea Disease Control and Prevention Agency (KDCA). Guide to Laminate Treatment and Aftercare, 2024.
- Seoul National University Hospital Medical Information. Patient Guide for Anterior Porcelain Bonded Restorations (Laminates), 2024.
- Alenezi, A., et al. "Long-term survival and complication rates of porcelain laminate veneers in clinical studies: A systematic review." Journal of Clinical Medicine, 2021.
※ The copyright for all content on this blog belongs to medihi. Unauthorized copying, distribution, or derivative use is strictly prohibited, and violations may result in legal action without prior notice.
Recommended reads